Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista de Gastroenterología del Perú
versión impresa ISSN 1022-5129
Rev. gastroenterol. Perú vol.37 no.1 Lima ene./mar. 2017
ARTÍCULOS ORIGINALES
Epidemiological aspects of endoscopic resections of colorectal polyps in patients at an endoscopy training center in the Santos region, Brasil
Aspectos epidemiológicos de las resecciones endoscópicas de los pólipos colo-rectales en un centro de entrenamiento de endoscopía en la región de Santos, Brasil
Tiago Franco Vilela Filho1a, Gabriel Marques Fávaro1b, Diego Soares Coca1a, Lubia Bonini Daniel1c, Katia Ferreira Guenaga1c, Ricardo Sato Uemura1c, Carlos Kyoshi Furuya Junior1c, Everson L. A. Artifon1d
1 in the Digestive Endoscopy Sector, Hospital Ana Costa. Santos, São Paulo, Brasil.
a Trainee; b Resident; c Attending Physician; d Head
ABSTRACT
Introduction: Colorectal polyps are structures that project from the surface of the mucosal layer of the large intestine. They are classified as neoplastic or non-neoplastic. Early detection of pre-neoplastic lesions is important for preventing colorectal cancer. These can be resected so as to decrease the morbidity and mortality rates. Colonoscopy is the gold-standard procedure for diagnosing and resecting precursor lesions. Objective: To evaluate the epidemiological, endoscopic and histological aspects of endoscopic resection of lesions of the colon and rectum at a training center. Materials and method: A search was conducted in the database of our institution covering the period from January 2011 to July 2014. Cases that underwent endoscopic resection of polyps and/or colorectal lesions were selection. The following variables were defined: general data on the patients (age, gender and indication from the examination) and data on the polypoid lesion (number, histological type and topographic distribution). Results: 678 lesions were identified in 456 examinations. Regarding sex, 242 (53.1%) were female and 214 (46.9%) were male. The mean age was 64.54 years, with extremes of 5 and 94 years. The most frequent locations were the rectum (21%) and sigmoid (20%). Histologically, 34.7% were hyperplastic polyps and 58.9% were adenomatous polyps, of which 74.1% were tubular, 10.6% tubulovillous, 2% villous and 13% indeterminate; and 1.7% were adenocarcinomas. In 65.4% of the cases, the examination showed that only one polyps was present, while 34.6% had two or more lesions. Conclusion: In our clinic, with a mean of 250 examinations/month, the parameters evaluated were compatible with the results reported in the literature.
Keywords: Polyps; Colonoscopy; Colorectal cancer (source: MeSH NLM).
RESUMEN
Introducción: Los pólipos colorrectales son estructuras que se proyectan en la superficie de la capa mucosa del intestino grueso. Son clasificados en neoplásicos y no neoplásicos. La detección precoz de lesiones preneoplásicas es relevante en la prevención del cáncer colorrectal. Pueden ser resecados y reducir los índices de morbimortalidad. La colonoscopia es el patrón de oro para el diagnóstico y resección de lesiones precursoras. Objetivo: Evaluar aspectos epidemiológicos, endoscópicos e histológicos relacionados a las resecciones endoscópicas de lesiones de colon y recto en un centro de entrenamiento. Matariales y métodos: Fue realizada una búsqueda en la base de datos de nuestra institución durante el período de enero de 2011 a julio de 2014. Se seleccionaron aquellos sometidos a las resecciones endoscópicas de pólipos y/o lesiones colorrectales. Las siguientes variables fueron definidas: datos generales de los pacientes (edad género e indicación del examen) y datos de la lesión polipoidea (número, tipo histológico, distribución topográfica). Resultados: Fueron identificadas 678 lesiones en 456 exámenes. Con relación al sexo, 242 (53,1 %) eran del género femenino y 214 (46,9 %) masculino. El promedio de edad fue de 64,54 años, con extremos de 5 y 94 años. La ubicación más frecuente fue en el recto (21 %) y sigmoide (20 %). Histológicamente, 34,7% eran pólipos hiperplásicos y 58,9% adenomatosos, siendo 74,1% tubulares, 10,6% tubulovellosos, 2% vellosos y 13% indeterminados y, 1,7% correspondieron a adenocarcinomas. En el 65,4% de los casos existía solamente un pólipo al hacer el examen, 34,6% presentaban dos o más lesiones. Conclusión: En nuestro trabajo, con un promedio de 250 exámenes/mes, los parámetros evaluados fueron compatibles a los resultados encontrados en la literatura.
