Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista de Gastroenterología del Perú
Print version ISSN 1022-5129
Rev. gastroenterol. Perú vol.39 no.2 Lima Apr./Jun. 2019
REPORTE DE CASO
A rare case of recurrent acute pancreatitis after EUS-FNA in a patient with pancreatic intraepithelial neoplasia type 2
Un raro caso de pancreatitis aguda recurrente después de EUS-FNA en un paciente con neoplasia intraepitelial tipo 2
José Celso Ardengh1,2 Filadelfio Venco2, Otácio Micelli-Neto1, Eloy Taglieri1, Eliane Teixeira Orsini1, Rafael Kemp3, José Sebastião dos Santos3, Karol Alejandra Valdivia López3
1 Department of Anatomy and Surgery, Hospital das Clínicas, Medical School of Ribeirão Preto University of São Paulo. São Paulo, Brazil.
2 Pathological Laboratory Diagnostika, Department of Endoscopy Hospital 9 de Julho. São Paulo, Brazil.
3 Endoscopy Service, Hospital Heliópolis. São Paulo, Brazil.
ABSTRACT
Pancreatic intraepithelial neoplasia (PanIN) is considered a pre-malignant lesion difficult to identify by imaging methods. EUS- FNA is an effective technique to obtain material for histopathological study of pancreatic cystic tumors, but it is not free of adverse events. We report a case of a 56 years old patient, with chronic abdominal pain (early 1994). MRI showed pancreatic cystic images. The etiologic diagnosis was doubtful and EUS-FNA was performed. Immediately after a FNA, patient had an episode of acute pancreatitis, requiring hospitalization. During one year after FNA he had five episodes of AP. A new EUS suspected of PanIN, which was confirmed by surgery. After surgery the patient is well and has no more episodes of AP. Although the risk of AP, EUS-FNA should be performed to determine the best treatment for these patients with chronic abdominal pain who have cystic changes of pancreatic gland.
Keywords: Pancreatic ducts; Pancreatitis; Pancreatic neoplasms; Endosonography; Fine needle aspiration (source: MeSH NLM).
RESUMEN
La neoplasia intraepithelial pancreática (PanIN) es considerada una lesión premaligna con dificultad diagnostica mediante métodos imagenlógicos. La EUS-FNA es una técnica efectiva para obtener material para el estudio histopatológico de tumores quísticos pancreáticos, pero no está libre de efectos adversos. Nosotros reportamos un caso de un paciente de 56 años de edad, con dolor abdominal cronico (desde 1994). En la resonancia abdominal se observó un quiste pancreático. El diagnostico etiológico fue dudoso y EUS-FNA fue realizada, después de la cual el paciente presento un cuadro de pancreatitis, requiriendo hospitalización. Durante el periodo de un año posterior a la FNA, éste presento cinco episodios de pancreatitis aguda. Un nuevo estudio ecoendoscopico dio la sospecha de PanIN, la cual se confirmó con la realización de la cirugía. Después de la cirugía quedo asintomático y sin presentar nuevos episodios de pancreatitis aguda hasta el momento. Aunque exista riego de pancreatitis aguda, la EUS-FNA debe realizarse para determinar el mejor tratamiento para pacientes con dolor abdominal crónico que tienen cambios quísticos de la glándula pancreática.
Palabras clave: Conductos pancreáticos; Pancreatitis; Cáncer pancreático; Endosonografía; Biopsia con aguja fina (fuente: DeCS BIREME).
INTRODUCTION
Endosonography-guided fine needle aspiration (EUS-FNA) is effective technique to obtain material for pathological studies in patients with pancreatic cystic lesions (1). Because low risk of developing acute pancreatitis (AP) after procedure, it has been used in place of brushing guided by endoscopic retrograde cholangiopancreatography (ERCP) (2). In addition, it provides superior results for etiological diagnosis of these tumors, compared to percutaneous biopsy techniques guided by abdominal ultrasound (US) or helical computerized tomography (CT), which gives effectiveness for its use (3,4). It is safe with a low rate of complications, ranging from 0.3 to 5% (5).
Perforation, hemorrhage, AP and a case of tumor cells seeding (6) at needle’s route has been described after this technique. An important fact is that even with introduction of fine needle aspiration and guided biopsy technique; a study showed there is no statistical difference between diagnostic EUS and EUS-FNA related to episodes of AP after aspiration which is rare, up to 2% (7).
