Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista de Gastroenterología del Perú
Print version ISSN 1022-5129
Rev. gastroenterol. Perú vol.37 no.4 Lima Oct./Dec. 2017
ARTÍCULOS ORIGINALES
Diagnostic and therapeutic cholangioscopy in biliary diseases: a prospective study in Peru
Uso diagnóstico y terapéutico de la colangioscopía en enfermedades de la vía biliar: un estudio prospectivo en Perú
Víctor Sánchez Cerna1a, Christian Alcántara Figueroa1b, Tania Reyes Mugruza1a, Lisbeth Acorda Sifuentes1a, Miguel Valverde Huamán1a, Mario Valdivia Roldán1a, Gloria Várgas Cárdenas1a, Corina Mayuri Bravo de Rueda1a, Rolando Tito La Torre1a, Jeimy Ramos Pacheco1a, Miguel Chávez Rossell1a, Lucinda Morán Tisoc1a
1 Servicio de Gastroenterología, Hospital Nacional Arzobispo Loayza. Lima, Perú.
a Médico Asistente; b Médico Residente
ABSTRACT
Introduction: Cholangioscopy is a test that allows the evaluation of the biliary epithelium. It is used for diagnosis and management of biliary diseases. Objectives: Determine the success rate of complete removal of difficult stones with the use of laser lithotripsy through cholangioscopy as well as its complications. Determine the visual impression accuracy of bile duct injuries. Materials and methods: This is a prospective and descriptive study. We included 39 patients between July 2016 and July 2017 with diagnosis of difficult stones in the biliary tract and indeterminate stenosis of the biliary tract that were submitted to cholangioscopy. Results: Success rate of complete removal of difficult stones was 65.3%, there was one complication. Two laser sessions were required in 4 of the 17 patients who obtained complete removal of the stones. The visual impression accuracy of lesions in the bile duct to determine malignancy coincided in all cases with the final diagnosis of the patient. Conclusions: Laser lithotripsy allows a safe and effective treatment of the difficult stones of the bile duct. Precession of visual impression of lesions in the bile duct is very high.
Keywords: Choledocholithiasis; Cholangiopancreatography, endoscopic retrograde; Lasers (source: MeSH NLM).
RESUMEN
Introducción: La colangioscopía es un examen que permite evaluar la luz biliar, el epitelio biliar y sirve para diagnóstico y manejo de enfermedades de la vía biliar. Objetivos: Determinar la tasa de éxito de remoción completa de cálculos difíciles con el uso de litotripcia con láser a través de la colangioscopía asi como las complicaciones de ésta. Determinar la precisión de impresión visual de lesiones de la vía bilar. Materiales y métodos: Estudio prospectivo, descriptivo. Se incluyeron a 39 pacientes entre Julio 2016 a Julio 2017 con diagnóstico de cálculo difícil en la vía biliar y estenosis indeterminada de la vía biliar que fueron sometidos a colangioscopía. Resultados: La tasa de éxito de remoción completa de cálculos difíciles fue de 65,3% con una complicación. Se requirió de dos sesiones con láser en 4 de los 17 pacientes que obtuvieron remoción completa de cálculos. La precisión de impresión visual de lesiones en la vía biliar para determinar malignidad coincidió en todos los casos con el diagnóstico final del paciente. Conclusiones: La colangioscopía con uso de litotripcia con láser permite un tratamiento seguro y eficaz en los cálculos difíciles de la vía biliar. La precesión de la impresión visual de lesiones en la vía biliar es muy alta.
Palabras clave: Coledocolitiasis; Pancreatocolangiografía retrógrada endoscópica; Láser (fuente: DeCS BIREME).
INTRODUCTION
Endoscopic retrograde cholangiopancreatography (ERCP) is a mixed, endoscopic-radiological technique, described in 1968 by McCune et al., who were able to cannulate the Vater ampulla for the first time and thus obtain x-rays of the pancreatic ducts (1). Cholangioscopy, on the other hand, allows the evaluation of biliary light and bile epithelium. It also allows doctors to take some samples of biliary tissue and to make some therapeutic procedures. Its main indications are the management of difficult stones of the biliary and pancreatic ducts and to determine the origin of indeterminate stenosis of the bile duct with good precision and low complication rate (2).