Palabras clave: Pólipos; Colonoscopía; Cáncer colorrectal (fuente: DeCS BIREME).
INTRODUCTION
Polyp is a descriptive term for all tissue structures that originate in the wall of the digestive tract and project into the lumen in a regular and circumscribed manner, thus forming a prominence within the lumen, which may or may not be neoplastic (1-3).
According to their macroscopic presentation, polyps can be called flat (sessile), semipedunculated or pedunculares (1). Their size can range from 1 mm to more than 10 cm and they are classified as giant (more than 40 mm), large (20 to 40 mm), medium (5 to 20 mm) or small (less than 5 mm) (1). In addition, they can present singly or multiply (1).
In 1968, Morson established the importance of the progression from adenoma to cancer and classified polyps as either neoplastic, characterized by adenomas and carcinomas, or non-neoplastic, including hamartomatous, inflammatory, hyperplastic or metaplastic forms (2,3).
The main risk factors for development of polyps, and subsequently colorectal cancer, are age, male sex, smoking and alcohol abuse, while use of nonsteroidal anti-inflammatory drugs (NSAIDs), hormone replacement therapy and calcium seem to reduce the chances of the disease (4,5).
Adenomatous polyps account for around 70% to 80% of all polyps. They are known to be pre-malignant lesions that precede sporadic and hereditary colorectal cancer by 10 to 15 years (1,2,5,6). For this reason, detection of preneoplastic lesions in the large intestine is important with regard to prevention of colorectal cancer (2).
Colonoscopy is the gold standard for diagnosing colorectal cancer (1,2). Use of this diagnostic method as a form of screening affects mortality due to colorectal cancer in two ways: through detection of curable early cancer and through detection and removal of polyps (7). Endoscopic polypectomy, which is a procedure with low morbidity and mortality, diminishes mortality due to colorectal cancer by around 90%. It needs to be remembered that all resected polyps should be sent for histopathological examination (1,8).
In most cases, the clinical condition is asymptomatic. When symptoms are present, they are slight and intermittent. The commonest of these is intermittent rectal bleeding of bright red color. Other, much less frequent symptoms include diarrhea or constipation (1).
Colorectal cancer is the third commonest form of neoplasia in the world and the fifth in Brazil (2,9). According to the Brazilian National Cancer Institute (INCA), it is estimated that there will be 34,280 new cases during 2016, of which 16,660 will be in men and 17,620 in women. These numbers correspond to an estimated risk of 16.84 new cases for every 100,000 men and 17.10 for every 100,000 women (10).
The objective of the present study was to ascertain the profile of patients undergoing endoscopic resections in our clinic, with retrospective analysis on the epidemiological, endoscopic and histological aspects of these cases.
MATERIALS AND METHODS
This was a retrospective study to evaluate the profile of patients with polyps and/or colorectal lesions that were resected within the Digestive Endoscopy Sector of Hospital Ana Costa, in Santos – SP, between January 2011 and July 2014, from analysis on the medical records. For this, all the colonoscopy reports over this period were surveyed, in order to select patients who underwent endoscopic resection with a subsequent anatomopathological report, for comparison.
From these data, the following variables were analyzed: general data on the patients (age and sex) and data on the lesions (number, topographic distribution, histological type and resection margins).
The inclusion criteria for performing endoscopic resection by means of colonoscopy were: presence of polyps and/or colorectal lesions that were resectable by means of endoscopy; and absence of coagulation disorders.
On the other hand, the exclusion criteria were: presence of polyps and/or colorectal lesions that were unresectable; presence of coagulation disorders; cases of inadequate colon preparation; and cases of colonoscopy examination without any visible lesions.
All the patients were constantly monitored by an anesthesiologist.
Our team has Pentax devices available (EPK – 1000; EPK – i).