There are few publications and scarce data to demonstrate the occurrence of AP after EUS-FNA in pancreatic cystic lesions tumors (8-10). One study suggests that patients with a history of AP might be more likely to develop it (7). In any case the risk factors for the AP after EUS-FNA are unknown, and the frequency and severity of episodes vary from one center to another and must be related to practitioner’s experience (11,12).
We describe a case of pancreatic intraepithelial neoplasia (PanIN) with an recurrent episodes of AP after EUS-FNA. Based on scientific evidence the authors discuss its occurrence and risk factors for AP.
CASE REPORT
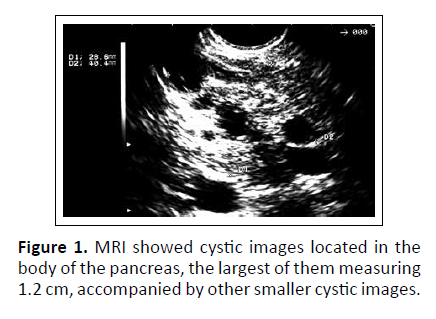
Caucasian male patient, 56 years old, complained of abdominal pain since 1994. Reported colonic diverticular disease for 15 years and nephrolithiasis. He smoked for over 20 years and said to be a social drinker. In 2001 presented high intensity abdominal pain and underwent CT which revealed hypodense areas in the body of pancreas. Medical treatment was performed with improvement in clinical status. Two years later, he had a new episode similar to previous. Another abdominal CT scan showed diverticulitis, swelling and changes in fat surrounding pancreatic tail. Magnetic resonance imaging of abdomen (MRI) revealed small cystic images in the body, along with dilation and tortuosity of main pancreatic duct (MPD) and branch duct (Figure 1). EUS-FNA was indicated to evaluate the cystic lesion and obtain material for pathological examination.
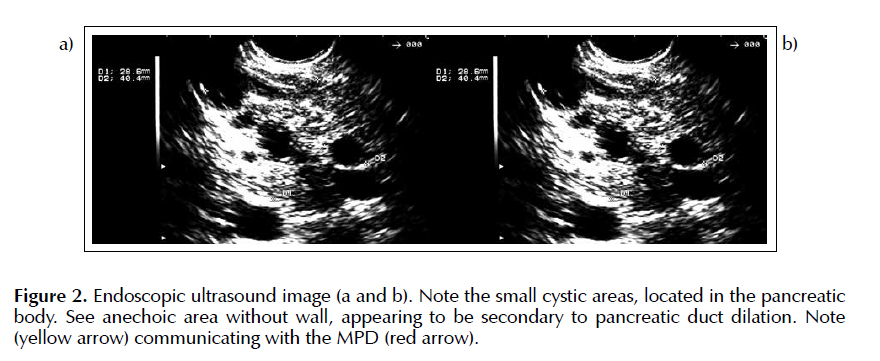
In the body we saw MPD dilation (33 mm). We noted numerous cystic areas, communicating with MPD, and the largest one reached 17 x 8 mm (Figure 2a and 2b). The lesion together (macrocystic and microcystic areas) had 26 mm. The diagnosis of EUS associated with the appearance of fluid aspirated reinforced the suspicion of branch-duct intraductal papillary mucinous tumor of the pancreas. The pathological examination was negative for malignancy, with rare leukocytes, scanty degenerate red blood cells and amorphous proteinaceous material.
Two hours after procedure, patient had intensive abdominal cramps in mesogastrium, radiating to the back, accompanied by nausea and vomiting refractory to analgesics and antispasmodics. Deep abdominal palpation revealed rigidity and severe pain in mesogastrium. Immediately, he was admitted and laboratory tests revealed: high levels of amylase (3x normal) and lipase (3x normal). Plain X-ray in upright position and both hemidiaphragm were normal. The clinical picture associated with laboratory tests showed AP after EUS-FNA. A symptomatic medical treatment was imposed along with antibiotics. Patient remained under medical care until painful symptoms disappear, and was discharged in good condition after 5 days of stay. In July of the same year he presented abdominal pain radiation to the back and located in LIF. CT showed increased pancreatic volume with small hypodense lesions without contrast enhancing. The largest one measured 18 mm. Amylase and lipase were normal. CEA- 1.62 mg / ml and CA 19-9- 12 U / ml, also were normal.
