Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista de Gastroenterología del Perú
Print version ISSN 1022-5129
Rev. gastroenterol. Perú vol.39 no.2 Lima Apr./Jun. 2019
ARTÍCULOS ORIGINALES
Preferential usage of rifaximin for the treatment of hydrogen-positive small intestinal bacterial overgrowth
Rifaximina como tratamiento de elección en pacientes con sobrecrecimiento bacteriano con prueba de hidrógeno positiva
Jodie A Barkin1, Tara Keihanian1, Jamie S Barkin1, Carol M Antequera1, Baharak Moshiree2
1 Division of Gastroenterology, Department of Medicine, Leonard M. Miller School of Medicine, University of Miami. Miami, Florida, USA.
2 Division of Gastroenterology, Carolinas HealthCare System, University of North Carolina. Charlotte, North Carolina, USA.
ABSTRACT
Objectives: Small intestinal bacterial overgrowth (SIBO) is challenging to treat and diagnose and is associated with diagnosis of irritable bowel syndrome (IBS). Although no FDA-approved medications exist for treatment of SIBO, rifaximin has recently received approval to treat diarrhea-predominant IBS and patients with methane-positive SIBO breath tests. The aim of this study is to evaluate patient response to rifaximin for SIBO based on breath test results. Materials and methods: All patients underwent breath testing to evaluate for SIBO during a 42-month period. Patients were defined as having a positive glucose breath test for SIBO based on an increase of ≥ 20 ppm of hydrogen and/or ≥ 10 ppm of methane 90 minutes after ingesting glucose. Patient demographic and symptom data, antibiotic treatment regimens, symptomatic response to therapy, and repeat treatments were recorded. Institutional review board approval was obtained. Results: A total of 53 of 443 patients had positive breath testing for SIBO. Response rates to rifaximin (550 mg three times daily for 14 days) were 47.4% for hydrogen positivity alone and 80% for both hydrogen and methane positivity. Conclusions: Rifaximin was the most commonly prescribed antibiotic regimen for SIBO therapy. Patients with hydrogen or hydrogen and methane positive breath tests responded well to rifaximin therapy. For patients with hydrogen-positive SIBO, rifaximin may prove a highly effective therapy in providing symptom relief from the effects of SIBO.
Keywords: Irritable bowel syndrome; Rifaximin; Therapy; Antibiotic (source: MeSH NLM).
RESUMEN
Objetivos: El sobrecrecimiento bacteriano de intestino delgado es una entidad difícil de diagnosticar y tratar, frecuentemente asociada con el síndrome de intestino irritable. A pesar que la FDA no ha aprobado medicamentos para tratar el sobrecrecimiento bacteriano, la rifaximina ha sido recientemente aprobada para tratar el intestino irritable tipo diarrea y en pacientes con test de aliento metano positivo en sobrecrecimiento bacteriano. El objetivo del estudio fue evaluar la respuesta a rifaximina de los pacientes con sobrecremiento bacteriano con prueba de aliento positiva. Material y métodos: Todos los pacientes que se realizaron prueba de aliento por sobrecrecimiento bacteriano durante un periodo de 42 meses. Se definió un paciente con sobrecrecimiento bacteriano positivo si tenía un incremento mayor a 20 ppm de hidrógeno y/o 10 ppm de metano luego de 90 minutos de la ingesta de glucosa. Se registraron los datos demográficos, síntomas, tratamiento antibióticos recibidos, respuesta a la terapia, y repetición de tratamientos. Resultados: Un total de 53 de 443 pacientes tuvieron prueba de aliento positiva para sobrecrecimiento bacteriano. La tasa de respuesta a rifaximina (550 mg tres veces x día x 14 días) fue 47.4% para pacientes con sólo test de hidrógeno positivo, y 80% para pacientes con tanto test de hidrógeno como metano positivos. Conclusiones: La rifaximina es el régimen antibiótico más frecuentemente utilizado en sobrecrecimiento bacteriano. Los pacientes con prueba de aliento de hidrógeno o hidrógeno y metano positivos respondieron bien a la rifaximina. Para pacientes con sobrecrecimiento bacteriano prueba de hidrógeno positiva, la rifaximina puede ser una terapia efectiva en mejorar síntomas.