The topographic categories used were: cecum, ascending colon, transverse colon descending colon, sigmoid colon and rectum. It should be noted that for the purposes of the statistical analysis, the first three categories were grouped as the right colon and the last three, as the left colon.
In relation to the histological type, the lesions were classified as hyperplastic, adenomatous, tubular adenoma, tubulevillous adenoma, villous adenoma, adenocarcinoma and other results. The "others" category included benign polyps such as inflammatory and hamartomatous types. The reports from the anatomopathological service of Hospital Ana Costa produced during the first part of the study period did not allow appropriate detailing of the lesions. However, through meetings with the Digestive Endoscopy Sector aimed towards reaching a consensus, revised description standard was achieved.
Statistical analysis
All the variables were initially analyzed descriptively. For the quantitative variables, this analysis comprised observation of the minimum and maximum values and calculation of the means, standard deviations and medians. For the qualitative variables, absolute and relative frequencies were calculated. To test the homogeneity between the proportions, the chi-square test was used (11).
The significance level used for the tests was 5%.
RESULTS
In this study, 456 colonoscopy examinations conducted within the Digestive Endoscopy Sector of Hospital Ana Costa over the period from January 2011 to July 2014 were evaluated. These examinations were conducted by the seven endoscopists who comprised the clinical staff, and 50% were performed by just two of them.
Among these 456 patients, the age range was from 5 to 94 years (mean of 64.54 years with standard deviation of 13.21 years and median of 66 years). Regarding sex, 214 (46.9%) were male and 242 (53.1%) were female.
Out of the 456 examinations selected, 298 (65.4%) presented a single polypoid lesion, 112 (24.6%) had two, 33 (7.2%) had three, 11 (2.4%) had four, one (0.2%) had five and one (0.2%)had eight.
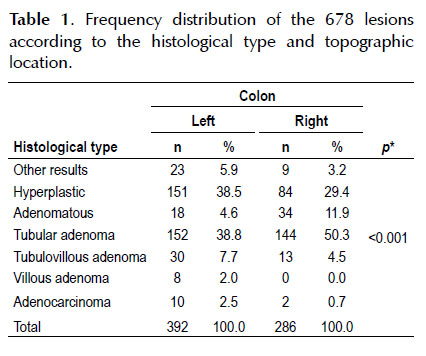
Among the 456 patients, 678 lesions were diagnosed and these had the following topographic locations: 40 (5.9%) in the cecum, 110 (16.2%) in the ascending colon, 136 (20.1%) in the transverse colon, 112 (16.5%) in the descending colon, 137 (20.2%) in the sigmoid colon and 143 (21.1%) in the rectum.
Among the 678 lesions analyzed, 235 (34.7%) were hyperplastic, 52 (7.7%) adenomatous, 296 (43.7%) tubular adenomas, 43 (6.3%) tubulevillous adenomas, 8 (1.2%) villous adenomas, 12 (1.7%) adenocarcinomas and 32 (4.7%) others.
In correlating the histological type of lesion with the topographic location in the colon, it was observed that there was a statistically significant difference between the left and right colons. The right colon presented a greater percentage of adenomatous lesions and tubular adenomas than the left colon. The other types were seen more frequently in the left colon (Table 1).
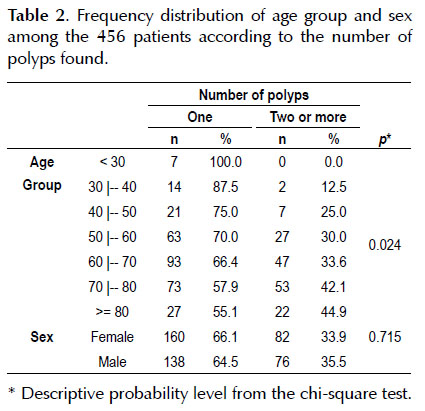
In correlating the number of polyps with the age group, it was noted that there was a statistically significant difference. From the partition of the chi-square text, we observed that among the patients aged over 70 years, a significantly greater percentage of the colonoscopy examinations showed two or more polyps or colorectal lesions than was seen in the group aged under 70 years (p=0.004). On the other hand, in evaluating the variables of sex and number of polyps, it was observed that there were no significant differences (Table2).
