Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista de Gastroenterología del Perú
Print version ISSN 1022-5129
Rev. gastroenterol. Perú vol.39 no.1 Lima Jan./Mar. 2019
ARTÍCULOS ORIGINALES
Complications After endoscopic balloon dilatation of esophageal strictures in children. Experience from a tertiary center in Shiraz – Iran (Nemazee Teaching Hospital)
Complicaciones posteriores a dilatación endoscópica con balón en niños con estenosis esofágica. Experiencia de un centro de referencia en Shiraz – Iran (Nemazee Teaching Hospital)
Seyed Mohsen Dehghani1, Naser Honar1, Mahsa Sehat1, Hazhir Javaherizadeh2, Iraj Shahramian3, Gholamreza Kalvandi4, Hamid Reza Foroutan5
1 Gastroenterohepatology research center, Nemazee teaching hospital, Shiraz University of Medical Sciences. Shiraz, Iran.
2 Alimentary Tract Research Center, Ahvaz Jundishapur University of Medical Sciences. Ahvaz, Iran
3 Dept. Of Pediatrics, Zabol University of Medical Sciences. Zabol, Iran.
4 Dept. Of Pediatrics, Ilam University of Medical Sciences. Ilam, Iran.
5 Dept. Of Pediatric Surgery, Nemazee Teaching Hospital, Shiraz University of Medical Sciences. Shiraz, Iran.
ABSTRACT
Background: Esophageal stricture is one of the most important complication of the caustic ingestion. Objective: The aim of this study was to evaluate complications of balloon dilatation among children with esophageal stenosis. Material and methods: In this retrospective study 82 children were included. Children who underwent balloon dilatation for esophageal stenosis were included in our study. Duration of study was 14 year starting from 2001. Mean age of the cases was 3.95±0.4 year (Min: 15 days, Max: 14 year). Chart review and telephone calling were the methods of data collection. Data was analyzed using SPSS. Results: In this study, 47% of the patients were male and 53% of the cases were female. Caustic ingestion (33.7%) was the most common etiology for the esophageal stricture. Vomiting (87.8%) was the most common presenting symptom. Among our cases, 76.8% had no compliant after esophageal dilatation. Chest pain was the most common compliant after esophageal dilatation. Response rate was similar among boys and girls. Toddler age had the best treatment response after esophageal dilatation. Conclusion: Among our cases, 76.8% had no post procedural compliant after esophageal dilatation. Esophageal perforation was seen in 4.9% of the cases. Chest pain was the most common post dilatation complication.
Keywords: Gastric balloon; Esophageal stenosis; Niño (source: MeSH NLM).
RESUMEN
Antecedentes: La estenosis esofágica es una de las más importantes complicaciones de la ingesta de caústicos. Objetivo: El objetivo del estudio fue evaluar las complicaciones de la dilatación endoscópica con balón en niños con estenosis esofágica. Material y métodos: En este estudio retrospectivo se incluyeron 82 niños. Se incluyeron todos los niños que se sometieron a una dilatación endoscópica con balón por estenosis esofágica. La duración del estudio fue 14 años iniciando en el año 2001. La edad media de los pacientes fue 3,95 +/- 0,4 años (Min. 15 días, Máx. 14 años). La recolección de datos se realizó revisando las historias clínicas y con llamadas telefónicas. Los datos se analizaron con el Sistema SPSS. Resultados: En este estudio, 47% de los casos fueron varones y 53% fueron mujeres. La ingesta de caústicos fue la causa más frecuente de estenosis esofágica (33,7%). El síntoma más común fueron los vómitos (87,8%). Entre nuestros casos, 76,8% no presentaron molestias luego de la dilatación esofágica. El dolor torácico fue la molestia más común luego de la dilatación esofágica. La tasa de respuesta al tratamiento fue similar entre hombres y mujeres. Los niños pequeños tuvieron la mejor respuesta al tratamiento luego de la dilatación esofágica. Conclusiones: Entre nuestros casos, 76,8% no presentaron molestias luego de la dilatación esofágica. La perforación esofágica se presentó en 4,9% de los casos. El dolor torácico fue la complicación más común posterior a la dilatación.
