Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista de Gastroenterología del Perú
versión impresa ISSN 1022-5129
Rev. gastroenterol. Perú vol.35 no.4 Lima oct. 2015
Surgical or endoscopic management for post-ERCP large transmural duodenal perforations: a randomized prospective trial
Manejo endoscópico o quirúrgico de las perforaciones transmurales duodenales post CPRE. Un estudio randomizado prospectivo
Everson L. A. Artifon.1a,2a, Mauricio K. Minata2,c, Marco Antonio B. Cunha1,b, Jose P. Otoch 2, a, Dayse P. Aparicio 1, b, Carlos K. Furuya 2, b, José L. B. Paione 1
1 Hospital Ana Costa. Santos, Brazil.
2 Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo. São Paulo, Brazil.
a Professor, b Assistant physician, c Resident physician
Abstract
Introduction: Duodenal perforations are an uncommon adverse event during ERCP. Patients can develop significant morbidity and mortality. Even though surgery has been used to manage duodenal complications, therapeutic endoscopy has seen significant advances. Objective: To compare endoscopic approach with surgical intervention in patients with duodenal perforations post-ERCP. Material and Methods: prospective randomized study in a tertiary center with 23 patients divided in 2 groups. Within 12 hours after the event, the patients underwent endoscopic or surgical approach. Endoscopic approach included closure of the perforation with endoclips and SEMS. Surgical repair included hepaticojejunostomy, suture of the perforation or duodenal suture. The success was defined as closure of the defect. Secondary outcomes included mortality, adverse events, days of hospitalization and costs. Results: The success was 100% in both groups. There was one death in the endoscopic group secondary to sepsis. There was no statistical difference in mortality or adverse events. We noticed statistical difference in favor of the endoscopic group considering shorter hospitalization (4.1 days versus 15.2 days, with p=0.0123) and lower cost per patient (U$14,700 versus U$19,872, with p=0.0103). Conclusions: Endoscopic approach with SEMS and endoclips is an alternative to surgery in large transmural duodenal perforations post-ERCP.
Key words: Intestinal perforation; Cholangiopancreatography, endoscopic retrograde; Stents; Surgical clips; Surgical procedures, operative (source: MeSH NLM).
Resumen
Introducción: Las perforaciones duodenales son un evento adverso poco frecuente durante la CPRE. Los pacientes pueden desarrollar morbilidad y mortalidad significativas. La cirugía se ha utilizado para tratar las complicaciones duodenales, pero la endoscopia terapéutica ha visto avances significativos. Objetivo: comparar abordaje endoscópico con intervención quirúrgica en perforaciones duodenales post CPRE. Materiales y Métodos: estudio prospectivo aleatorizado en un centro terciario con 23 pacientes divididos en 2 grupos. 12 horas después del evento, los pacientes fueron sometidos a tratamiento endoscópico o quirúrgico. El abordaje endoscópico incluyó el cierre de la perforación con endoclips y stent metálico autoexpandible. La reparación quirúrgica incluyó hepaticoyeyunostomía, sutura de la perforación o sutura duodenal. El éxito se definió como el cierre del defecto. Los resultados secundarios incluyeron: mortalidad, eventos adversos, días de hospitalización y costos. Resultados: El éxito fue del 100% en ambos grupos. Hubo una muerte en el grupo endoscópico secundaria a sepsis. No hubo diferencia estadísticamente significativa. Hubo una diferencia estadística a favor del grupo endoscópico en vista de la hospitalización más corta (4,1 días frente a 15,2 días, p=0,0123) y menor costo por paciente (U$ 14 700 frente a U$ 19 872, p=0,0103). Conclusión: El abordaje endoscópico es una alternativa a la cirugía en perforaciones duodenales post CPRE.
Palabras Claves: Perforación intestinal; Pancreatocolangiografía retrógrada endoscópica; Stents; Clips quirúrgicos; Procedimientos quirúrgicos operativos (fuente: DeCS Bireme).
Introduction
Duodenal perforations are an uncommon adverse event during endoscopic retrograde cholangiopancreatography (ERCP). While their reported incidence is low (0.1-2.1%), patients can develop significant morbidity and mortality, have longer hospitalization and higher costs (1-4).