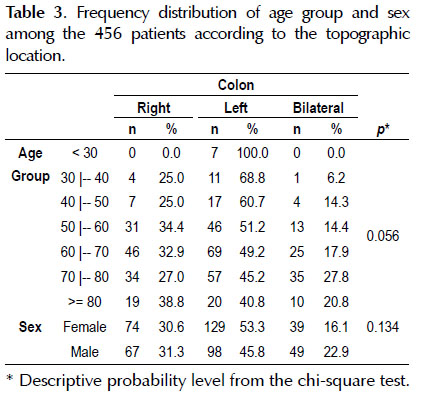
In relation to the topographic location, lesions were diagnosed in the left colon of 227 patients (49.8%), in the right colon of 141 (30.9%) and bilaterally in 88 (19.3%).
In correlating the variables of age group and sex with location, it was noted that there was no statistical difference between the groups (Table 3).
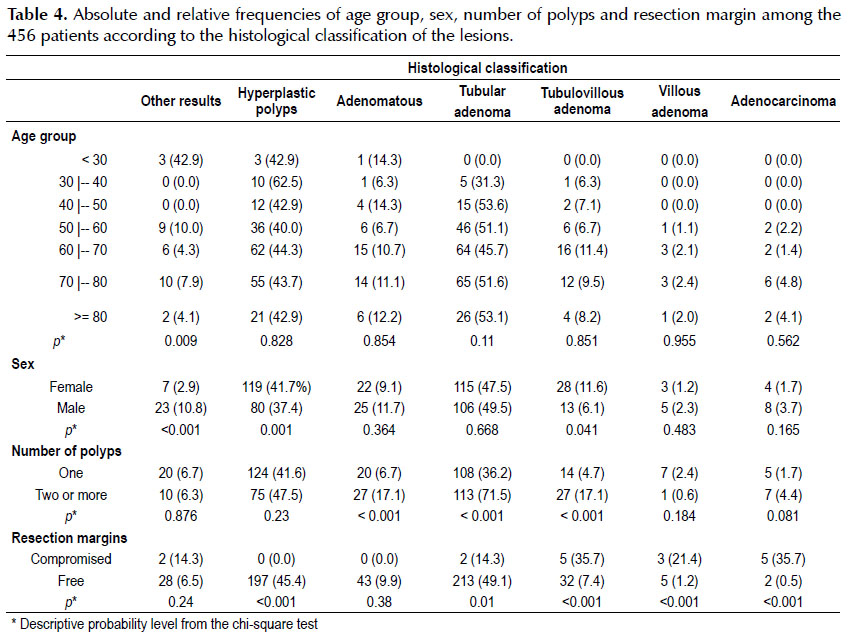
Comparison between the histological type and age group showed that there was a significant difference such that the younger group presented a significantly larger percentage of cases with the histological type of "other results" than shown by the other groups (Table 4).
In correlating the data between the variables of sex and histological type, it was noted that there was a statistically significant difference between the sexes in relation to the histological types of hyperplastic polyps, tubulevillous adenomas and others. Females presented a significantly higher percentage of cases with hyperplastic polyps and tubulevillous adenomas, while males had more "others" (Table 4).
It was shown that there were statistically significant differences in the numbers of polyps in relation to the histological types of adenomatous polyps, tubular adenomas and tubulevillous adenomas. Thus, the patients with a diagnosis of two or more polyps presented significantly higher percentages of adenomatous polyps, tubular adenomas and tubulevillous adenomas, in comparison with the group of patients with only one polyp, seen through colonoscopy.
Regarding the evaluation of the endoscopic resection margins of the polyps or colorectal lesions under the microscope, 434 patients (95.2%) presented diseasefree margins, 14 (3.0%) presented compromised margins and 8 (1.8%) presented compromised and free margins.
In performing the statistical analysis between the lesion resection margin and the histological type of these lesions, it was observed that in the cases of tubulevillous adenomas, villous adenomas and adenocarcinomas, there were significantly greater percentages of cases in which the margins were compromised. On the other hand, the cases of hyperplastic polyps and tubular adenomas presented significantly greater percentages of cases of resection with free margins. It should be noted that, to do the analysis between these two variables, patients who presented two or more colorectal lesions with different types of margins were not taken into consideration (Table 4).
