Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista de Gastroenterología del Perú
versión impresa ISSN 1022-5129
Rev. gastroenterol. Perú vol.34 no.1 Lima ene. 2014
Artículo de revisión
Difficult cannulation: what should I do before EUS guided access?
Canulación difícil: ¿qué hacer antes de acceso guiado por EUS?
Everson L.A. Artifon 1,2, Renata N. Moura 3, Jose P. Otoch 4
1 Servicio de endoscopia, Hospital Ana Costa. Sao Paulo, Brasil.
2 Sector de endoscopía biliopancreática, Servicio de endoscopía, Hospital de Clínicas, Universidad de San Paulo. Sao Paulo, Brasil.
3 Advanced Fellow del Servicio de Endoscopía del Hospital de Clínicas de la Universidad de Sao Paulo. Sao Paulo, Brasil.
4 Profesor de la Universidad de Sao Paulo. Sao Paulo, Brasil.
ABSTRACT
Selective cannulation of the common bile duct can be difficult, so multiple strategies have been developed to overcome the situation. In this review we analize the different strategies that can be used like different papillotome instead of the standard catheter, precut papillotomy using precut needle knives or precut papillotome, transpancreatic papillary septotomy, and stenting of the pancreatic duct. Bile duct cannulation remains an important benchmark of successful ERCP. Alternative biliary access indication and its use is very important If biliary cannulation remains unsuccessful.The suprapapillary puncture is a promissory technique. It´s important to have in mind that the goal of all techniques is to provide acute pancreatitis decrease. .
Key words: Cannulation; Endoscopic papillotomy; Pancreatitis, acute necrotizing (source: MeSH NLM).
RESUMEN
La canulación selectiva del conducto biliar común puede ser difícil por eso se han desarrollado diferentes estrategias para disminuir esta dificultad. La presente revisión analiza el uso de papilótomos diferentes en lugar del catéter estándar, la papilotomía con pre corte usando cuchillos o papilótomos, la septotomía papilar transpancreática y el uso de stents. La canulación biliar sigue siendo el factor más importante para considerar una ERCP como exitosa. Las indicaciones de accesos biliares alternativos y su uso es muy importante si esta falla. La punción suprapapilar es una técnica promisoria. Es importante tener en cuenta que la meta de todas las técnicas es disminuir la ocurrencia de pancreatitis aguda.
Palabras clave: Canulación; Papilotomía endoscopica; Pancreatitis aguda necrotizante (fuente: DeCS BIREME).
INTRODUCTION
Endoscopic retrograde cholangiography (ERCP) is a technically-demanding procedure and an important tool in diagnosis and therapy of benign and malignant disorders of the biliary tree (1).
The ability to selectively cannulate the bile duct quickly and a traumatically is the key to successful therapeutic ERCP, and to minimizing post-ERCP complications, especially pancreatitis (PEP) (2).
The selective cannulation of the common bile duct is a difficult procedure, the success of which mainly depends on the skills of the examiner but also on the anatomical variants and the underlying illnesses (1).
The access can usually be overcome by using basic anatomic principles to optimize endoscope position and cannula axis, and by selecting accessories based upon identified challenges (3).
The clinical success of a procedure is determined by the balance between clinical efficacy, technical success, and adverse events (4).
Skilled biliary specialists achieve successful cannulation 95% to 99% of the time while experienced community endoscopists should reach cannulation rates above 90% (3). However, selective bile duct cannulation can fail in up to 10% of patients, with an increased risk of post-ERCP pancreatitis.
CRITICAL ANALYSIS OF THE ACCESORIES FOR CONVENTIONAL CANNULATION
A variety of instruments and techniques exist to achieve selective common bile duct (CBD) cannulation, including use of a standard or tapered catheter, sphincterotomes, performance of pre-cut papillotomy, and the use of guidewires (5).
Most catheters used for ERCP are 5F to 7F in diameter and can accept guide wires up to 0.035 in in diameter. Regular cannulas with or without guide wires can be difficult to use because the angle of approach cannot be varied. Standard papillotomes are widely used for cannulation (4).