Palabras calve: Síndrome del colon irritable; Rifaximina; Terapia; Antibiótico (fuente: DeCS BIREME).
INTRODUCTION
Small intestinal bacterial overgrowth (SIBO) is a gastrointestinal condition which remains challenging to both treat and diagnose. Patients often suffer from diarrhea and abdominal bloating, amongst other symptoms. SIBO has been associated with a diagnosis of irritable bowel syndrome (IBS), and may have overlapping symptomatology (1-3). Further, SIBO has been associated with multiple medical conditions including chronic pancreatitis, celiac disease, gastrointestinal dysmotility, and even obesity with alterations in visceral to subcutaneous fat ratios (4-8). Currently, no Food and Drug Administration (FDA) approved medications exist for the treatment of SIBO. However, the FDA has approved rifaximin for the treatment of diarrhea-predominant IBS. Additionally, rifaximin has been recommended for the treatment of patients with methane-positive SIBO breath tests (9). This retrospective study evaluates patients’ symptom responses to rifaximin for SIBO using breath test results, with a specific focus on treatment response in patients with hydrogen-positive breath tests.
MATERIALS AND METHODS
All patients undergoing breath testing to evaluate for SIBO at our tertiary-care motility center from September, 2012 through March, 2016 were evaluated for inclusion in the study. Retrospective review of breath test results followed by chart review in the electronic medical record was performed. Breath testing was performed using standardized protocol.
Breath test protocol:
Patients fasted for at least 12 hours prior to performing the breath test. Patients undergoing breath testing were instructed to avoid the following: i. High fiber foods on the day before the procedure; ii. Antibiotics for 4 weeks prior to the test; and iii. Smoking on the day of the breath testing. Patients ingested an oral solution of 75 grams glucose (or fructose if diabetic) in 150 mL of water. Breath samples were collected at baseline and every 15 minutes after glucose administration for 1 hour, then every 30 minutes for the next two hours. Hydrogen, methane and carbon dioxide levels were measured simultaneously during breath testing. Samples were analyzed in a QuinTron breath tracker microanalyzer (QuinTron Instrument Company Inc., Milwaukee, Wisconsin USA). All breath tests were performed by one experienced motility technician and nurse and interpreted by one experienced gastroenterology motility specialist physician.
Patients were defined as having a positive glucose or fructose breath test for SIBO if the test revealed an increase of ≥ 20 ppm of hydrogen within 90 minutes and/or an increase of ≥ 10 ppm of methane within 90 minutes, based on standardized criteria (10). Only patients with breath testing positive for SIBO were included in the study as those with a negative study were not treated with antibiotics. Data were recorded for breath test results with hydrogen, methane, or hydrogen and methane positivity. Additional data was then retrospectively recorded from the health system’s electronic medical record, including patient demographics such as age and gender, patient symptoms/indication for breath testing, antibiotic treatment regimens prescribed, symptomatic response to each antibiotic therapy, and repeat antibiotic treatment regimens and response.
Institutional review board approval was obtained for this study.
RESULTS
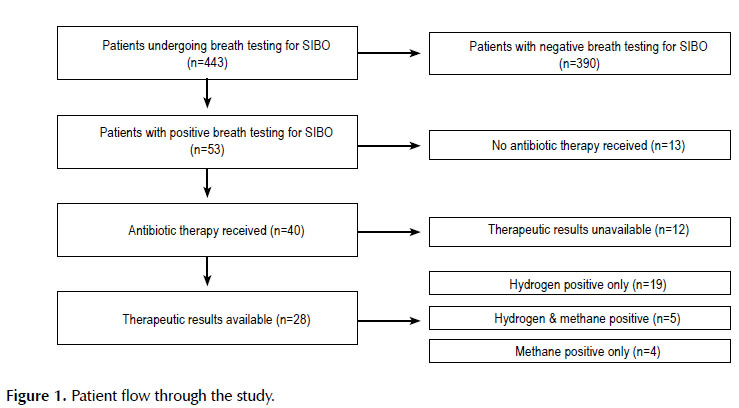
Four hundred and forty-three patients underwent breath testing for SIBO during the study period. Of these patients, 12.0% had positive breath testing for SIBO (Figure 1). Within this 12% of patients, 79.2% were women with a mean age of 58 years (range 16-86 years; SD 16.7 years). The most common symptomatic indications for patients who underwent breath testing were abdominal bloating (60.4%), diarrhea (47.2%), excessive flatulence (30.2%), abdominal pain (24.5%), nausea (22.6%), and constipation (20.8%). Of those with positive breath testing for SIBO, 75.5% had received antibiotic therapy by chart review.