DISCUSSION
Colorectal cancer is recognized as a public health problem worldwide. The rate of sporadic detection of colorectal cancer is 85% among all the cases registered.
The main objective in studying polyps and colorectal lesions is to diminish the incidence of colorectal cancer and achieve early diagnosis of this disease. This aim arises especially from the potential for malignant transformation presented by neoplastic polyps. Among these are adenomas, which as mentioned earlier, are pre-malignant lesions that precede colorectal cancer by 10 to 15 years, and also account for around 80% of the polyps (1,2). Nonetheless, only 5% of adenomas undergo malignant transformation (3). Screening programs involving colonoscopy are important for early detection and removal of these lesions, with consequent halting of the progression from adenoma to cancer and prevention of cancer. Moreover, this enables detection of the cancer at an initial stage and may increase the five-year survival rate by 90% when adequate treatment is implemented (2).
Winawer et al. showed that endoscopic screening programs for patients at higher risk are important for diminishing the mortality due to colorectal cancer. In their study, endoscopic polypectomy of precursor adenomatous lesions reduced the mortality due to colorectal cancer by up to 90% (8). Furthermore, this was found to be a safe method with low complication rates (1,4).
It is known that polyps are highly prevalent in the population, especially with increasing age starting in the fifth decade of life, such that they affect 25% of the population over the age of 75 years (1). In our sample, the mean age of the patients studied was 64.54±13.21 years, with an age range from 5 to 94 years. Among the 456 patients evaluated, 355 (78%) were in the age range from 51 to 80 years. These were the three decades of life most affected, similarly to what has been reported by other authors (2).
In the present study, the incidence according to sex was 46.9% among males and 53.1% among females. The frequency was relatively higher among women, and this differed from the data seen in the literature, which did not show any significant difference between the sexes (1,12,13). Nonetheless, our findings were in line with the data on the incidence of colorectal cancer according to sex from the National Cancer Institute (INCA), in which the number of new cases estimated for Brazil in 2016 is 34,280, of which 16,660 are expected to occur in men and 17,620 in women (10).
Regarding the locations of the polyps and colorectal lesions, these can occur throughout the colon, although currently there is higher prevalence in the proximal colon (1). In a study that analyzed the distribution of colorectal tumors in 1694 cases during the 1960s, 1970s and 1980s, an overall decrease in rectal neoplasms of 15.80% was observed, together with an increase in cases in the right colon of 10.20%, thus showing a change in behavior of colorectal cancer (2,14). In our survey, the highest incidence was in the rectum (21.1%), followed by the sigmoid (20.2%). By adding these two topographic locations, it can be seen that 41.3% were located in the rectum and sigmoid, thus corresponding to the highest incidence of colorectal cancer. In other recent studies, there were higher rates of diagnosis of proximal lesions, thus showing a change in the behavior of colorectal cancer. In the present study, the incidence of lesions in the right colon was 42.2%.
The prevalence of synchronic polyps has been found to be between 18.9 and 37.4% (2,4). Among the 456 patients studied, 158 (34.64%) presented synchronic lesions. Of these, 112 patients presented only one additional polypoid lesion on colonoscopy.
Several studies have shown that the most frequent histological types of polyps in the colonare hyperplastic and adenomatous polyps (1). From the various studies consulted, it was seen that adenomatous lesions could be more (12,15-17) or less frequent (6,13,18) than hyperplastic lesions, or could have similar incidence (6,19). In the present study, adenomas were the most frequent histological type, accounting for 399 (58.9%) of the lesions diagnosed, followed by hyperplastic lesions, accounting for 235 (34.7%).
Hyperplastic polyps are formed through hyperproliferation of the normal cells of the mucosa. They are often indistinguishable macroscopically from adenomatous lesions (1). Moreover, although they are considered to have no potential for malignant transformation, this concept has been questioned through recognition of serrated adenomas (20,21). Several studies have now demonstrated the malignant nature of this type of lesion (9). Hyperplastic polyps are considered to be intermediate lesions characterized by an association of hyperplastic and adenomatous tissue, with evidence that they might be associated with colorectal neoplasia (22). In the present study, the hyperplastic polyps were considered to be pre-malignant lesions because of their association with serrated adenomas, which may evolve to colorectal cancer.