A randomized trial comparing the success of biliary access using a sphincterotome with that of a regular cannula found, in 100 patients, that a sphincterotome
without a guidewire was successful in 84% using a sphincterotome compared with 62% using a standard cannula (p<.05) (6).These findings were confirmed in another randomized trial in which biliary cannulation was successful in 97% of patients using a sphincterotome compared with 67% using a standard catheter (p<.05). The use of a sphincterotome was associated with fewer cannulation attempts and shorter cannulation times (5).
Rotatable papillotomes are widely used now, which allow the endoscopist to match of the angle of approach of the papillotome to the specific course of the bile duct within the papilla. These devices may improve cannulation in surgically altered anatomy, distorted and peridiverticular papillas, or unusual angulation of the bile duct (4).
A randomized trial of conventional cannulation technique using sphincterotome and contrast injection versus guide wire cannulation technique has been conducted by Artifon et al and demonstrated that guide wire cannulation was associated with significantly lower likelihood of post-ERCP pancreatitis (p<.05) by facilitating cannulation and reducing need for precut sphincterotomy (7).
A comprehensive list of devices for biliary cannulation and sphincterotomy was published in Gastrointestinal Endoscopy in 2010 (8).
LIMITING FACTORS
There are a lot of possible causes of difficult cannulation (Table 1).
Ampullary diverticulum Periampullary tumor Opie syndrome Biliopancreatic junction Surgically altered anatomy (bariatric surgery, Billroth II) Papillitis Sphincter of oddi dysfunction Small or tortuous papilla Difficult approach to papilla.
The presence of periampullary duodenal diverticula used to be considered a risk factor for failed biliary cannulation. However, most of the time, the papilla remains accessible, often on a side wall of the diverticulum. Difficulty arises when the papilla lies deep within a diverticulum and/or its orientation is unfavorable (2).
The papilla can be difficult to locate in the setting of tumor infiltration of the papilla or the duodenum, or pancreatitis that causes duodenal edema and distortion (4).
Another example is sphincter of Oddi dysfunction. Although the anatomy is preserved, cannulation may be challenging because the sphincter is often stenotic (4).
Esophageal, gastric outlet and duodenal strictures create access difficulty by preventing the endoscope reaching the papilla. It may be necessary to dilate or even stent such strictures (2).
Occasionally, the main duodenal papilla in located in the third (D3) or even the fourth (D4) part of the duodenum.
Another anatomical rearrangement that presents technical challenges for ERCP is the Roux-en-Y biliary diversion performed in the latest iteration of bariatric (weight loss) surgery. Typically, the papilla cannot be reached with a standard duodenoscope, due to the considerable length of the Roux diversion.
The papilla can sometimes be reached with a colonoscope, and more reliably with single- and double balloon enteroscopes However, these instruments do not have elevators with which cannulas can be manipulated, and there is a paucity of suitable accessories, such as papillotomes, baskets, and balloon catheters, that can be used through these longer-thanstandard endoscopes (2).
In 2013, Choi et al compared indications and outcomes between ERCP via gastrostomy (GERCP) versus double balloon enteroscopy (DBERCP) to access the pancreatobiliary tree in patients with prior bariatric Roux-en-Y gastric bypass surgery (RYGB). They concluded that GERCP is more effective than DBERCP in gaining access to the pancreatobiliary tree in patients with RYGB, but it is hindered by the gastrostomy maturation delay and a higher morbidity (9). Nevertheless, technical improvements in each method are needed.
“TRICKS” FOR CANNULATION
Using pancreatic duct techniques to facilitate biliary cannulation is becoming increasingly popular. An advantage of this approach is that a pancreatic duct stent can be placed to reduce the likelihood of pancreatitis in the setting of difficult biliary cannulation (4).
Over the last decade, the placement of small caliber stents in the PD has been recognized as the most effective technique identified to date to prevent the development of post-ERCP pancreatitis (PEP) (2).
The efficacy and safety of biliary cannulation after pancreatic duct wire placement was assessed in a randomized trial of 53 patients in whom biliary cannulation failed after 10 minutes. The patients were then randomized to further attempts using biliary techniques versus pancreatic duct wire placement followed by repeat attempts at biliary cannulation. Successful cannulation was achieved in 93% when using the pancreatic wire, compared with 58%in the standard biliary techniques group (P<.05). No differences in pancreatitis were observed, although the amylase tended to be higher when using pancreatic duct access technique (10).
