Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista de Gastroenterología del Perú
Print version ISSN 1022-5129
Rev. gastroenterol. Perú vol.38 no.1 Lima Jan./Mar. 2018
ARTÍCULOS ORIGINALES
Upper gastrointestinal endoscopy applied in pediatrics: endoscopic and histological findings, including Helicobacter pylori
Endoscopia digestiva alta aplicada em pediatria: hallazgos endoscópicos e histológicos incluyendo al Helicobacter pylory
Diego Soares Coca1a, Carolina Manna Santos1b, Osmar Silvio Garcia de Oliveira1c, Dayse Aparício Pereira1c, Carlos Kiyoshi Furuya Júnior1c, Everson L.A. Artifon1e,2d
1 Endoscopy Service, Hospital Ana Costa. São Paulo, Brazil.
2 Faculty of Medicine, University of São Paulo. São Paulo, Brazil.
a Trainee, b Resident , c Assistant Physician , d Professor, e Head of the Endoscopy Service
ABSTRACT
Objective: To present and discuss the endoscopic and histological results, as well as the incidence of Helicobacter pylori and other diseases, indications and characteristics of upper digestive endoscopies performed in children. Material and methods: Twenty-five endoscopies were performed in children aged six months to 11 years (mean 7.69 years), from February 2013 to January 2016. In 200 patients, endoscopies were diagnostic and serial biopsies were performed (esophagus, stomach and duodenum), in 120 of them. Results: The indication of endoscopy was diagnosed in 88.89% of the patients, and in 26 patients, a therapeutic procedure was performed. The most frequent endoscopic findings were esophagitis in 49 patients, gastritis in 84 and duodenitis in 16 patients. Four duodenal ulcers were diagnosed. In the therapeutic endoscopies, six gastrostomies were performed, 14 foreign body withdrawals, five nasoenteral tube passages and esophageal dilatation. The H. pylori survey was performed by anatomopathological method and was positive in 26 (13%) of the 200 patients in whom it was searched. Conclusion: pediatric endoscopy is an important niche of the digestive endoscopy, where it is important to emphasize the relevance of the institutional structure that performs these procedures, in order to conduct them safely, being able to treat possible and feasible complications.
Keywords: Endoscopy; Esophagogastroduodenoscopy; Child (source: MeSH NLM).
RESUMEN
Objetivo: Presentar y discutir los hallazgos endoscópicos e histológicos, así como la incidencia de Helicobacter pylori y otras enfermedades, indicaciones y características de endoscopia digestiva alta realizada en niños. Material y métodos: Fueron realizadas 225 endoscopias en niños de seis meses a 11 años (media de 7,69 años) a partir de febrero de 2013 hasta enero de 2016. En 200 pacientes, en las endoscopias diagnósticas se llevan a cabo biopsias seriadas (esófago, estómago y duodeno) en 120 de ellos. Resultados: La indicación de endoscopia fue diagnóstica en el 88,89% de los pacientes y en 26 pacientes se realizaron un procedimiento terapéutico. Los hallazgos endoscópicos más frecuentes fueron esofagitis en 49 pacientes, gastritis y duodenitis 84 y en 16 pacientes se diagnosticaron cuatro úlceras duodenales. En endoscopias terapéuticas fueron realizadas seis gastrostomías, catorce extracciones de cuerpos extraños, cinco pasajes de sonda nasogástrica y una dilatación esofágica. El estudio de H. pylori se realizó por el método histopatológico y fué positivo en 26 (13%) de 200 pacientes en los que se han buscado. Conclusión: La endoscopía pediátrica es un nicho importante de la endoscopía digestiva donde es importante enfatizar la relevancia de la estructura institucional que realiza estos procedimientos para conducirlos con seguridad y ser capaces de tratar las complicaciones posibles.
Palabras clave: Endoscopía; Esofagogastroduodenoscopía; Niño (fuente: DeCS BIREME).
INTRODUCTION
Upper digestive endoscopy in children had its onset in the 1970s, and is usually performed by pediatric gastroenterologists. At the end of the 1990s, the North American Society of Pediatric Gastroenterology, Hepatology and Nutrition (NASPGHAN) issued guidelines for trainees to improve the competence of practitioners in this area (1-3).