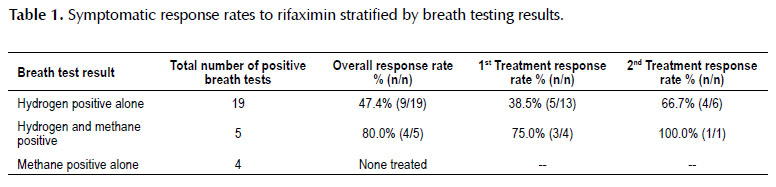
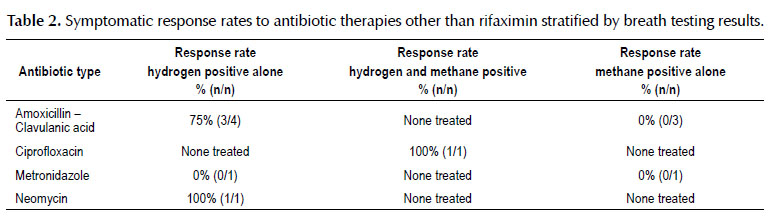
Therapeutic results post-antibiotic course were available in 66.7% of patients who tested positive for SIBO. Of this group, 19 had predominantly hydrogenpositive breath tests, 4 had methane-positive breath tests, and 5 had breath testing positive for both hydrogen and methane. In our population, rifaximin was the most commonly prescribed antibiotic regimen, with 78.4% of patients having taken the antibiotic. The rifaximin regimen used was 550 mg by mouth three times daily for 14 days. Symptomatic response was defined by resolution of the symptoms for which breath testing was indicated in the electronic medical record. Symptomatic response rates to rifaximin were investigated and recorded (Table 1). Response rates to additional antibiotics were catalogued as well (Table 2). For the 19 patients with hydrogen positivity alone on breath testing, the overall response rate to rifaximin was 47.4%, with 38.5% of patients having taken rifaximin as a first antibiotic treatment and 66.7% as a second antibiotic treatment regimen. For the 5 patients with both hydrogen and methane positivity on breath testing, the overall response rate to rifaximin rose to 80.0%, with 75% of patients having received the medication as a first as antibiotic treatment and 100% of patients as a second antibiotic treatment regimen. In our study population, none of the 4 patients with methane positivity alone on breath testing were treated with rifaximin. The aggregate response rate to rifaximin for patients with either hydrogen or hydrogen and methane positive breath testing in our population was 54.2%.
DISCUSSION
Patients with hydrogen or hydrogen and methane positive breath tests had symptomatic response to rifaximin, consistent with previous studies(11-14). Rifaximin was first shown to have efficacy for treatment of SIBO by Di Stefano et al. in 2000 (11). Di Stefano contrasted rifaximin with chlortetracycline, noting rifaxmin resulted in a 70% eradication rate of SIBO on repeat breath testing, contrasted with chlortetracycline’s 27% rate. The same study noted patients in the rifaximin group experienced a significant reduction in hydrogen production, as well as in overall mean number of flatus episodes and abdominal girth compared to patients in the chlortetracycline group (11). The higher reported response rate to rifaximin, compared with our study’s results, may be due to the short interval follow-up at 7 days with more durable symptom response rates potentially waning over time. Unfortunately, in our study, we did not repeat breath testing once symptoms resolved post antibiotic treatment. Similarly, Long and DiPalma’s study of lactulose breath testing in patients positive for SIBO found 74.2% of patients had symptomatic response to a course of rifaximin, although results were not stratified in their study based upon elevations in hydrogen, methane, or both hydrogen and methane positivity (12). The results of both of these studies do further substantiate our more modest results, showing the benefit of rifaximin therapy in hydrogenpositive SIBO.