Regarding adenomatous polyps, these can differentiate into three types: tubular, tubulevillous and villous (1). Previous studies have shown that the tubular type is the one most frequently encountered, with incidence ranging from 39 to 80.50%. The tubulevillous type is less common, with incidence ranging from 3 to 55.70%, and the villous type from 4.30 to 17% (2,3). In relation to the 399 adenomatous lesions diagnosed in the present study,296 (74.18%) were tubular adenomas, 43 (10.77%) tubulevillous adenomas and 8 (2%) villous adenomas. It should be noted that in our sample, 52 (13.03%) of the lesions were classified as adenomatous. After meetings with the pathology service of our institution in 2012, there was an improvement in the description of the adenomatous subtype. We therefore saw a similarity between our data and the findings reported in the literature, although the percentage of villous adenomas that we diagnosed was lower than in other reports.
Colonoscopy may fail to prevent colorectal cancer for a variety of reasons, including incomplete polypectomy. Approximately one in every ten tiny polyps found by means of colonoscopy presents incomplete resection through the standard methods for polypectomy (23). Efthymiou et al. showed that the rate of incomplete resection among tiny polyps was 61%, and most of these were hyperplastic (24). In the present study, approximately 95% of the patients presented free resection margins. Most of the cases of endoscopic resection with compromised margins were of three histological types: tubulovillous adenomas, villous adenomas and adenocarcinomas.
Although this was the first study to evaluate the profile of the population undergoing colonoscopy in our region and although it had a large sample, it presents certain limitations. Firstly, this was a retrospective observational study. Moreover, the classification of histological types presented a change, in that after meetings with the pathology service in 2012, it improved. Previously, the polyps were classified as adenomatous, without subdivision into tubular, tubulovillous and villous. It is known that these present differences in relation to the level of malignity. In addition, our sample did not include any cases of serrated adenomas, given that this classification was not described in the anatomopathological reports.
Conclusion
The data obtained in our study were compatible with reports in the literature. This shows the importance of performing colonoscopy and, if necessary, polypectomy for preventing colorectal cancer, a disease that presents high morbidity and mortality when diagnosed late.
Conflict of interests: the authors have declared that no competing interests exist.
Funding: none.
BIBLIOGRAPHIC REFERENCES
1. Quilici FA, Quilici LCM. Polipos e poliposes. In: Averbach M. Endoscopia digestiva – diagnostico e tratamento, SOBED. Rio de Janeiro: Revinter; 2013. p. 425-36. [ Links ]
2. Torres Neto JR, Arcieri JS, Teixeira FR, Aspectos epidemiológicos dos pólipos e lesões plano-elevadas colorretais. Rev Bras Coloproct, 2011;30(4):419-29 [ Links ]
3. Bas B, Dinc B, Oymaci E, Mayir B, Gunduz UR, What are the Endoscopic and Pathological Characteristics of Colorectal Polyps? Asian Pac J Cancer Prev. 2015;16(13):5163-7. [ Links ]
4. Manzione CR, Nadal SR, Nadal MA, Melo SVM. Análise morfológica e histológica de pólipos colorretais submetidos à ressecção endoscópica. Rev Bras Coloproct. 2004;24(2):119-25. [ Links ]
5. Iravani S, Kashfi SM, Azimzadeh P, Lashkari MH. Prevalence and characteristics of colorectal polyps in symptomatic and asymptomatic Iranian patients undergoing colonoscopy from 2009-2013. Asian Pac J Cancer Prev. 2014;15(22):9933-7. [ Links ]
6. Liljegren A, Lindblom A, Rotstein S, Nilsson B, Rubio C, Jaramillo E. Prevalence and incidence of hyperplastic polyps and adenomas in familial colorectal cancer: correlation between the two types of colon polyps. Gut. 2003;52(8):1140-7. [ Links ]
7. Zauber AG, Winawer SJ, Obrien MJ, Landsdorp-Vogelaar I, van Ballegooijen M, Hankey BF, et al. Colonoscopic polypectomy and long-term prevention of colorectal-cancer deaths. N Engl J Med. 2012;366(8):687-96. [ Links ]
8. Winawer SJ, Zauber AG, Ho MN, O’Brien MJ, Gottlieb LS, Sternberg SS, et al. Prevention of colorectal cancer by colonoscopicpolypectomy. The National Polyp Study Workgroup. N Engl J Med. 1993;329(27):1977-81.