Factors that increase the risk of duodenal perforation during ERCP include performing a sphincterotomy, a Billroth II anatomy, intramural injection of contrast, history of sphincter of Oddi dysfunction, dilation of a biliary stricture, malignancy, prolonged procedure and performing a "precut" of the ampulla in order to gain access to the common bile duct (4).
Even though surgery has been commonly used to manage duodenal complications, therapeutic endoscopy has seen significant advances in regards to technique and the availability of instrumentation. The experience with endoscopic management of duodenal perforations is scarce and limited to case reports (5-11). The procedure is normally directed toward closing the defect with clips and other devices like stents and endoloops. There are few studies comparing endoscopic management versus surgical repair of duodenal perforations caused during ERCP.
The aim of this study is to compare the outcomes of endoscopic management with traditional surgery in patients with large transmural duodenal perforations post-ERCP. Endoscopic management included covered SEMS (self-expandable metallic stents) plus clips (Group I or endoscopic) and surgical repair (Group II or surgical) was done within 12 hours of the adverse event. Large was defined as appreciated by endoscopist >5 mm.
The main outcome was the success of the procedure (closure or repair of the defect). Secondary outcomes were: days of hospitalization, mortality at 30 days, complications and costs.
MATERIAL AND METHODS
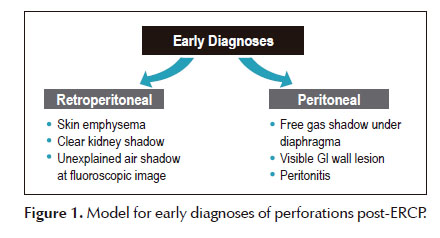
This was a randomized controlled trial including patients that developed large transmural duodenal perforations during an ERCP with visible defect in the duodenal wall (of at least 5mm by endoscopic appreciation) and the presence of pneumoperitoneum and/or retroperitoneal emphysema seen in the fluoroscope or CT image. Early diagnosis of perforation was based on Figure 1.
The study was performed at Hospital Ana Costa (Santos, Brazil), which is a tertiary care level I institution. IRB approval to conduct this prospective study was granted by Hospital Ana Costa.
Patients that met inclusion criteria were admitted to the hospital, placed nothing per mouth, a nasogastric tube was placed, started on a proton pump inhibitor and broad-spectrum intravenous antibiotics (ceftriaxone and metronidazole for 7 days). Patients were selected consecutively for therapy and randomized by using sealed envelopes that were opened just after complications.
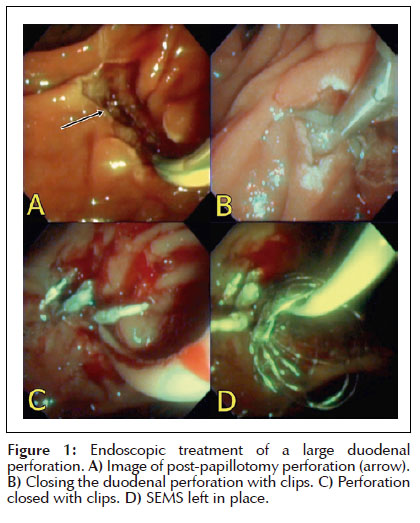
On those patients that underwent surgical management of the perforation an upper endoscopy was performed (video duodenoscope channel 3.2 mm Pentax). First, a partially covered metallic stent (60x10 mm, Boston Scientific, Natick, Massachusetts, United States) was deployed in the duodenum. Then, at least 2 endoclips were deployed from proximal to distal perforated area. The guidewire were left in place deeply in the CBD before clips deployed (Figure 2). All patients had an abdominal computer tomography done 2 and 7 days after the procedure. The duodenal stent was removed after 3 weeks.
The group randomized to the surgery arm, underwent either open or laparoscopic surgical intervention which was decided by the surgeon who performed the procedure; with suture of the perforation, hepaticojejunostomy with Roux in Y or duodenum suture (to access the perforated area, the surgeon had an incision on the duodenum, thus both were sutured).
The statistical analysis was performed with absolute number, and compared using the Student t test. Numeric data were compared using X2 test. Logistic regression analysis was applied to evaluate the success rate of the procedures and the incidence rates of complications. Statistical significances for all tests was set at p<0.05. The sample size was calculated in a non-inferiority study to be 47 patients in each group. After 5 years, the investigators agreed to stop the trial to slow recruitment and concern that the study would not be successfully completed. The final analysis was performed with those patients that had been recruited (23 patients).