Palabras clave: Balón gástrico; Estenosis esofágica; Child (fuente: DeCS BIREME).
INTRODUCTION
Esophageal stenosis has different etiology. Caustic ingestion is the one of the most common etiology especially among childhood. Esophageal stricture is the most important late complication of corrosive esophagitis (1,2). Esophageal stenosis may be seen in 20% of children following of ingestion of corrosive material in our country (3). Repaired esophageal atresia may be lead to esophageal stenosis. Esophageal stenosis was reported in 5.9%-21% of neonates who underwent repair of esophageal atresia according to type of esophageal anastomosis (4).
Esophageal dilatation may be performed using Savary dilatation (5) or balloon dilatation. Recently esophageal stents are recommended for some cases. In the study by Lang et al, endoscopic balloon dilatation is preferable to traditional bougienage (6).
Complication following esophageal dilatation such as esophageal perforation (7,8), chest pain, and respiratory problem were reported by researched with various frequencies. The aim of this study was to evaluate complication of balloon dilatation among children with esophageal stenosis.
MATERIAL AND METHODS
In this retrospective study 82 children with esophageal stenosis were included. Duration of the study was 14 year starting from 2001. Patients with esophageal stenosis due to different etiology such as achalasia, caustic ingestion, epidermolysis bullosa, gastroesophageal reflux, and congenital stricture were included. In the current study, children who underwent esophageal dilatation using Balloon were included. These patients were visited due to vomiting, cyanosis, regurgitation, abdominal pain, dysphagia, or cough. Nine cases were excluded due to incomplete follow up.
For each case etiology, sex, age, age at diagnosis, number of dilatation session, post dilatation complication, response to treatment, and duration of follow up were recorded. Some information was obtained via telephone calling. Resolving symptom such as dysphagia, was considered as a treatment response (9), p value < 0.05 was considered significant. This study was approved by ethical committee of the university.
RESULTS
In this study 82 children who underwent esophageal dilatation in our pediatric gastroenterology department, during 2001 till 2013 were included. Age of the cases were between 15 days till 14 years old with mean age 3.95±0.4. Of all cases, 53% were female and 47% were male.
Mean age of onset was 28.1 months. Number of dilatation session was 2.4±1.77 for each case. Number of dilatation session was between 1 till 10 session. Pneumatic balloon was used for 21 (25.3%) of the achalasia cases. TTS balloon was used in 61 (73.5%) of the cases.
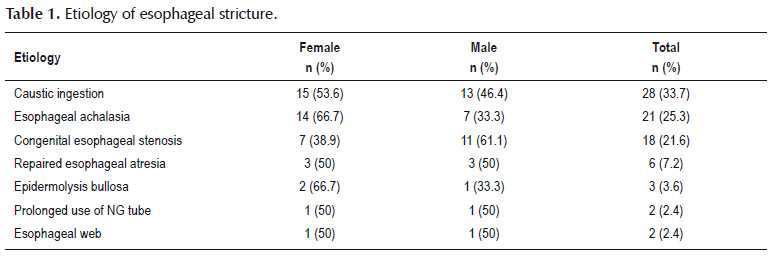
Etiology of the esophageal stricture were shown in Table 1. Vomiting was the most common presenting symptoms in our patients (Table 2).