The American Society of Gastroenterology reports that gallstones affect more than 20 million people in the US (3). A portion of these patients also have choledocholithiasis, including 5 to 10% of those who undergo laparoscopic cholecystectomy for symptomatic cholelithiasis (4-8) and 18 to 33% of patients with acute biliary pancreatitis (9-12).
Extraction of stones using balloon at the intraductal level continues to be the technique of choice to permeabilize the bile duct, including difficult stones. Even so, electrohydraulic laser lithotripsy assisted by cholangioscopy is a new technique that emerges as an advanced intervention for cases of difficult stones of the bile duct that are not solved with the balloon (13).
In view of the above, we decided to carry out the present research with the objective of answering the question about the value of cholangioscopy use in intra ductal biliary disease in a Hospital of the Ministry of Health in Lima, Peru. This will allow us to know the success rate of removal of difficult stones of the biliary tract as well as the usefulness of this procedure in the diagnosis of indeterminate stenosis. By demonstrating the utility and low complications of this technique, patients could avoid surgery and morbidity and mortality derived from surgery.
MATERIALS AND METHODS
This prospective, observational, transverse, and descriptive study was performed at "The Arzobispo Loayza National Hospital" in Lima-Peru, between July 2016 and July 2017. This study was based on the review of clinical records and follow-up of outpatients or hospitalized patients. We obtained data from those with a diagnosis of difficult stones and indeterminate stenosis of the biliary tract who had laboratory exams and radiologic images before and after the procedure. People younger than 15 years and / or pregnant women were excluded from the study. For this purpose, a data collection form was developed. In the data processing, the programs Microsoft Excel V. 2010 and SPSS V.15 were used to perform the descriptive statistical analysis corresponding to frequencies, averages, means, etc. The research work was evaluated and approved by the Chief of the Gastroenterology Service and the Office of Support of Research of the Arzobispo Loayza National Hospital.
In this study, the following operational definitions will be considered:
Intraductal biliary disease: Defined as an obstruction of the biliary tract either by benign or malignant stenosis of the biliary tract, gallstones in the biliary tract or cysts of the biliary tract.
Complete stone removal: Defined as the total extraction of difficult stone(s) from the biliary tract in one or more ERCP sessions.
Difficult stone in the bile duct: Defined by 1) congenital or post-surgical anatomical alteration of the bile duct and / or periampular region; 2) large stones (diameter >15 mm); 3) multiple stones (greater than or equal to 3); 4) intrahepatic location of the stones; 5) stone location above a stenosis or those that are impacted (6).
Indeterminate stenosis of the bile duct: It is a stenosis in which its nature can not be determined after obtaining basic laboratory data, abdominal images (magnetic resonance, tomography and / or endoscopic ultrasonography) and retrograde endoscopic cholangiopancreatography.
Endoscopic and technical system
All procedures were performed on outpatient and hospitalized patients by a trained endoscopists and with sedation monitoring. An endoscopic papillo-sphincterotomy was performed prior to insertion of the cholangioscope. Methods for making this dissection included sphincteroplasty, sphincterotomy, or both. Cholangioscopy procedures were performed with the Spyglass®DS system, belonging to Boston Scientific, with a distal diameter of 3.5 mm, a therapeutic channel of 1.2 mm and a working length of 2140 mm. All patients received one dose of ceftriaxone 2 g iv during the procedure and then ciprofloxacin 500 mg v.o bid for 3 days (antibiotic prophylaxis). The cholangioscope was introduced through a standard therapeutic duodenoscope (Fujinon), model 4400 HD, field of view of 100° and therapeutic channel 4.2 mm.
The laser lithotripsy system was performed using the Holmiun Laser device, Auriga QI model, using laser fibers of 365 um, 4 m in length and parameters of a frequency of 10 Hz, power 1,200 mJ and 12 watts of power. After this procedure the fragments of the calculus were removed from the bile duct using balloon catheter and / or Dormia´s basket.
Regarding patients with indeterminate bile duct stenosis who underwent biopsy, these were obtained through spybite® and then were evaluated by a pathologist selected from the Anatomy-Pathology Service of the Arzobispo Loayza National Hospital. The clinical history was obtained to get the information of the final diagnosis of all patients. Patients with visual impression and / or biopsy compatible with cholangiocarcinoma were referred to the Oncology and Surgery service of the Arzobispo Loayza National Hospital. A monthly follow-up was performed up to 6 months after cholangioscopy requesting hemogram, liver biochemical tests and tumor markers in those patients with visual impression and / or biopsy compatible with benign lesions of the bile duct.