RESULTS
Twenty three patients were randomized to have surgery (n=11) or endoscopic management of the perforation (n=12) between March 2007 until April 2013. The mean age were 69.7 and 63.9 to the groups I and II, respectively. In the endoscopic group there were 5 peritoneal (41.6%) and 7 retroperitoneal perforations (58.3%). In the surgical group we noticed 4 peritoneal (36.3%) and 7 retroperitoneal perforations (63.6%), without statistical significance. The baseline characteristics of the both group of patients are shown on Table 1, including the type and size of duodenal perforation.
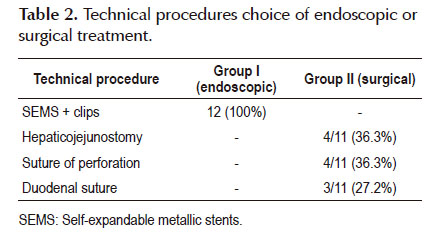
Table 2 shows the procedure performed in each group. All 12 patients on Group I underwent SEMS with endoclips. In Group II 4 (36.3%) had hepaticojejunostomy; 4(36.3%) suture of the perforation and 3 (27.2%) duodenal suture.
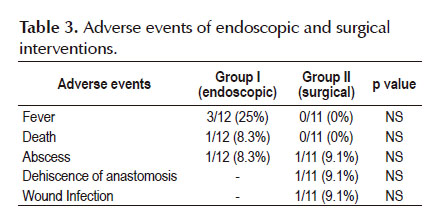
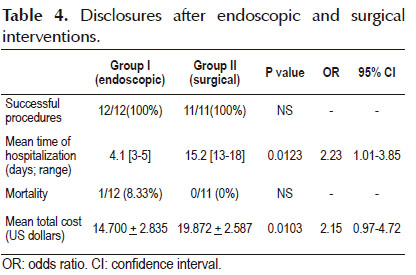
Tables 3 and 4 shows the adverse events and disclosures. The success was 100% in both groups, defined as closing the defect or perforation. In the endoscopic treatment group, there was one case of retroperitoneal abscess treated with percutaneous drainage guided by conventional ultrasound, three cases of fever treated with antibiotics and antipyretics and one death (still mortality was non-significant in both groups). The mortality case was an 84 years old patient with several comorbities, American Society of Anesthesiologists (ASA) 5 that died secondary to sepsis. In the surgical intervention group, there was one case of abscess treated with percutaneous drainage guided by conventional ultrasound, one case of dehiscence of anastomosis that required reoperation and one case of wound infection submitted to debridement.
Other important variables included a shorter hospitalization in Group I (4.1 days) compared to Group II (15.2 days), with p=0.0123; and together with that a lower cost per patient from U$14,700 in Group I to U$19,872 in Group II (p=0.0103).
DISCUSSION
Duodenal perforations are an uncommon adverse event during ERCP with a reported incidence around 0.14 to 6% (12-16), but can be catastrophic. Being a rare event makes it very difficult to find enough patients for any trial. In these 5 years our perforation rate was only 0.5%. There had been also most recent publications that duodenal perforations are even more rare than 16,17 previously though (16,17). We were not able to reach our sample size; still we were able to collect 23 patients over 5 years. We decided to close our study at this point, as we would require several years to collect this number of patients.
The first two classifications for duodenal perforations after ERCP were published in 1999 and 2000 (18,19). Howard et al. classified them as: guide-wire induced perforation, periampullary after sphincterotomy; and luminal in a site away from the ampulla (18). The one published by Stapfer et al. (19) is based on the potential management of perforation: Type 1 is usually a large defect and away from the ampulla, they usually have large leaks on imaging (either retroperitoneal or peritoneal) and usually require surgery. Type 2 is periampullary and tend to be discrete. Type 3 is associated with the instrumentation of the biliary tree. Type 2 and 3 normally do not require surgery. Finally, type 4 are those that develop in the retroperitoneum, are probably related to barotrauma, no overt perforation is detected and do not require surgery. Overall, authors recommend surgery in the following scenarios: large persistent extravasation of contrast, unresolved fluid collection, unresolved choledocolithiasis or retained hardware, massive pneumoperitoneum with a duodenal diverticulum and when there is failure of nonsurgical management (19).