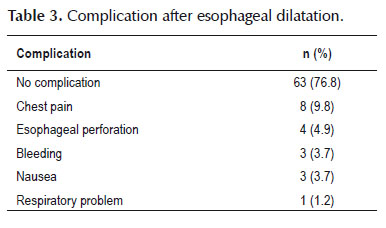
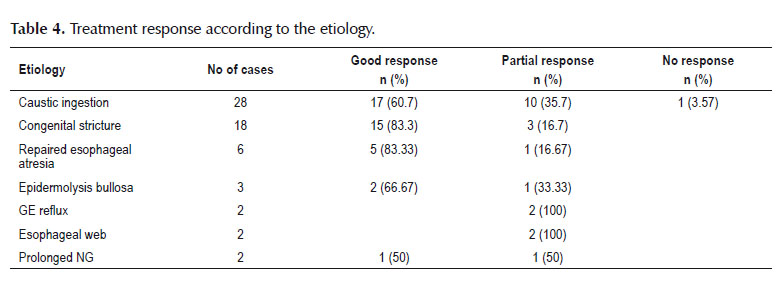
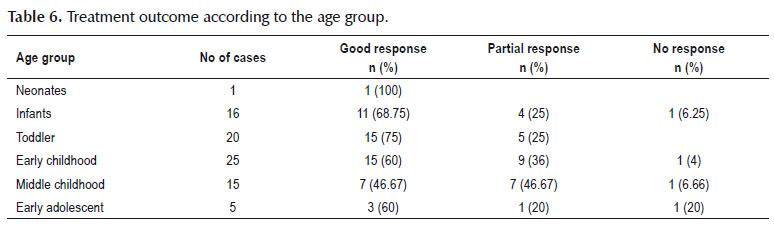
Of the cases, 76.8% had no complication after esophageal dilatation (Table 3). Chest pain was the most post procedural complication (Table 3). Treatment response according to the etiology of esophageal stricture was shown in Table 4. Among children with good response, 51.9 were male and 48.1 were female (Table 5). Treatment response in infants age group was slightly better than other age groups (Table 6).
DISCUSSION
This study was included 82 patients aged 15 days -14 years old in our hospital. Maximum number of dilatation session was 10 in the current study. In the study by Karaman et al., maximum number of dilatation session was 52 (10).
Caustic ingestion were the most common etiology for the children who underwent esophageal dilatation. In another study from Poland, post operative stricture were the most common indication (11).
Bleeding was observed in 3.7% of the patients. In the study by Pieczarkowski and colleagues (11), bleeding was seen in 95 cases of 347 procedures. The rate of bleeding in our study was lower than Pieczarkowski et al. (11). Rate of bleeding was differ between these studies and it was may be due to etiology of esophageal stenosis, experience of pediatric gastroenterology, and associated problem.
Esophageal perforation was seen in 4.9% of patients. In the study by Cakmak et al., esophageal perforation was seen in 10.5% of the cases (12). In Chang et al study on 10 children underwent esophageal dilatations, esophageal perforation was not observed (13). In the study by Lan et al, esophageal perforation were observed in 1.5% of dilatations (14). In a multicenter study from Poland, only one perforation was reported among 347 esophageal dilatations (11). In the study by Contini et al., procedure related perforation was 0.7% (15). In the study by Serhal et al. on 23 children with repaired esophageal atresia and esophageal stricture, no complications were observed during or after dilatation sessions (16). In the study by Doo et al. on 11 children and 36 balloon session, esophageal perforation was occurred in 45% of the patients and 31% of the balloon session (17). In the study by de la Rionda et al., on 30 children aged < 15 years, two perforations were reported (18). In the study by Bicakci et al. on children with caustic ingestion, no perforation was occurred following esophageal dilatation (19). The rate of esophageal perforation in our center was lower than Cakmak et al. (12) study but higher than Lan et al. (14) and Pieczarkowski et al. study (11). Complication following dilatation of stricture due to caustic ingestion may be higher than stricture due repaired esophageal atresia (20). This difference may be due to severity of esophageal stricture or aggressive dilatation. Other factors may include age of the cases and experience of gastroenterologist.
Among children with esophageal achalasia, 57.1% had good response following pneumatic dilatation. Among our patient, 26.6% showed partial response. In the study by Di Nardo et al., pneumatic dilatation achieved 67% success rate (21). The result of two study was similar.
