Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista de Gastroenterología del Perú
versión impresa ISSN 1022-5129
Rev. gastroenterol. Perú v.32 n.2 Lima abr./jun. 2012
REPORTE DE CASOS
A novel endoscopic treatment of pancreas divisum
Un tratamiento endoscópico nuevo para el páncreas divisum
Everson L. A. Artifon1, Mariana S. V. Frazão2, Flávio Coelho Ferreira3, José Pinhata Otoch4
1. Associate Professor of Medicine University of Sao Paulo, Sao Paulo, Brazil.
2. Gastrointestinal Endoscopy Unit resident, University of Sao Paulo, Sao Paulo, Brazil.
3. Gastrointestinal Endoscopy Unit resident, University of Sao Paulo, Sao Paulo, Brazil.
4. Associate Professor of Medicine, University of Sao Paulo, Sao Paulo, Brazil.
RESUMEN
El páncreas divisum es la malformación congénita más común del páncreas que resulta de la no fusión ó fusión incompleta de las porciones ventral y dorsal del páncreas embrionario. Se encuentra en 7% de los estudios de autopsias (rango 1-14%), siendo generalmente asintomática. Un 5% de estos pacientes presentan síntomas, que son básicamente dolor abdominal y casos de pancreatitis recurrente. Se reporta el caso de una paciente mujer de 52 años, con 2 episodios de pancreatitis postcolecistectomía con imagen por colangioresonancia de páncreas divisum con comunicación entre el páncreas dorsal y ventral. Se procedió a dilatar el conducto mayor; y luego se hizo una papilotomia del conducto menor y se pasó un balón hidroneumático hasta más allá de su diámetro mayor. El procedimiento ha tenido éxito en 9 meses de seguimiento.
PALABRAS CLAVE: Páncreas Divisum, Colangiopancreatografia endoscópica retrograda, Terapia endóscópica.
ABSTRACT
Pancreas divisum is the most common congenital malformation of the pancreas that results from the non-fusion or incomplete fusion of the ventral and dorsal portions of the embryonic pancreas. It is found in 7% of autopsy studies (range 1-14%) and is generally asymptomatic. 5% of the patients have symptoms, which are basically cases of abdominal pain and recurrent pancreatitis. We report the case of a woman of 51y, postcholecystectomy with 2 episodes of pancreatitis with imaging from magnetic resonance of pancreatic divisum with communication between the dorsal and ventral pancreas. We proceeded by endoscopy (ERCP) to dilate the major duct, and then made a minor duct papillotomy and made a hydropneumatic ball dilatation with the catheter balloon up the waist portion. The procedure was successful with 9 months of follow up.
KEYWORDS: Pancreas divisum, endoscopic retrograde cholangiopancreatography, endoscopic therapy.
INTRODUCTION
Pancreas divisum is the most common con-genital pancreatic anatomical variant, usually asymptomatic, occurring in approximately 7% of the autopsies (range 1% -14%).1 Endoscopic or surgical treatment is indicated in symptomatic patients after a complete investigation and exclusion of other causes of abdominal pain and acute pancreatitis.2,3
The authors intend to demonstrate a new technique of minor papilloplasty, through the major papilla, performed antegradely in a patient with pancreas divisum and acute recurrent pancreatitis.
CASE REPORT
A 51 year-old, female, with previous history of colecistectomy presented two episodes of acute pancreatitis on a period of two months. Magnetic resonance cholangiopancreatography demonstrated dilation of the intrahepatic bile duct, without evidence of stones or strictures and dilation of main pancreatic duct with communication between dorsal and ventral pancreas. Laboratory findings included a high direct bilirubin of 2.8 mg/dL and amylase of 290 U/dL.
After multidisciplinary discussion, it was decided to perform endoscopic retrograde cholangiopancreatography with dilation of the major papilla.