This is the first trial comparing endoscopic intervention with surgery for duodenal perforations post-ERCP. Studies from large prospective databases or from large tertiary centers in the current era of therapeutic ERCP are few (1,20).
The success at closing the defect was 100% in both groups. Still one death in the endoscopic group (in the analysis this was non-significant between the groups). Then probably we can consider that at least endoscopy is equally effective when compared to surgery in these cases with early diagnosis. Two additional advantages of endoscopy group are the shorter hospitalization and less expense.
Limitations in our study include small sample and heterogeneous group of patients included in each arm (peritoneal and retroperitoneal perforations). The small number of patients is difficult to overcome, becoming this adverse event <1% of all the ERCP. Second, all the duodenal perforations after the ERCP are not equal and certainly randomization of the patients helped to eliminate the bias, but still is a very tough scenario.
The current guidelines about ERCP and their adverse events mention management including: fasting, nasogastric or nasobiliary drainage, and antibiotics (4). The recommendation when to pursue to surgical intervention is difficult to define and require close evaluation by the surgical and gastroenterology teams.
From the literature, we have the initial publications from Howard et al. (18) and Stapfer et al. (19). They both recommend surgery for defects in the duodenal wall away from the papilla (the majority of the peritoneal perforations). However their studies were published more than 10 years ago and their conclusions and recommendations are probably not completely valid anymore.
Some authors stated the difficulty of classifying the perforation in the previous schemes right away after the procedure. For them, the key in the decision of pursuing surgical management was close frequent evaluation of the patient by the surgical team (18,19,21).
Li et al. also reported their experience in 2012 and reviewed of the literature including the numbers of 6 additional papers (6). Two hundred and thirteen (213) patients with duodenal perforations post-ERCP were included; 140 with retroperitoneal perforations and 73 with peritoneal perforations. Of the retroperitoneal perforations 87.9% recovered with conservative management, with a total mortality in this group of 2.9%. In the peritoneal perforations group 80.8% required surgery and the total mortality was 24.7%. The peritoneal perforations carry a worse prognosis. The mortality in 19/22 of the cases was secondary to sepsis. They also suggest that the majority of the retroperitoneal cases can be managed with conservative treatment (6). They support the endoscopic closure of the defects if possible. Thereafter there were several case publications, but no comparison to the surgical intervention (5-11).
Most of the above literature was published after our trial design and was not taken in the elaboration of our protocol. However several points are important to mention. Still the majority of the perforations are diagnosed during ERCP. Late diagnosis carries a dismal prognosis. To avoid late diagnosis some authors suggest an abdominal film before and after ERCP in each patient not to miss silent perforations (6). Yet this means multiple negative studies, as perforations are <1% of all ERCP. Also some false-positive studies as routine CT after ERCP showed extraluminal air in 29% of asymptomatic patients (22).
It is difficult to generalize recommendations for all duodenal perforations after ERCP. Nevertheless for our current endoscopic knowledge and resources, the cases of perforations documented during ERCP should have attempted endoscopic closure of the defect by clips, stent or other available tools and accessories. The Endoscopic and Surgical teams should closely manage all cases even the perforation has been closed by endoscopy. Retroperitoneal perforations are less likely to require surgical intervention. Again this might not be valid in a few years, considering that our field is evolving so fast.
Repeating another study like this might not be ethically, as with the available literature we see that many cases can be managed with conservative treatment and can avoid completely surgery. But we can be sure that endoscopy can save some cases that were referred to surgery a few years ago. We concluded that endoscopic therapy is an alternative to surgical intervention in the cases of large retroperitoneal and peritoneal duodenal perforations post-ERCP.
REFERENCES
-
Cotton PB, Lehman G, Vennes J, Geenen JE, Russell RC, Meyers WC, et al. Endoscopic sphincterotomy complications and their management: an attempt at consensus. Gastrointest Endosc. 1991;37(3):383-93.
-
Ell C, Rabenstein T, Schneider H T, Ruppert T, Nicklas M, Bulling D. Safety and efficacy of pancreatic sphincterotomy in chronic pancreatitis. Gastrointest Endosc. 1998;48(3):244-9.
-
Vandervoort J, Soetikno RM, Tham TC, Wong RC, Ferrari AP Jr, Montes H, et al. Risk factors for complications after performance of ERCP. Gastrointest Endosc. 2002;56 (5):652-6.