Chest pain was the most frequent complication in our study. Chest pain may be due to pneumothorax due to esophageal perforation or appearance of peristalsis in achalasic patients (22). Chest pain in our study didn’t result to further treatment.
Death after esophageal dilatation was not seen among our cases. One death was reported by Contini et al. (15). Another mortality following esophageal dilatation was reported Güitrón et al. (23) study. They used Savary-Gilliard bougies for esophageal dilatation.
In conclusion, caustic ingestion and esophageal achalasia were the most common etiology of esophageal stenosis requiring esophageal dilatation. Vomiting was the main presenting symptom. Chest pain was the most common complication following esophageal dilatation. Congenital stenosis and repaired esophageal atresia had the highest response compared to the other etiologies. Toddler ages had the higher response in comparison to other age group. Outcome and complication of children with esophageal stricture treated by esophageal dilatation procedures were similar to most pediatric gastroenterology centers in the world.
Limitation: Single center study and duration of follow up. Etiology of esophageal stenosis were hetrogen.
Acknowledgment:This study was supported by research affair of Shiraz University of Medical Sciences. The source of data used in this article was research thesis no of Mahsa Sehat (no# 91-01-01-84) for general physician degree.
Conflict of interest: There was nothing.
BIBLIOGRAPHIC REFERENCES
1. Yararbai O, Osmanodlu H, Kaplan H, Tokat Y, Coker A, Korkut M, et al. Esophagocoloplasty in the management of postcorrosive strictures of the esophagus. Hepatogastroenterology. 1998;45(19):59-64. [ Links ]
2. Kim JH, Song HY, Kim HC, Shin JH, Kim KR, Park SW, et al. Corrosive esophageal strictures: long-term effectiveness of balloon dilation in 117 patients. J Vasc Interv Radiol. 2008;19(5):736-41. [ Links ]
3. Honar N, Haghighat M, Mahmoodi S, Javaherizadeh H, Kalvandi G, Salimi M. Caustic ingestion in children in south of Iran. Retrospective study from Shiraz - Iran. Rev Gastroenterol Peru. 2017;37(1):22-5. [ Links ]
4. Askarpour S, Ostadian N, Peyvasteh M, Alavi M, Javaherizadeh H. End-to-end versus end-to-side anastomosis in the treatment of esophageal atresia or tracheo-esophageal fistula. Arq Bras Cir Dig. 2016;29(1):48-9. [ Links ]
5. Al-Hussaini A. Savary Dilation Is Safe and Effective Treatment for Esophageal Narrowing Related to Pediatric Eosinophilic Esophagitis. J Pediatr Gastroenterol Nutr. 2016;63(5):474-480. [ Links ]
6. Lang T, Hummer HP, Behrens R. Balloon dilation is preferable to bougienage in children with esophageal atresia. Endoscopy. 2001;33(4):329-35. [ Links ]
7. McCann F, Michaud L, Aspirot A, Levesque D, Gottrand F, Faure C. Congenital esophageal stenosis associated with esophageal atresia. Dis Esophagus. 2015;28(3):211-5. [ Links ]
8. Shehata SM, Enaba ME. Endoscopic dilatation for benign oesophageal strictures in infants and toddlers: experience of an expectant protocol from North African tertiary centre. Afr J Paediatr Surg. 2012;9(3):187-92. [ Links ]
9. Youn BJ, Kim WS, Cheon JE, Kim WY, Shin SM, Kim IO, et al. Balloon dilatation for corrosive esophageal strictures in children: radiologic and clinical outcomes. Korean J Radiol. 2010;11(2):203-10. [ Links ]
10. Karaman I, Koc O, Karaman A, Erdoğan D, Çavuşoğlu YH, Afşarlar ÇE, et al. Evaluation of 968 children with corrosive substance ingestion. Indian J Crit Care Med. 2015;19(12):714-8.