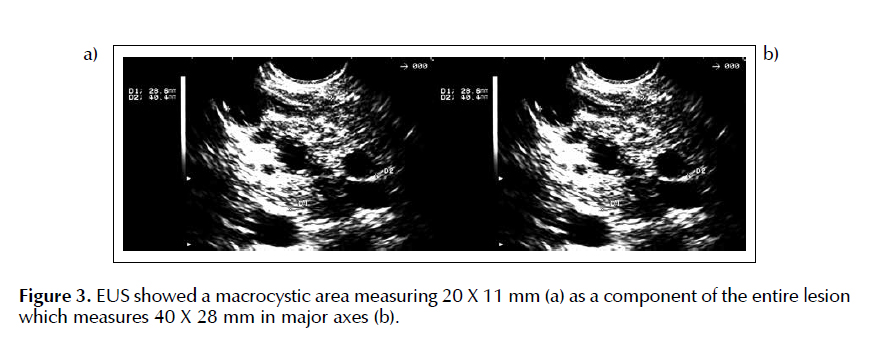
One year after presented four episodes of abdominal pain accompanied by increased amylase and lipase (2x normal). This situation led the doctor to request a new EUS. The examination revealed a cyst 20 mm length and other smaller cysts. It measured 40 x 28 mm in its major axes, with dilatation of secondary ducts (Figure 3a and 3b). The other regions were normal.
Based on EUS results patient was referred for surgery, undergoing subtotal pancreatectomy without complications and with good outcome. Macroscopic analysis of surgical specimen showed a segment of pancreatic body measuring 90 x 50 x 15 mm, with a nodular, soft and slightly purplish and bosselated lesion measuring 35 x 15 x 15 mm. This lesion was adjacent to MPD, which was dilated. Final diagnosis was pancreatic intraepithelial neoplasia (PanIN type II) with ductal adenomatous papillary hyperplasia, without atypical changes. Patient had good outcome and now, after 12 years is doing well.
DISCUSSION
EUS-FNA is being increasingly used for diagnosis of different pancreatic cystic lesions (3). The risks associated with this procedure are low (5,8). The technique is safe with low rate of complications, ranging from 0.3% to 5% (11). These complication rates are equivalent to those of upper digestive endoscopy (13) and colonoscopy (14). Perforation, hemorrhage, and AP are described as well one case of tumor cells dissemination after EUS-FNA for pancreatic tumor (6). O’Toole et al. (15) evaluated the complications of EUS-FNA in 322 patients. After 345 punctures they observed overall complication rate in 1.6%, without any case of serious complication or death.
In 3324 patients underwent radial EUS and EUS- FNA, 10 patients (0.3%) had complications related to the procedure and death in 0.06% of cases according Mortensen et al. (16). There was no statistical difference between diagnostic EUS and EUS-FNA (16).
The risk of iatrogenic AP caused by FNA ranges from 0 to 2% and increases in patients with pancreatic masses, cysts or when FNA is performed through MPD, because all these procedures consist of passing the needle directly through a normal pancreatic parenchyma (5,7- 9,11). Perhaps this was the major problem, in this case, because to reach its destination the needle had to cross a reasonable amount of normal pancreatic tissue and this was done twice.
O’Toole et al reported 4 complications (1.2%) after aspiration of pancreatic cystic tumors (3 cases of AP and 1 aspiration pneumonia). The AP in this series was the result of FNA in lesions of the head or uncinate process, unlike our case, with FNA performed in the body of the pancreas. Significantly in this study, the number of punctures was not important to predict the occurrence of complications (15). Eloubeidi et al. (9) reported 1 case (0.6%) of moderate intensity AP in 158 patients underwent EUS-FNA for solid tumors of the pancreas, and the other autor reported a fatal consequence of the EUS-FNA ina a patient with pancreatic cystic lesion (12).
Other studies suggest that episodes of AP after EUS- FNA occur more frequently in patients with a history of AP (7). Some relate its occurrence in patients with benign diseases or pseudotumors (17,18). The fact is that our patient had never had AP prior to EUS-FNA presented five episodes of AP after this procedure in 1 ½ year period, despite having a benign lesion.
In several reports of fatal AP episodes after percutaneous FNA of pancreas no cancer or mass was found during autopsy (17), which ratifies the one found in our case. Unlike, recent studies demonstrate a mass or pancreatic cancer in patients with AP after EUS-FNA (6,7-9,11).
Another factor that seems important and has been discussed in the literature deals with experience of the operator, because AP was found when about 79% of echo-endoscopists had performed at least 100 FNA for pancreatic masses (11). This is not the case, because the operator (JCA), at time of this procedure, had already performed more than 600 EUS-FNA for pancreatic tumors (3).