Some recommendations are essential for endoscopy in children, ranging from orientations to parents about procedural risks, ideal fasting time, and types of equipment for different age groups, as well as contraindications, types of sedation, and after-care from therapeutic procedures (endoscopic dilations, percutaneous gastrostomies, removal of foreign bodies and even sclerotherapy) (1).
An important step in conducting any examination or procedure in children is the informed consent of the parents or responsible adult about the risks that may be present (1).
According to the American Academy of Pediatrics (AAP) guideline and recommendations of the American Society of Anesthesiologists (ASA), clear liquids (including breastmilk but not processed formulas) can be given to children two to three hours before endoscopy in order to avoid dehydration. Children under six months can receive infant formulas four to six hours earlier. For older children, standard fasting lasts from six to eight hours before sedation, for liquids in general, and solid foods (4,5).
Recurrent chronic abdominal pain is a common complaint in pediatrics, for which no organic cause is usually found. Several reports on the relationship between abdominal pain and H. pylori infection are found in the literature, but the results are controversial (6).
In most cases, it is believed that chronic abdominal pain, whose definition is that felt for at least two months, is due to a functional disorder. Chronic functional abdominal pain has two peak periods: the first in 5 - 7 years of age (when 5-8% of children have abdominal pain) and second, from 8 - 12 years of age (up to 25% of patients) When there is a strong predominance of females (7).
Functional CAD is uncommon in children under 5 years of age. Approximately 3 - 8% of cases of isolated CAD are due to organic disease (8). The typical presentation is a child aged 5 to 10 years, with vague periumbilical pain, which can be quite intense, even interrupting normal activities and being associated with nausea, pallor and headache. Epigastric pain is also described. Pain is not related to food intake, activity levels or stool pattern, and usually occurs during the day (8).
The episodes are similar, resolve spontaneously, and the child "works" normally between bouts of pain. Helicobacter pylori in children causes antral gastritis, where it often has nodular appearance, having a prevalence of 30 to 100%, compared with only 0 to 20% in adults. It can be characterized as lymphocytic or neutrophilic. The incidence of peptic ulcer disease in children is low but, as in adults, 90 to 100% of duodenal ulcers are strictly associated with H. pylori infection (9).
MATERIAL AND METHODS
A retrospective study of upper digestive endoscopies in pediatric patients, ranging from six months to eleven years (mean of 7.69 years), both diagnostic and therapeutic, electively or in the 2013 until January 2016). The endoscopy used for all procedures was Pentax EPK 1000 (9.8 mm). Endoscopes of smaller size were not used. The only procedure in children below 15 kg was in an endoscopic gastrostomy, where general sedation was performed under orotracheal intubation.
Outpatient diagnostic and therapeutic exams were performed by a single experienced endoscopist (with more than 20 years of experience), always in the presence of an experienced anesthetist. Anesthesia was performed with intravenous sedation using fentanyl, midazolam and propofol and, when necessary, anesthetic induction by inhalation using sevoflurane.
Urgent endoscopies, such as removals of foreign bodies or passages from nasal infants, were performed by attending physicians on the day of their respective shifts. In an outpatient diagnosis, the clinical complaints were correlated, mostly referred to by parents or caregivers, and the endoscopic and histological findings.
RESULTS
A total of 225 patients aged 6 months to 11 years (mean of 7.69 years with standard deviation of 2.77 years and median of 8 years) were evaluated. One hundred and thirteen (50.2%) patients were male.
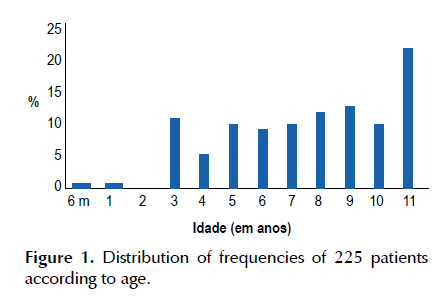
In Figure 1 we present the frequency distribution of 225 patients according to age.