Hydrogen-positive SIBO response rates to rifaximin in our population were similar to prior TARGET 3 Study data that showed a 44.1% initial response rate to rifaximin in diarrhea-predominant IBS, again suggesting overlap with SIBO (15). Other studies have also suggested rifaximin as a therapeutic option for methane-positive SIBO, providing a synergistic benefit from combination therapy of rifaximin and neomycin, increasing the symptom response rate to 85% with the combined medications (9). Low et al.’s study (9) showed a patient response rate of 56% in the rifaximin-only therapy, similar to our 47.4% response rate in hydrogen-positive patients. Taken together these studies indicate that, while rifaximin is by no means a "cure-all" therapy for all types of SIBO, differences in therapeutic response to rifaximin between patients with either hydrogen- or methane-positive breath testing may be minimal.
Subsequent to the performance of our study, a metaanalysis was published by Gatta et al. examining the efficacy of rifaximin as an antibiotic treatment for SIBO (13). Their meta-analysis encompassed 32 studies of 1,331 total patients diagnosed with SIBO. The overall eradication rate according to intention-to-treat analysis was 70.8%, and improvement or resolution of symptoms in patients with eradicated SIBO was found to be 67.7% (95% CI: 44.7-86.9). The aggregate response rate to rifaximin in Gatta et al.’s (13) meta-analysis is similar to our rate of 54.2%, and further confirms our results. The difference between the two rates may lie in the marked heterogeneity among studies included in the meta-analysis (I2 value=91.3%), and due to almost half of those in the meta-analysis also having concomitant IBS. A prior meta-analysis of 8 studies examining breath testing normalization rate with antibiotic therapy showed that the aggregate response rate to rifaximin was 49.5% again confirming our results; however, the review authors noted the small sample size and marked heterogeneity amongst the included studies in the review and meta-analysis (14).
Given the low prevalence of SIBO, our study’s small sample size is consistent with the sizes of other study populations but may limit the wider applicability of our results. As a retrospective study, it omitted followup data on some patients, as well as a prospective comparison between responses to treatment based on hydrogen-or methane-positivity on breathtesting. Our study is limited due to its retrospective nature on the nuances of the response to treatment, as responses to treatment were identified by review of the electronic medical record with notations often times of improvement in a constellation of prior symptoms without specific delineation of one symptom compared to another. Further, given the retrospective nature, repeat breath testing was not performed to confirm eradication based on routine clinical practice as this is not standard of care, and therefore clinical response was defined via improvement in symptoms. In future comparative prospective studies, investigators may consider the merits of repeat breath testing for confirmation of eradication. Due to the small sample size, head-to-head comparisons between different antibiotic regimens could not be performed. Lastly, given the retrospective nature and small numbers, variability in choice of first line antibiotics and perhaps insurance approval of prescribed therapy may impact the prescribing patterns and results.
Our study’s long duration and follow-up represent an important first step toward establishing the basis for future prospective trials on antibiotic therapies with non-systemic antibiotics such as rifaximin which are suited to patients with SIBO across different outcomes on breath-testing. For patients with hydrogen-positive SIBO, rifaximin may prove a highly effective therapy in providing symptom relief from the effects of SIBO.
Conflicts of interest: Dr. Moshiree reports grants and personal fees from Synergy pharmaceuticals, personal fees from Ferring pharmaceuticals, grants and personal fees from Medtronic, grants and personal fees from Medical QOL, grants and personal fees from Cairin Diagnostics, grants from Allergan/Ironwood, grants from Prometheus Lab, outside the submitted work. The remaining authors report no relevant conflicts of interest nor financial disclosures.
Financial support: No external study funding was provided.