-
ASGE Standards of Practice Committee, Anderson MA, Fisher L, Jain R, Evans JA, Appalaneni V, et al. Complications of ERCP. Gastrointest Endosc. 2012;75(3):467-73.
-
Seibert DG. Use of an endoscopic clipping device to repair a duodenal perforation. Endoscopy. 2003;35(2):189.
-
Li G, Chen Y, Zhou X, Lv N. Early management experience of perforation after ERCP. Gastroenterol Res Pract. 2012;2012:657418.
-
Lee TH, Bang BW, Jeong JI, Kim HG, Jeong S, Park SM, et al. Primary endoscopic approximation suture under cap-assisted endoscopy of an ERCP-induced duodenal perforation. World J Gastroenterol. 2010;16(18):2305-10.
-
Nakagawa Y, Nagai T, Soma W, Okawara H, Nakashima H, Tasaki T, et al.Endoscopic closure of a large ERCP-related lateral duodenal perforation by using endoloops and endoclips . Gastrointest Endosc.. 2010;72(1):216-7.
-
Yang J F, Zhang X, Zhang X F. [Diagnosis and management of duodenal perforation after endoscopic retrograde cholangio- pancreatography: clinical analysis of 15 cases]. Zhonghua Wei Chang Wai Ke Za Zhi. 2012;15(7):682-6.
-
Baron TH, Gostout CJ. Herman L. Hemoclip repair of sphincterotomy-induced duodenal perforation. Gastrointest Endosc. 2000;52(4):566-8.
-
Solomon M, Schlachterman A, Morgenstern R. Iatrogenic duodenal perforation treated with endoscopic placement of metallic clips: a case report. Case Rep Med. 2012;2012:609750.
-
Andriulli A, Loperfido S, Napolitano G, Niro G, Valvano MR, Spirito F, et al. Incidence rates of post-ERCP complications: A systematic survey of prospective studies. Am J Gastroenterol. 2007;102(8):1781-8.
-
Masci E, Toti G, Mariani A, Curioni S, Lomazzi A, Dinelli M, et al. Complications of diagnostic and therapeutic ERCP: A prospective multicenter study. Am J Gastroenterol. 2001;96(2):417-23.
-
Avgerinos DV, Llaguna OH, Lo AY, Voli J, Leitman IM. Management of endoscopic retrograde cholangiopancreatography: related duodenal perforations. Surg Endosc. 2009;23(4):833-8.
-
Lai CH, Lau WY. Management of endoscopic retrograde cholangiopancreatography related perforation. Surgeon. 2008;6(1):45-8.
-
Kodali S, Monkemuller K, Kim H, Ramesh J, Trevino J, Varadarajulu S, et al. ERCP-related perforations in the new millennium: A large tertiary referral center 10-year experience. United European Gastroenterol J. 2015 Feb;3(1):25-30.
-
Law R, Baron TH. ERCP. Gastrointest Endosc. Gastrointest Endosc. 2013;78(3):428-33.
-
Howard TJ, Tan T, Lehman GA, Sherman S, Madura JA, Fogel E, et al. Classification and management of perforations complicating endoscopic sphincterotomy. Surgery. 1999;126(4):658-63.
-
Stapfer M, Selby RR, Stain SC, Katkhouda N, Parekh D, Jabbour N, et al. Management of duodenal perforation after endoscopic retrograde cholangiopancreatography and sphincterotomy. Ann Surg. 2000;232(2):191-8.
-
Freeman ML, Nelson DB, Sherman S, Haber GB, Herman ME, Dorsher PJ, et al. Complications of endoscopic biliary sphincterotomy. N Engl J Med. 1996;335(13):909-18.
-
Dubecz A, Ottmann J, Schweigert M, Stadlhuber RJ, Feith M, Wiessner V, et al. Management of ERCP-related small bowel perforations: the pivotal role of physical investigation. Can J Surg. 2012;55(2):99-104.
-
Genzlinger JL, McPhee MS, Fisher JK, Jacob KM, Helzberg JH. Significance of retroperitoneal air after endoscopic retrograde cholangiopancreatography with sphincterotomy. Am J Gastroenterol. 1999;94(5):1267-70.
Correspondence: Everson L. A. Artifon
E-mail: eartifon@hotmail.com
Recibido: 27-07-2015
Aceptado para publicación: 18-10-2015