RESULTS
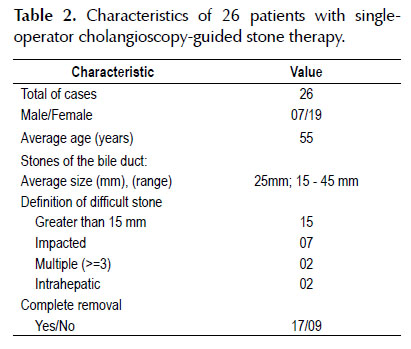
In total, 39 patients underwent cholangioscopy. Of the 39 patients, 26 had a therapeutic indication for difficult stones management and 13 patients underwent cholangioscopy for etiological diagnosis of indeterminate biliary stenosis. The mean age was 55 years (range 2587 years) and all had preparation of the papilla with sphincterotomy. The characteristics of all patients are shown in Table 1.
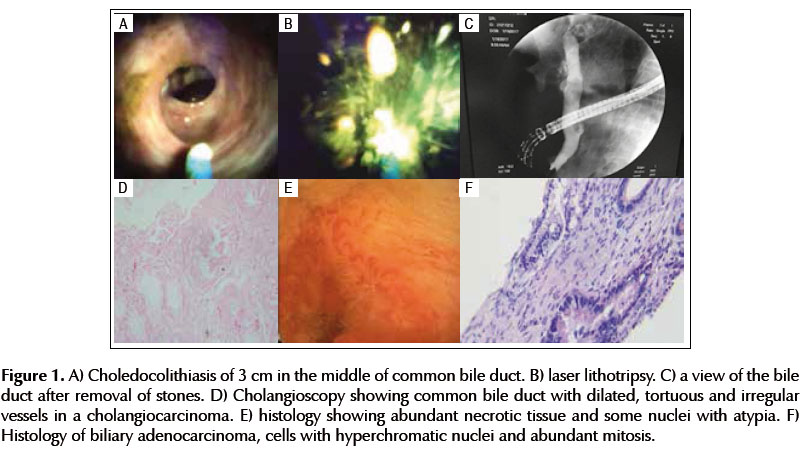
The use of laser lithotripsy using cholangioscopy was used in 26 patients for difficult stones management of the biliary tract, of which 19 patients were women and 7 men with an average age of 55 years. Success (complete removal) was 65% (Table 2). The stones were greater than 15 mm in 15 patients; 7 patients had an impacted stone; 2 patients had multiple stones and 2 patients had intrahepatic stones. (Figure 1).
Two of the 17 patients who had complete removal of stones required two sessions of laser lithotripsy. The mean time of use of laser lithotripsy was 65 min. The size of the stones varied between 15 mm - 45 mm. The only complication was acute cholangitis in one case. Plastic stent was placed in the bile duct in those patients who did not obtain complete removal of the stones.
Factors that were found in those patients that did not obtain complete removal were the following: multiple choledocolithiasis of 35 mm, intrahepatic location, prolonged time procedure greater than 90 min, inability to access with guide above a stone due to marked angulation.
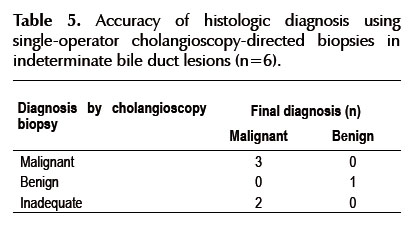
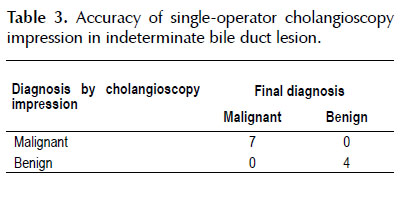
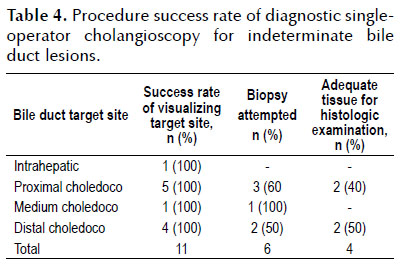
Cholangioscopy was used for the diagnosis of indeterminate bile duct strictures in 13 patients (Tables 3 and 4). The location of the lesion was seen in distal, middle, proximal, intrahepatic bile duct at 4, 1, 5 and 1 occasion respectively. Cholangioscopy was normal in two of the 13 patients. Of the 11 patients with biliary tract injury determined with cholangioscopy, the visual impression of malignant disease was in 7 cases and the impression of benign lesion was in 4 cases (Figure 1). Biopsies were taken in 6 cases of the 7 cases with suspected malignancy (one case could not be obtained because of technical difficulty). The results are shown in Table 5.