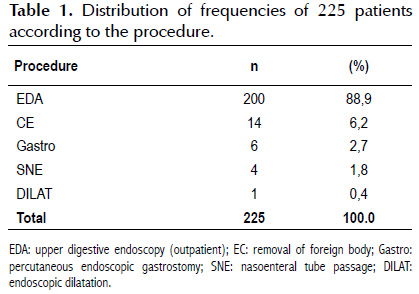
Table 1 presents the frequency distribution of 225 patients according to the procedure to which they were submitted.
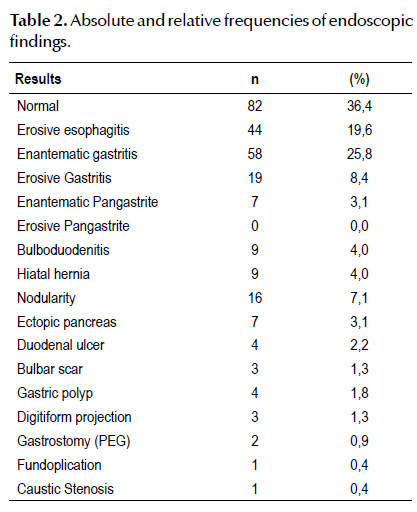
Table 2 shows the absolute and relative frequencies of the endoscopic findings of the exams performed in the outpatient setting.
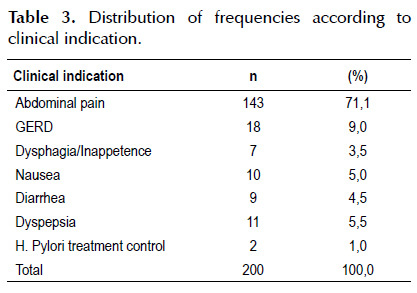
Table 3 presents the frequency distribution of the patients according to the clinical indication of the outpatient diagnostic tests.
In 120 patients (60.3%) biopsies of the esophagus, stomach and duodenum were performed.
In 26 patients (13.1%) the Helicobacter pylori test was positive.
Of the total number of patients, three (1.5%) had celiac disease and two (1%) had eosinophilic esophagitis.
DISCUSSION
Recurrent abdominal pain is the most common cause to perform EGD in the pediatric patient (10-13). It should be investigated when a peptic disease such as ulcer, gastritis or esophagitis is suspected. Since isolated abdominal pain in the school-age child is most often functional, high endoscopy should be considered when it suggests an organic etiology, that is, when it is well localized, epigastric, when it has other associated symptoms such as nausea, vomiting, weight loss, anemia, occult or apparent bleeding, when the patient is awakened at night or when there is a family history of peptic ulcer (14-15).
occurs between six months and three years of age (16).
In general, 80 to 90% of the foreign bodies that enter the stomach pass spontaneously, 10 to 20% require endoscopy and 1% require surgery. Coins seem to be the object most often children swallow.
They should be removed when they remain in the esophagus for more than 24 hours, or when they stay in the stomach for more than 4 weeks (with weekly radiological follow-up). In general, after they pass the card, the coins leave spontaneously (16,17).
The EGD, when diagnosed, is considered a safe procedure and the complications that can occur from it are smaller. Risks increase when endoscopy is performed urgently, when the patient is in critical condition or when there is therapeutic intervention. There is little information available in the literature regarding the rates of complications of pediatric endoscopies (18). Ament (12) reported 1.7% of complications in 2,046 EGD. In our series, we did not have any major complications.
In conclusion, pediatric endoscopy is an important niche of the digestive endoscopy, where it is important to emphasize the relevance of the institutional structure that performs these procedures, in order to conduct them safely, being able to treat possible and feasible complications.