9. Szylberg A, Janiczek M, Popiel A, MarszaBek A. Serrated polyps and their alternative pathway to the colorectal cancer: a systematic review. Gastroenterol Res Pract. 2015;2015:573814. [ Links ]
10. InstitutoNacional de Câncer [Internet]. Brasil: Ministério da Saúde c1996-2007 [citado el 30 de agosto de 2008]. Disponible en: http://www.inca.gov.br/ [ Links ]
11. Rosner B. Fundamentals of Biostatistics. 2nd edition. Boston: PWS Publishers; 1986. [ Links ]
12. Webb WA, McDaniel L, Jones L. Experience with 1000 colonoscopic polypectomies. Ann Surg. 1985;201(5):626-32. [ Links ]
13. Fenoglio-Preiser CM, Hutter RVP. Colorectal polyps: pathologic diagnosis and clinical significance. CA Cancer J Clin. 1985;35(6):322-44. [ Links ]
14. Gharemani GG, Dowlatshahi K. Colorectal carcinomas: diagnostic implications of their changing frequency and anatomic distribution. World J Surg.1989;13(3):321-5. [ Links ]
15. Zheng S, Liu XY, Ding KF, Wang LB, Qiu PL, Ding XF, et al. Reduction of the incidence and mortality of rectal cancer by polypectomy: a prospective cohort study in Haining County. World J Gastroenterol. 2002;8(3):488-92. [ Links ]
16. Morimoto LM, Newcomb PA, Ulrich CM, Bostick RM, Lais CJ, Potter JD. Risk factors for hyperplastic and adenomatous polyps: evidence for malignant potential? Cancer Epidemiol Biomarkers Prev. 2002;11(10 Pt 1):1012-8. [ Links ]
17. Patel K, Hoffman NE. The anatomical distribution of colorectal polyps at colonoscopy. J Clin Gastroenterol. 2001;33(3):222-5. [ Links ]
18. Williams AR, Balasooriya BA, Day DW. Polyps and cancerof the large bowel: a: necropsy study in Liverpool. Gut. 1982;23(10):835-42. [ Links ]
19. Imperiale TF, Wagner DR, Lin CY, Larkin GN, Rogge JD, Ransohoff DF. Results of screening colonoscopy among persons 40 to 49 years of age. N Engl J Med. 2002;346(23):1781-5. [ Links ]
20. Huang CS, O’Brien M J, Yang S, Farraye FA. Hyperplasticpolyps, serrated adenomas, and the serrated polyp neoplasia pathway. Am J Gastroenterol. 2004;99(11):2242-55.
21. Higuchi T, Jass JR. My approach to serrated polyps of the colorectum. J Clin Pathol. 2004;57(7):682-6. [ Links ]
22. Cross SS. Kappa statistics as indicators of quality assurancein histopathology and cytopathology. J Clin Pathol. 1996;49(7):597-9. [ Links ]
23. Gomez V, Badillo RJ, Crook JE, Krishna M, Diehl NN, Wallace MB. Diminutive colorectal polyp resection comparing hot and cold snare and cold biopsy forceps polypectomy. Results of a pilot randomized, single-center study (with videos). Endosc Int Open. 2015;3(1):E76-80. [ Links ]
24. Efthymiou M, Taylor AC, Desmond PV, Allen PB, Chen RY. Biopsy forceps is inadequate for the resection of diminutive polyps. Endoscopy. 2011;43(4):312-6. [ Links ]
Correspondence:
Tiago Franco Vilela Filho Rua Pedro Américo, 60 - 11075-400 Santos, SP. Brazil.
E-mail: tiagofvf@yahoo.com.br
Recibido: 2-4-2016
Aprobado: 16-7-2016