DISCUSSION
In this article we discuss two of the most frequent use of cholangioscopy such as its therapeutic use with laser and its usefulness in the diagnosis of indeterminate strictures of the bile duct. Difficult stones of the bile duct are those who have difficult endoscopic removal and occur in patients with anatomical alteration of the bile duct, those stones greater than 15 mm, those stones that are multiple (greater than or equal to 3 calculations), those stones of intrahepatic location, those stones with location above a stenosis or those stones that are impacted (13-16). Stones larger than 20 mm in size need to be fragmented before being removed. However, the success rate to remove them decreases in the presence of the factors already mentioned. With the use of laser cholangioscopy, the success rate for removal of the stones in question has increased, so the American Association of Gastrointestinal Endoscopy (ASGE) mentions in an article published in 2016 a success rate of 70-100% for some authors. It should be noted that factors that decrease success include surgically altered anatomy, stenosis, marked ductal angulation and impacted stones (17). Some authors like Stevens reported the use of cholangioscopy with electrohydraulic lithotripsy. This author reported its use in 15 patients for the management of difficult choledocholithiasis. Removal of the stones was obtained in 85% of the cases (11/13). 61% (8/13) of the cases were removed with an endoscopic therapy session, 23% (3/13) of the cases were removed with 2 sessions of endoscopic therapy (18). Draganov mentions in an international multicenter study with a registry of 296 patients who required peroral cholangioscopy for the treatment of choledocholithiasis and support in the etiologic diagnosis of indeterminate biliary stenosis. The results of this study reported the utility and safety of this procedure (19). Complications of this procedure are the same as ERCP are pancreatitis, hemorrhage, perforation, cholangitis and those related to sedation. A higher risk of cholangitis when using cholangioscopy is described in the international literature, this could be due to the use of intermittent irrigation of saline solution to obtain adequate visualization and the use of intraductal lithotripsy in the cases that were necessary (20). For us the use of intermittent irrigation with saline solution could lead to some fragments of the stone to reach the proximal bile duct or mobilizing them to the intrahepatic ducts, this can produce stasis of the bile and became a risk of cholangitis.
Currently, there are few publications of the use of cholangioscopy in Latin America and the number of patients in each publication does not exceed 100, being also the majority studies in a single center. Landaeta makes a publication about the use of peroral choroangioscopy mono-operator in a Public Hospital in Venezuela in which it presents to 9 patients with pathologies of the bile duct, concluding that the procedure was effective in the evaluation and treatment of stone and biliary lesions (21). In Brazil, Moura et al. conducted the first report of this country about the use of peroral cholangioscopy. As results they obtained that the most frequent indication was choledocholithiasis (12/20 patients), they used electrohydraulic lithotripsy in 8 cases (66%). Electrohydraulic lithotripsy was successful in 7 patients (87.5%) (22). Ospina points out in a study from Colombia the importance of cholangioscopy and shows 9 patients with bilio-pancreatic pathology, 3 of whom were treated with giant choledocholithiasis, achieving success in all patients and he had no complications (23). Another Colombian case-report study shows the usefulness of peroral laser cholangioscopy for the management of large choledocholithiasis in 2 patients, being successful in both cases (14). A study of a third-level private center in Caracas - Venezuela evaluated the use of peroral monooperative cholangioscopy, which involved 46 patients with pathology of the biliary tract, with the following indications: indeterminate stricture of the bile duct (23 cases), choledocholithiasis (20 cases), and tumor (2 cases). The ductal clearance following holmiun lithotripsy lasers of the patients with lithiasis was achieved in 85% after one session, and 15% in a second attempt (24).
To date, this study has the highest number of patients with regard to the use of laser cholangioscopy for difficult stones management in Latin America (all cases treated with the Holmiun Laser equipment). Complete removal was achieved in 65.3% of the 26 patients who were treated with laser for bile duct stone removal. Two laser sessions were required in 4 of the 17 patients who obtained complete removal. The size range of all patients' stones ranged from 15 mm to 45 mm. The size of the largest one was 45 mm and it was completely removed.