Another group using pancreatic wire-assisted biliary cannulation in 32% of all ERCPs requiring biliary access reported no difference in complications when compared with easy conventional cannulation (mild pancreatitis in 7.8%and 8.3%, respectively) (11).
These findings were confirmed by Sherman et al suggesting that leaving a pancreatic duct stent in place following needle-knife sphincterotomy reduced the pancreatitis rate from 21.3% to 2.2% (12).
A variety of “tricks” may have to be tried to obtain a view of the papilla from which it can be cannulated. The tip of the duodenoscope may have to be negotiated inside the diverticulum, which risks injury and possible perforation. Blind probing of the diverticulum with guide wires and catheters is even more dangerous, and should be avoided. Advancing the duodenoscope into the “long position” is one way to alter its orientation to the diverticulum and the papilla within (2).
Though a lot of strategies have been developed to facilitate selective cannulation of the common bile duct and to prevent the major complication of difficult ERCPs, little is known about the factors responsible for the difficulty to gain access to the common bile duct. Variables related to the anatomy of the patient and the papilla can be used to predict success or failure (1).
Papilla-related factors for the successful selective cannulation of the common bile duct (CBD) was assessed in 50 patients with a papilla with no prior sphincterotomy needing an ERC and suggests that the typical position of the duodenoscope is the single most important factor determining success. The combination of two variables—typical position of duodenoscope and visible orifice—has a positive predictive value of 96%. These variables can be evaluated easily at the beginning of the procedure and can be used by the examiner to quickly predict success (1).
DIFFICULT CANNULATION
We can define difficult cannulation depending on the time taken to achieve deep cannulation of the bile duct (more than 5 minutes) or the number of cannulation of the pancreatic duct (PD) while accessing the biliary tree (more than 10 attempts).
Quick, atraumatic access is the ideal, but this is not always possible, even for experts. Repeat cannulation of the PD when the bile duct is the intended target invites PEP; there is a direct (linear) relationship between the number of PD instrumentations and the likelihood of this complication, especially if contrast medium is repeatedly injected (1).
OPTIONS FOR BILIARY ACCESS
• Pre-cut
Precut papillotomy can be accomplished by a variety of techniques, the success and complications of which heavily depend on technique-related factors and the risk profile and anatomic variations of the patient. In particular, the skill of the endoscopist, the indication for the procedure, and the use of pancreatic stents all influence the outcome of this procedure (4).
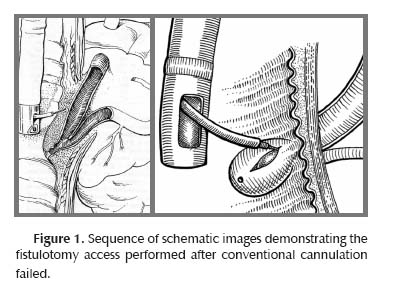
Precut papillotomy when performed as a rescue measure is widely considered as the procedure of choice and improves the success rate of ERCP to 95% to 98% at expert centers (13). (Figure 1).
The decision to use a precut technique relies on a variety of factors. For example, one group reported that this technique was more necessary in unusual or distorted anatomy of the papilla, such as in the case of duodenal stenosis or malignancy (4).
In a randomized study of 103 patients with choledocholithiasis, needle-knife fistulotomy was compared with needle-knife precut papillotomy. Precutting was successful in 90.54% of patients in the needle-knife fistulotomy group and 88.6% of patients in the needle-knife precut papillotomy group. Both methods were effective in the management of choledocholithiasis. When needle knife fistulotomy is performed, however, lithotripsy is needed more often. Needle-knife fistulotomy was safer than needleknife precut papillotomy with respect to pancreatic complications (14).
• Transpancreatic sphincter pre-cut
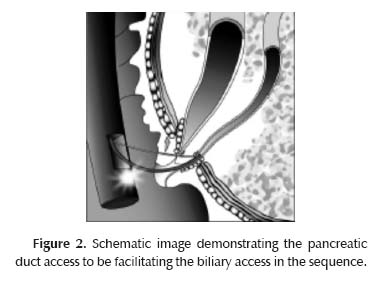
A more common technique, known as “transpancreatic precut sphincterotomy,” involves intentional seating of a standard papillotome into the pancreatic duct and making a transseptal incision to access the bile duct.The transpancreatic duct pre-cut to gain access to the bile duct for diagnostic and therapeutic maneuvers has been described as useful. To further evaluate this technique, Goff et al performed a review on 200 consecutive endoscopic sphincterotomies. Precutting was successful in 96% of patients. The overall complication rate for the standard sphincterotomy was 2.1%; that for the transpancreatic approach was 1.96%. There were no cases of post-ERCP pancreatitis after transpancreatic duct pre-cut sphincterotomy (15). (Figure 2).