11. Pieczarkowski S, Woynarowski M, Landowski P, Wilk R, Daukszewicz A, Toporowska-Kowalska E, et al. Endoscopic therapy of oesophageal strictures in children – a multicentre study. Prz Gastroenterol. 2016;11(3):194-9. [ Links ]
12. Cakmak M, Boybeyi O, Gollu G, Kucuk G, Bingol-Kologlu M, Yagmurlu A, et al. Endoscopic balloon dilatation of benign esophageal strictures in childhood: a 15-year experience. Dis Esophagus. 2016;29(2):179-84. [ Links ]
13. Chang CF, Kuo SP, Lin HC, Chuang CC, Tsai TK, Wu SF, et al. Endoscopic balloon dilatation for esophageal strictures in children younger than 6 years: experience in a medical center. Pediatr Neonatol. 2011;52(4):196-202. [ Links ]
14. Lan LC, Wong KK, Lin SC, Sprigg A, Clarke S, Johnson PR, et al. Endoscopic balloon dilatation of esophageal strictures in infants and children: 17 years’ experience and a literature review. J Pediatr Surg. 2003;38(12):1712-5.
15. Contini S, Garatti M, Swarray-Deen A, Depetris N, Cecchini S, Scarpignato C. Corrosive oesophageal strictures in children: outcomes after timely or delayed dilatation. Dig Liver Dis. 2009;41(4):263-8. [ Links ]
16. Serhal L, Gottrand F, Sfeir R, Guimber D, Devos P, Bonnevalle M, et al. Anastomotic stricture after surgical repair of esophageal atresia: frequency, risk factors, and efficacy of esophageal bougie dilatations. J Pediatr Surg. 2010;45(7):1459-62. [ Links ]
17. Doo EY, Shin JH, Kim JH, Song HY. Oesophageal strictures caused by the ingestion of corrosive agents: effectiveness of balloon dilatation in children. Clin Radiol. 2009;64(3):265-71. [ Links ]
18. De la Rionda L, Fragoso T, Sagaro E, Delgado B, Larramendi O, Borbolla E. Treatment with Savary-Gilliard bougies in esophageal stenosis in children. Rev Gastroenterol Peru. 1995;15(2):152-7. [ Links ]
19. Bicakci U, Tander B, Deveci G, Rizalar R, Ariturk E, Bernay F. Minimally invasive management of children with caustic ingestion: less pain for patients. Pediatr Surg Int. 2010;26(3):251-5. [ Links ]
20. Yeming W, Somme S, Chenren S, Huiming J, Ming Z, Liu DC. Balloon catheter dilatation in children with congenital and acquired esophageal anomalies. J Pediatr Surg. 2002;37(3):398-402. [ Links ]
21. Di Nardo G, Rossi P, Oliva S, Aloi M, Cozzi DA, Frediani S, et al. Pneumatic balloon dilation in pediatric achalasia: efficacy and factors predicting outcome at a single tertiary pediatric gastroenterology center. Gastrointest Endosc. 2012;76(5):927-32. [ Links ]
22. Papo M, Mearin F, Castro A, Armengol JR, Malagelada JR. Chest pain and reappearance of esophageal peristalsis in treated achalasia. Scand J Gastroenterol. 1997;32(12):1190-4. [ Links ]
23. Guitron A, Adalid R, Nares J, Mena G, Gutiérrez JA, Olivares C. [Benign esophageal strictures in toddlers and pre-school children. Results of endoscopic dilation]. Rev Gastroenterol Mex. 1999;64(1):12-5. [Article in Spanish] [ Links ]
Correspondence:
Hazhir Javaherizadeh
Address: Abuzar Children’s Hospital, Dept. of Pediatric Gastroenterology, Ahvaz Jundishapur University of Medical Sciences, Ahvaz, Iran
E-mail: Hazhirja@ajums.ac.ir, Hazhirja@yahoo.com
Recibido: 18.06.18
Aprobado:18.03.19