BIBLIOGRAPHIC REFERENCES
1. Friedt M, Welsch S. An update on pediatric endoscopy. Eur J Med Res. 2013;18:24. [ Links ]
2. Thomson M, Elawad M, Barth B, Seo JK, Vieira M. Worldwide strategy for implementation of paediatric endoscopy: Report of the FISPGHAN Working Group. J Pediatr Gastroenterol Nutr. 2012;55(5):636-9. [ Links ]
3. Rudolph CD, Winter HS. NASPGN guidelines for training in pediatric gastroenterology. NASPGN Executive Council, NASPGN Training and Education Committee. J Pediatr Gastroenterol Nutr. 1999;29 Suppl 1:S1-26. [ Links ]
4. ASGE Standards of Practice Committee, Lee KK, Anderson MA, Baron TH, Banerjee S, Cash BD, et al. Modifications in endoscopic practice for pediatric patients. Gastrointest Endosc. 2008;67(1):1-9. [ Links ]
5. American Academy of Pediatrics; American Academy of Pediatric Dentistry, Coté CJ, Wilson S; Work Group on Sedation. Guidelines for monitoring and management of pediatric patients during and after sedation for diagnostic and therapeutic procedures: an update. Paediatr Anaesth. 2008;18(1):9-10. [ Links ]
6. Thakkar K, Gilger MA, Shulman RJ, El Serag HB. EGD in children with abdominal pain: a systematic review. Am J Gastroenterol. 2007;102(3):654-61. [ Links ]
7. Thakkar K, Chen L, Tatevian N, Shulman RJ, McDuffie A, Tsou M, et al. Diagnostic yield of oesophagogastroduodenoscopy in children with abdominal pain. Aliment Pharmacol Ther. 2009;30(6):662-9. [ Links ]
8. Gray L. Chronic abdominal pain in children. Austral Family Phys. 2008;37(4):398-400. [ Links ]
9. Kimia A, Zahavi I, Shapiro R, Rosenbach Y, Hirsh A, Druzd T, et al. The role of Helicobacter pylori and gastritis in children with recurrent abdominal pain. Isr Med Assoc J. 2000;2(2):126-8. [ Links ]
10. Koletzko S, Jones NL, Goodman KJ, Gold B, Rowland M, Cadranel S, et al. Evidence-based Guidelines from ESPGHAN and NASPGHAN for Helicobacter pylori Infection in Children. J Pediatr Gastroenterol Nutr. 2011;53(2):230-43. [ Links ]
11. Gold BD, Gilger MA, Czinn SJ. New diagnostic strategies for detection of helicobacter pylori infection in pediatric patients: discussion. Gastroenterol Hepatol (N Y). 2014;10(12 Suppl 7):1-19. [ Links ]
12. Ament ME, Vargas J. Fiberoptic Upper Intestinal Endoscopy. In: Walker WA. Pediatric Gastrointestinal Disease. 1ª ed. Mosby Year-Book, Inc; 1991. p. 1247-56. [ Links ]
13. Squires RH, Colletti RB. Indications for Pediatric Gastrointestinal Endoscopy: a medical position statement of the North American Society for Pediatric Gastroenterology and Nutrition. J Pediatr Gastroenterol Nutr. 1996;23(2):107-10. [ Links ]
14. Prolla JC, Diehl AS, Benvenuti GA, Loguercio SV, Magalhães DS, Silveira TR. Upper gastrointestinal fiberoptic endoscopy in pediatric patients. Gastrointest Endosc. 1983;29(4):279-81. [ Links ]
15. Benaroch LM, Rudolph CD. Introduction to pediatric esophagogastroduodenoscopy and enteroscopy. Gastrointest Endosc Clin N Am. 1994;4(1):121-42. [ Links ]
16. Byrne WJ. Foreign bodies, bezoars, and caustic ingestion. Gastrointest Endosc Clin N Am. 1994;4(1):99-119. [ Links ]
17. Schwartz GF, Polsky HS. Ingested foreign bodies of the gastrointestinal tract. Am Surg. 1976;42(4):236-8. [ Links ]
18. Fox VL. Upper Gastrointestinal Endoscopy. In: Walker WA. Pediatric Gastrointestinal Disease. 2ª ed. Mosby Year-Book, Inc; 1996. p. 1514-33. [ Links ]
Correspondence:
Diego Soares Coca
Endoscopy Service of Ana Costa Hospital, Rua Pedro Américo, 60, 10th floor - Santos / SP, Brazil.
E-mail: diego_coca@hotmail.com
Recibido: 22-8-2017
Aprobado: 21-2-2018