• Papillary needle puncture The suprapapillary needle-puncture is a novel technique with a successful over than 90% in selective biliary cannulation, requiring less than 5 minutes for cannulation and associated with minimal complication rate and no mortality (16).Selective cannulation of the bile duct by using suprapapillary needle puncture of the bile duct followed by balloon dilation of the tract avoids potential mechanisms that precipitates pancreatitis associated with conventional transpapillary biliary cannulation and endoscopic sphincterotomy (16).
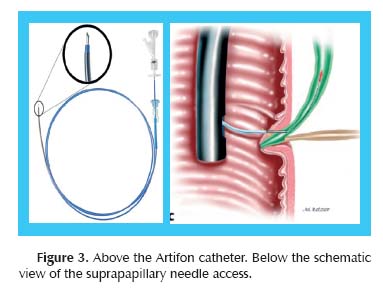
Direct mechanical injury to the pancreatic duct orifice from repeated probing of the ampulla is avoided by aiming the entry in the suprapapillary portion of bile duct. Chemical, allergic, and hydrostatic injury to the pancreatic duct from inadvertent injection of contrast into the pancreatic duct is eliminated by totally avoiding the pancreatic-duct injections and selectively injecting into the bile duct only after confirmation of the position of the guide wire in the bile duct. Thermal injury from conventional biliary sphincterotomy is also avoided, because balloon dilation of the puncture tract is used to enlarge the orifice for removal of stones. Avoiding several of these potential mechanisms that precipitate post-ERCP pancreatitis by using the suprapapillary puncture technique could reduce the risk of post-ERCP pancreatitis (16). (Figure 3).
Potential applications of papillary needle puncture are showed on Table 2.
CURRENT ALTERNATIVES FOR BILIARY CANNULATION
Some endoscopists may be unfamiliar with some of the newer devices and techniques. Many of these techniques can be successfully applied, and disagreement as to the most appropriate technique may exist even among experts. This is further amplified by lack of comparative data available to generalize various techniques outside of centers where such studies are performed. Inferences about relative safety and efficacy of one technique over another are limited because complications can depend on patients’ susceptibility as much as the specific technique used by the endoscopist (4).
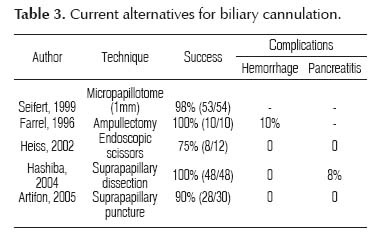
Current alternatives for biliary cannulation and their respective success rate and complications are shown in Table 3.
Failed biliary cannulation has been traditionally managed with percutaneous transhepatic biliary drainage (PTBD) or surgery. The potential complications associated with these procedures, along with the patient dissatisfaction associated with external drainage make these options less desirables. EUS-guided cholangiopancreatography followed by biliary drainage (BD) has been performed with many case reports and series confirming both the success and safety of this technique.
EUS-guided rendezvous drainage of the bile duct can be performed in the endoscopy room in the same session and involves gaining access to the biliary tree via the duodenum or stomach by using a 19-gauge needle (13).
The efficacy and safety profile of the EUS-guided rendezvous technique with use of the short wire system and a comparison of the clinical outcomes with patients who underwent precut papillotomy for biliary access were evaluated in a retrospective study. Treatment success was significantly higher for the EUS-guided rendezvous than for those undergoing precut papillotomy technique (98.3% vs 90.3%; p <.03). There was no significant difference in the rate of procedural complications between the EUS and precut papillotomy techniques (3.4% vs 6.9%, p <.27) (13).
CONCLUSIONS
Selective cannulation of the common bile duct can be difficult, so multiple strategies have been developed to overcome the situation: different papillotome instead of the standard catheter, precut papillotomy using precut needle knives or precut papillotome, transpancreatic papillary septotomy, and stenting of the pancreatic duct. However, these methods carry a high complication.