This success rate (more than 60%) is comparable to that reported in other studies (14,16,18). The predisposition of this pathology was greater in the female sex, in more than 70% of the cases, and with peaks between the 4th and 6th decade of life. Factors contributing to decreased success in our study were as follows: impacted stones, marked ductal angulation, prolonged operative time greater than 90 min, intrahepatic stones with size larger than 35 mm.
The presence of intrahepatic lithiasis, as well as stones greater than 35 mm, could not be removed by this method despite two prolonged sessions of laser lithotripsy; in the first case we have a difficult access despite the use of the previous guide, it could not be progressed to the respective intrahepatic region, despite multiple attempts and previous lubrication, this could be found in association with two hypotheses such as the thickness of the laser fiber in relation to the therapeutic channel of the cholangioscope, since this fiber is not of specific use for biliary route, making difficult even its external maneuverability its short length, and the second hypothesis would be associated with the diameter of the cholangioscope (3.5 mm) in relation to the therapeutic channel of the duodenoscope (4.2 mm), which would make difficult its progression in proximal areas. Only one complication was present, which was acute cholangitis in a patient who required two sessions but did not have complete removal of the stones. The patient was treated with antibiotics and presented favorable evolution.
Regarding the use of cholangioscopy for the diagnosis of indeterminate biliary stenosis, our study had 13 patients, of whom 2 resulted in normal cholangioscopy. Of the 11 patients in whom bile duct injury was found, 4 had visual impression of benign aspect determined by granular appearance, regular mucosa and preserved vasculature and 7 had visual impression of malignancy determined by a mucosa of irregular surface, tortuous, dilated and irregular neovascularization. Biopsies were taken in 6 of the 7 patients with visual impression of malignancy, in one case due to technical defects, the sample was not taken. Finally, all 7 cases with visual impression of malignancy had the diagnosis of cholangiocarcinoma either by biopsy or after surgical intervention.
Of the results of biopsy, 4 samples were adequate, 3 of them with diagnosis of adenocarcinoma and one of them showed conserved architecture and no neoplastic cells in the submitted sample but the final diagnosis of the patient was cholangiocarcinoma due to surgery. The 4 cases that had impressed benign lesions were monitored monthly for 6 months, carrying a stationary evolution clinically and with imaging tests. It is remarkable the importance of cholangioscopy in this sense as it allows reducing the number of surgeries unnecessary and also are very cruel with important morbi-mortality.
Victor et al. published an interesting application of cholangioscopy in indeterminate biliary strictures. He describes and argues that such is the importance of this procedure that can change the behavior radically in these patients (25). Several studies have been performed to demonstrate the benefit and safety of cholangioscopy in these cases. Thus, Ramchandani et al. (26) described a sensitivity of 95% and a specificity of 75% visual impression using cholangioscopy in 36 patients with indeterminate stenosis. After using cholangioscopic biopsies with Spybite, they demonstrated an accuracy of 82% to differentiate between malignant and benign ductal lesions. Dranagov (27) reported that biopsies taken using single operator cholangioscopy had significantly greater accuracy (84%) compared to standard transpapillary biopsies. The results of the cytology were also compared in this study, with accuracy being 53% with cholangioscopy versus 35% with standard brushing.
Laleman published a prospective study with 45 patients who underwent single-operator cholangioscopy with indication of indeterminate stenosis, the region of interest could be visualized in 93% of cases and biopsy of the lesion with Spybite® was possible in 24 of 29 patients (82.8%). Biopsy specimens were considered adequate by the pathologist in all but one case (28).
Worldwide, cholangioscopy articles continue to be published about its use in getting to know the etiology of indeterminate stenosis, obtaining results similar to the previously described studies (29-33).
To date there are no national publications on the management of difficult stones of the biliary tract with the use of laser and peroral cholangioscopy monooperator. This therapeutic intervention has proven to be effective and safe allowing an alternative to surgery in this pathology. As mentioned in the literature, by facilitating the diagnosis of indeterminate stenosis we can avoid unnecessary risks when addressing non-surgical management regarding the biliary pathology suffered by the patient in cases of benign lesions.