REFERENCES
1. Giamarellos-Bourboulis EJ, Pyleris E, Barbatzas C, Pistiki A, Pimentel M. Small intestinal bacterial overgrowth is associated with irritable bowel syndrome and is independent of proton pump inhibitor usage. BMC Gastroenterol. 2016;16(1):67. [ Links ]
2. Ghoshal UC, Srivastava D. Irritable bowel syndrome and small intestinal bacterial overgrowth: meaningful association or unnecessary hype. World J Gastroenterol. 2014;20(10):2482-91. [ Links ]
3. Ghoshal UC, Shukla R, Ghoshal U. Small Intestinal Bacterial Overgrowth and Irritable Bowel Syndrome: A Bridge between Functional Organic Dichotomy. Gut Liver. 2017;11(2):196- 208. [ Links ]
4. Fialho A, Fialho A, Thota P, McCullough A, Shen B. Higher visceral to subcutaneous fat ratio is associated with small intestinal bacterial overgrowth. Nutr Metab Cardiovasc Dis. 2016;26(9):773-7. [ Links ]
5. Roland BC, Ciarleglio MM, Clarke JO, Semler JR, Tomakin E, Mullin GE, et al. Small Intestinal Transit Time Is Delayed in Small Intestinal Bacterial Overgrowth. J Clin Gastroenterol. 2015;49(7):571-6. [ Links ]
6. Ghoshal UC, Srivastava D, Verma A, Misra A. Slow transit constipation associated with excess methane production and its improvement following rifaximin therapy: a case report. J Neurogastroenterol Motil. 2011;17(2):185-8. [ Links ]
7. Losurdo G, Marra A, Shahini E, Girardi B, Giorgio F, Amoruso A, et al. Small intestinal bacterial overgrowth and celiac disease: A systematic review with pooled-data analysis. Neurogastroenterol Motil. 2017;29(6). [ Links ]
8. Capurso G, Signoretti M, Archibugi L, Stigliano S, Delle Fave G. Systematic review and meta-analysis: Small intestinal bacterial overgrowth in chronic pancreatitis. United European Gastroenterol J. 2016;4(5):697-705. [ Links ]
9. Low K, Hwang L, Hua J, Zhu A, Morales W, Pimentel M. A combination of rifaximin and neomycin is most effective in treating irritable bowel syndrome patients with methane on lactulose breath test. J Clin Gastroenterol. 2010;44(8):547- 50. [ Links ]
10. Rezaie A, Buresi M, Lembo A, Lin H, McCallum R, Rao S, et al. Hydrogen and Methane-Based Breath Testing in Gastrointestinal Disorders: The North American Consensus. Am J Gastroenterol. 2017;112(5):775-84. [ Links ]
11. Di Stefano M, Strocchi A, Malservisi S, Veneto G, Ferrieri A, Corazza GR. Non-absorbable antibiotics for managing intestinal gas production and gas-related symptoms. Aliment Pharmacol Ther. 2000;14(8):1001-8. [ Links ]
12. Long SK, DiPalma JA. Does carbohydrate challenge testing predict clinical response in small intestinal bacterial overgrowth? South Med J. 2016;109(5):296-9. [ Links ]
13. Gatta L, Scarpignato C, Systematic review with meta-analysis: rifaximin is effective and safe for the treatment of small intestine bacterial overgrowth. Aliment Pharmacol Ther. 2017;45(5):604-16. [ Links ]
14. Shah SC, Day LW, Somsouk M, Sewell JL. Meta-analysis: antibiotic therapy for small intestinal bacterial overgrowth. Aliment Pharmacol Ther. 2013;38(8):925-34. [ Links ]
15. Lembo A, Pimentel M, Rao SS, Schoenfeld P, Cash B, Weinstock LB, et al. Repeat Treatment With Rifaximin Is Safe and Effective in Patients With Diarrhea-Predominant Irritable Bowel Syndrome. Gastroenterology. 2016;151(6):1113-21. [ Links ]
Correspondence:
Jodie A Barkin MD
University of Miami, Leonard M. Miller School of Medicine
Department of Medicine, Division of Gastroenterology 1120 NW 14th Street
Clinical Research Building, Suite 1188 (D-49) Miami, Florida 33136 USA
E-mail: jabarkin@med.miami.edu
Recibido: 10.10.18
Aprobado: 10.06.19