Bile duct cannulation remains an important benchmark of successful ERCP. Alternative biliary access indication and its use is very important If biliary cannulation remains unsuccessful.
The suprapapillary puncture is a promissory technique in selective cannulation of the bile duct, while avoiding mechanical, chemical, or thermal injury to the pancreatic duct and avoiding bleeding.
It´s important to have in mind that the goal of all techniques is to provide acute pancreatitis decrease.
REFERENCES
1. Zuber-Jerger I, Gelbman MC, Kullmann F. Visual characteristics of the papilla to estimate cannulation of the common bile duct – a pilot study . N Am J Med Sci. 2009;1(2):66-73.
2. Baillie J. Difficult biliary access for ERCP . Curr Gastroenterol Rep. 2012;14(6):542-7. [ Links ]
3. Petersen BT. Cannulation techniques: biliary and pancreatic. Techniques in Gastrointestinal Endoscopy. 2003;5(1):17-26. [ Links ]
4. Bakman YG, Freeman ML. Difficult biliary access at ERCP . Gastrointest Endoscopy Clin N Am. 2013;23(2):219-36. [ Links ]
5. Cortas GA, Mehta SN, Abraham NS, Barkun AN. Selective cannulation of the common bile duct: a prospective randomized trial comparing standard catheters with sphincterotomes . Gastrointest Endosc. 1999;50(6):775-9. [ Links ]
6. Schwacha H, Allgaier HP, Deibert P, Olschewski M, Allgaier U, Blum HE. A sphincterotome-based technique for selective transpapillary common bile duct cannulation . Gastrointest Endosc. 2000;52(3):387-91. [ Links ]
7. Artifon EL, Sakai P, Cunha JE, Halwan B, Ishioka S, Kumar A. Guidewire cannulation reduces risk of post-ERCP pancreatitis and facilitates bile duct cannulation. Am J Gastroenterol. 2007;102(10):2147-53. [ Links ]
8. ASGE Technology Committee, Kethu SR, Adler DG, Conway JD, Diehl DL, Farraye FA, et al. ERCP cannulation and sphincterotomy devices . Gastrointest Endosc. 2010;71(3):435-45. [ Links ]
9. Choi EK, Chiorean MV, Coté GA, El Hajj II, Ballard D, Fogel EL, et al. ERCP via gastrostomy vs. double balloon enteroscopy in patients with prior bariatric Roux-en-Y gastric bypass surgery . Surg Endosc. 2013;27(8):2894-9. [ Links ]
10. Maeda S, Hayashi H, Hosokawa O, Dohden K, Hattori M, Morita M, et al. Prospective randomized pilot trial of selective biliary cannulation using pancreatic guide-wire placement . Endoscopy. 2003;35(9):721-4. [ Links ]
11. Gyökeres T, Duhl J, Varsányi M, Schwab R, Burai M, Pap A. Double guide wire placement for endoscopic pancreaticobiliary procedures . Endoscopy. 2003;35(1):95-6. [ Links ]
12. Sherman S, Earle DT, Bucksot L, Baute P, Gottlieb K, Lehman G. Does leaving a main pancreatic duct stent in place reduce the incidence of precut biliary sph1ncterotomy (ES)-induced pancreatitis?: A final, analysis of a randomized prospective. Gastrointest Endosc. 1996;43:A489. [ Links ]
13. Dhir V, Bhandari S, Bapat M, Maydeo A. Comparison of EUS-guided rendezvous and precut papillotomy techniques for biliary access (with videos) . Gastrointest Endosc. 2012;75(2):354-9. [ Links ]
14. Mavrogiannis C, Liatsos C, Romanos A, Petoumenos C, Nakos A, Karvountzis G. Needle-knife fistulotomy versus needle-knife precut papillotomy for the treatment of common bile duct stones . Gastrointest Endosc. 1999;50(3):334-9. [ Links ]
15. Goff JS. Long-term experience with the transpancreatic sphincter pre-cutapproach to biliary sphincterotomy . Gastrointest Endosc. 1999;50(5):642-5. [ Links ]
16. Artifon EL, Sakai P, Ishioka S, Hondo FY, Raju GS. Suprapapillary puncture of the common bile duct for selective biliary access: a novel technique (with videos) . Gastrointest Endosc. 2007;65(1):124-31. [ Links ]