In conclusion, our study demonstrates that the use of laser cholangioscopy allows us to treat safely and with a success greater than 60% to complete removal of difficult stones of the bile duct; which is comparable with the international literature. The precision of the visual impression of cholangioscopy in the etiological diagnosis of the indeterminate stenosis of the biliary tract was very high in our study. However, it should be noted that only 13 cases were studied. It will be possible to have diagnostic test studies that evaluate the performance of biopsies with more patients and obtaining data from other centers of Peru.
Conflict of interests: The authors have declared that no competing interests exist.
Financing: The article did not have any type of financing for its realization.
BIBLIOGRAPHIC REFERENCES
1. McCune W, Short P, Moscovitz H. Endoscopic canulation of the ampulla of Vater: a preliminary report. Ann Surg. 1968;167(5):752-6. [ Links ]
2. Sioulas AD, El-Masry MA, Groth S, Schachschal G, Anders M, Rosch T, et al. Prospective evaluation of the short access cholangioscopy for stone clearance and evaluation of indeterminate strictures. Hepatobiliary Pancreat Dis Int. 2017;16(1):96-103. [ Links ]
3. ASGE Standards of Practice Committee, Maple JT, Ben-Menachem T, Anderson MA, Appalaneni V, Banerjee S, Cash BD, et al. The role of endoscopy in the evaluation of suspected choledocholithiasis. Gastrointest Endosc. 2010; 71(1):1-9. [ Links ]
4. Everhart JE, Ruhl CE. Burden of digestive diseases in the United States I: Overall and upper gastrointestinal diseases. Gastroenterology. 2009;136(2):376-86. [ Links ]
5. Hunter JG. Laparoscopic transcystic bile duct exploration. Am J Surg. 1992;163(1):53-6. [ Links ]
6. Robinson BL, Donohue JH, Gunes S, Thompson GB, Grant CS, Sarr MG, et al. Selective operative cholangiography: appropriate management for laparoscopic cholecystectomy. Arch Surg. 1995;130(6):625-30. [ Links ]
7. Petelin JB. Laparoscopic common bile duct exploration. Surg Endosc. 2003;17(11):1705-15. [ Links ]
8. O’Neill CJ, Gillies DM, Gani JS. Choledocholithiasis: overdiagnosed endoscopically and undertreated laparoscopically. ANZ J Surg. 2008;78(6):487-91.
9. Chang L, Lo SK, Stabile BE, Lewis RJ, de Virgilio C. Gallstone pancreatitis: a prospective study on the incidence of cholangitis and clinical predictors of retained common bile duct stones. Am J Gastroenterol. 1998;93(4):527-31. [ Links ]
10. Chak A, Hawes RH, Cooper GS, Hoffman B, Catalano MF, Wong RC, et al. Prospective assessment of the utility of EUS in the evaluation of gallstone pancreatitis. Gastrointest Endosc. 1999;49(5):599-604. [ Links ]
11. Liu CL, Lo CM, Chan JKF, Poon RT, Lam CM, Fan ST, et al. Detection of choledocholithiasis by EUS in acute pancreatitis: a prospective evaluation in 100 consecutive patients. Gastrointest Endosc. 2001;54(3):325-30. [ Links ]
12. Cohen ME, Slezak L, Wells CK, Andersen DK, Topazian M. Prediction of bile duct stones and complications in gallstone pancreatitis using early laboratory trends. Am J Gastroenterol 2001;96(12):3305-11. [ Links ]
13. Easler J, Sherman S. Endoscopic retrograde cholangiopancreatography for the management of common bile duct stones and gallstone pancreatitis. Gastrointest Endosc Clin N Am. 2015;25(4):657-75. [ Links ]
14. Gómez M, Gutiérrez O, Jaramillo M. Manejo del cálculo difícil en la vía biliar: Serie de casos. Rev Col Gastroenterol. 2015;30(4):461-8. [ Links ]
15. Yasuda I, Itoi T. Recent advances in endoscopic management of difficult bile duct stones. Dig Endosc. 2013;25(4):376-85. [ Links ]
16. McHenry L, Lehman G. Difficult bile duct stones. Curr Treat Options Gastroenterol. 2006;9(2):123-32. [ Links ]
17. ASGE Technology Committee, Komanduri S, Thosani N, Abu Dayyeh BK, Aslanian HR, Enestvedt BK, et al. Cholangiopancreatoscopy. Gastrointest Endosc. 2016;84(2):209-21. [ Links ]
18. Stevens P, Chen Y, Pleskow D, Haluszka O, Peterson B. Biliary stone extraction (BSE) guided by direct visualization using the new SpyGlassTM direct visualization system. Gastrointest Endosc. 2007;65(5):AB96. [ Links ]
19. Draganov P. The SpyGlass® direct visualization system for cholangioscopy. Gastroenterol Hepatol (N Y). 2008;4(7):469-70.