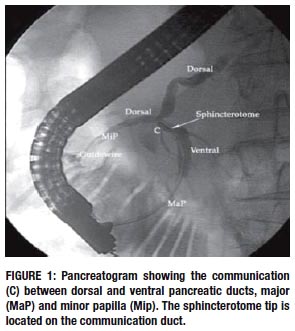
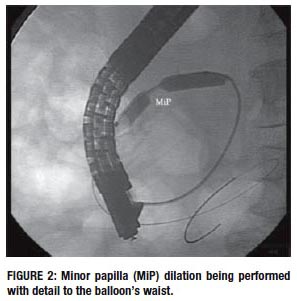
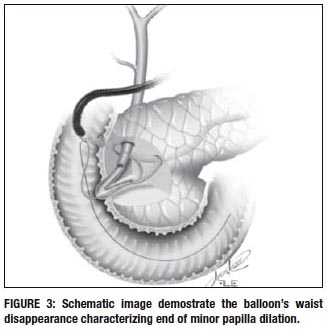
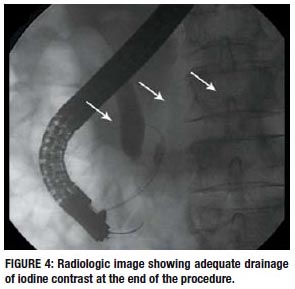
A thin and soft catheter was used while exposing the tip end of the guidewire to facilitate canullation of dorsal pancreatic duct. Dye spraying can improve the view of the minor papilla ostium. After minor papillotomy, a dilatation with a 6mm x 30mm hydrostatic balloons was performed until balloons waist disappearance. If during the exam it is clear that there is good clearance of the contrast injected, pancreatic stenting can be avoided, as it was on this patient.
No immediate or late complications were observed during the 9 months follow-up. The laboratory exams demonstrated to be normal after the procedure.
DISCUSSION
Pancreas divisum is a congenital anomaly caused by a failure of fusion of the ventral and dorsal buds during the embryologic period. Therefore, the drainage of these glands are made separately into the duodenum.4
The anomaly is classified as complete when there is no communication between the ventral and dorsal ducts and incomplete when is a narrow communication between the ventral and dorsal.2,3,5 The clinical presentation as well as its relevance is similar in both forms, and symptomatic cases represent only 5%. The incomplete variant in 15% of the cases.2-5
Patients with mild symptoms can be managed conservatively. However, those with recurrent acute pancreatitis, chronic pancreatitis or pancreatic-type abdominal pain may require treatment that focuses on decompression and drainage of the dorsal duct, performed endoscopically or surgically. Both therapies are effective in reducing episodes of acute pancreatitis and pain relief in approximately 80% of patients. Lower rates of response occur in cases of chronic pancreatitis and pancreatic pain, 70% and 55% respectively.6
Several techniques to access the dorsal duct have been described and includes: canullation with a tapered 3F or 5F catheter and a 0.018-inch diameter guidewire followed by guidewire exchange and dilation of the papilla, stent placement, and then over the stent papillotomy. Regardless of the technique, the access is not successful in 10% of the cases, even in the hands of experienced endoscopists.7,8
This case allowed us to demonstrate a new technique for the treatment of pancreas divisum in its incomplete form. Feasible alternative, allows antegrade access to the papilla minor through papilla major catheterization. We did not observe complications for a period of 9 months. This option of treatment should be discussed with the patient, family and surgeons.
REFERENCES
1. SMANIO T. Proposed nomenclature and classifi cation of the human pancreatic ducts and duodenal papillae: study based on 200 post mortems. Int Surg. 1969; 52:125-134.
2. BENAGE D, MCHENRY R, HAWES RH. Minor papilla cannulation and dorsal ductography in pancreas divisum. Gastrointest Endosc. 1990;36:553-557.
3. MOREIRA VF, MERONO E, LEDO L, et al. Incomplete pancreas divisum. Gastrointest Endosc. 1991;37:104-107.
4. QUEST L, LOMBARD M. Pancreas divisum: opinio divisa. Gut 2000; 47: 317–319.
5. NG JWD, WONG MK, HUANG J, et al. Incomplete pancreas divisum associated with abnormal junction of the pancreatobiliary duct system. Gastrointest Endosc. 1992;38:105-106.
6. Z. LIAO, R. GAO, W. WANG, Z. YE, et al. A systematic review on endoscopic detection rate, endotherapy, and surgery for pancreas divisum. Pancreas. 2007; 34: 21-46.
7. COTTON PB. Congenital anomaly of pancreas divisum as cause of obstructive pain and pancreatitis. Gut. 1980;21:105-115.
8. KLEIN SD, AFFRONTI JP. Pancreas divisum, an evidence based review: Part I, pathophysiology. Gastrointest Endosc. 2004;60(3):419-425.