20. Sethi A, Chen YK, Austin GL, Brown WR, Brauer BC, Fukami NN, et al. ERCP with cholangiopancreatoscopy may be associated with higher rates of complications than ERCP alone: a single-center experience. Gastrointest Endosc. 2011;73(2):251-6. [ Links ]
21. Landaeta J, Rodríguez M, Dias C, Corredor L, Esquerre I, Manuitt J, et al. Colangioscopia peroral mono operador (Spyglass). Experiencia preliminar en el Hospital Vargas de Caracas, Caracas, Venezuela. Gen. 2013;67(1):20-4. [ Links ]
22. Moura E, Franzini T, Moura R, Carneiro F, Artifon E. Cholangioscopy in bile duct disease: a case series. Arq Gastroenterol. 2014;51(3):250-4. [ Links ]
23. Ospina J, Raijman I, Velasco B. Spyglass, ¿Es real y útil en nuestro medio? Rev Col Gastroenterol. 2014;29(2):139-45. [ Links ]
24. Landaeta J, Dias C, Paternina R, Tempestini O, Caraballo D. Experiencia colangioscopia peroral monoperador (SPYGLASS) en patología biliar en un centro privado de tercer nivel en Venezuela. Gen. 2016;70(2):61-3. [ Links ]
25. Victor D, Sherman S, Karakan T, Khashab M. Current endoscopic approach to indeterminate biliary strictures. World J Gastroenterol. 2012;18(43):6197-205. [ Links ]
26. Ramchandani M, Reddy D, Gupta R, Lakhtakia S, Tandan M. Role of single-operator peroral cholangioscopy in the diagnosis of indeterminate biliary lesions: a single-center, prospective study. Gastrointest Endosc. 2011;74(3):511-9. [ Links ]
27. Draganov P, Chauhan S, Wagh M, Gupte A, Lin T. Diagnostic accuracy of conventional and cholangioscopy-guided sampling of indeterminate biliary lesions at the time of ERCP: a prospective, long-term follow up study. Gastrointest Endosc. 2012;75(2):347-53. [ Links ]
28. Laleman W, Verraes K, Van Steenbergen W, Cassiman D3, Nevens F3, Van der Merwe S, et al. Usefulness of the singleoperator cholangioscopy system SpyGlass in biliary disease: a single-center prospective cohort study and aggregated review. Surg Endosc. Surg Endosc. 2017;31(5):2223-32. [ Links ]
29. Siddiqui A, Mehendiratta V, Jackson W, Loren D, Kowalski T. Identification of cholangiocarcinoma by using the Spyglass Spyscope system for peroral cholangioscopy and biopsy collection. Clin Gastroenterol Hepatol. 2012;10(5):466-71. [ Links ]
30. Theodoropoulou A, Vardas E, Voudoukis E, Tavernaraki A, Tribonias G, Konstantinidis K, et al. SpyGlass direct visualization system facilitated management of iatrogenic biliary stricture: a novel approach in difficult cannulation. Endoscopy. 2012;44 Suppl 2 UCTN:E433-4. [ Links ]
31. Woo Y, Lee J, Noh D, Park J, Lee K. SpyGlass cholangioscopyassisted guidewire placement for post-LDLT biliary strictures: a case series. Surg Endosc. 2016;30(9):3897-903. [ Links ]
32. Kurihara T, Yasuda I, Isayama H. Diagnostic and therapeutic single-operator cholangiopancreatoscopy in biliopancreatic diseases: Prospective multicenter study in Japan. World J Gastroenterol. 2016;22(5):1891-901. [ Links ]
33. Syam A, Wafa S, Makmun D. The role of per oral cholangiopancreatoscopy (POCPS) in complicated pancreaticobiliary disease. Acta Med Indones. 2015;47(2):169-71. [ Links ]
Correspondence:
Victor Sanchez Cerna
E-mail: visace@hotmail.com
Recibido: 29/12/2017
Aprobado: 12/07/2017