It is not possible to determine with certainty if smaller lesions are more likely to present episodes of AP. However a study with percutaneous FNA revealed the frequency of AP is higher in lesions smaller than 30 mm compared with those larger than 45 mm (17). In our case the lesion was much smaller than 30 mm, measuring 17 mm. So perhaps this was an important factor for the occurrence of AP. Our experience confirms these data. The frequency of AP after EUS-FNA appears to be lower than in cases submitted to percutaneous FNA (11). In a retrospective study with percutaneous FNA, severe episodes of AP occurred in 3% of patients (19). All patients who developed AP related to the procedure had lesions smaller than 30 mm (19).
It is mere speculation the mechanism by which episodes of AP occurs after FNA. Perhaps is related to pancreatic juice leakage from MPD or its branch ducts during FNA (11). Perhaps MPD or branch ducts disruption caused by needle, may be responsible for AP. Anyway, in this case and in all where the lesions are smaller than 30 mm, we always take care to avoid introduce the needle into MPD, a factor we consider important in genesis of AP episodes.
Gress et al. (7) prospectively evaluated the frequency of AP after pancreas EUS-FNA. In this study, the levels of blood amylase and lipase were measured before and 2 hours after procedure. There was significant elevation of amylase and / or lipase in 5%, but only 2% of patients showed clinical signs of AP. Interestingly the main reason for EUS-FNA be performed for these two developed AP, was unexplained recurrent AP episode (7).
In short, it is pointed out that pancreatic EUS-FNA is safe, effective and has a low AP occurrence rate in experienced hands. On the other hand, if a patient has a history of recurrent AP, normal pancreatic parenchyma between the wall of the digestive system and the lesion to be punctured, a benign lesion less than 30 mm or MPD transfixed by inadvertently puncture, are supposedly causal factors of AP, as no clear risk factor was identified. Surely the vast majority of retrospective studies demonstrating AP after EUS- FNA are underestimated.
Conflict of interest: The authors have no potential conflicts of interest
REFERENCES
1. Okasha HH, Ashry M, Imam HM, Ezzat R, Naguib M, Farag AH, et al. Role of endoscopic ultrasound-guided fine needle aspiration and ultrasound-guided fine-needle aspiration in diagnosis of cystic pancreatic lesions. Endosc Ultrasound. 2015;4(2):132-6. [ Links ]
2. Lee JG. Brush cytology and the diagnosis of pancreaticobiliary malignancy during ERCP. Gastrointest Endosc. 2006;63(1):78-80. [ Links ]
3. Ardengh JC, Lopes CV, de Lima LF, de Oliveira JR, Venco F, Santo GC, et al. Diagnosis of pancreatic tumors by endoscopic ultrasound-guided fine-needle aspiration. World J Gastroenterol. 2007;13(22):3112-6. [ Links ]
4. Wiersema MJ, Vilmann P, Giovannini M, Chang KJ, Wiersema LM. Endosonography-guided fine-needle aspiration biopsy: diagnostic accuracy and complication assessment. Gastroenterology. 1997;112(4):1087-95. [ Links ]
5. Eloubeidi MA, Tamhane A, Varadarajulu S, Wilcox CM. Frequency of major complications after EUS-guided FNA of solid pancreatic masses: a prospective evaluation. Gastrointest Endosc. 2006;63(4):622-9. [ Links ]
6. Paquin SC, Chua TS, Tessier G, Gariepy G, Raymond G, Bourdages R. A first report of tumor seeding by EUS-FNA. Gastrointest Endosc. 2004;59:AB 235. [ Links ]
7. Gress F, Michael H, Gelrud D, Patel P, Gottlieb K, Singh F, et al. EUS-guided fine-needle aspiration of the pancreas: evaluation of pancreatitis as a complication. Gastrointest Endosc. 2002;56(6):864-7. [ Links ]
8. Bournet B, Migueres I, Delacroix M, Vigouroux D, Bornet JL, Escourrou J, et al. Early morbidity of endoscopic ultrasound: 13 years’ experience at a referral center. Endoscopy. 2006;38(4):349-54.
9. Eloubeidi MA, Chen VK, Eltoum IA, Jhala D, Chhieng DC, Jhala N, et al. Endoscopic ultrasound-guided fine needle aspiration biopsy of patients with suspected pancreatic cancer: diagnostic accuracy and acute and 30-day complications. Am J Gastroenterol. 2003;98(12):2663-8. [ Links ]
10. Siddiqui AA, Shahid H, Shah A, Khurana T, Huntington W, Ghumman SS, et al. High risk of acute pancreatitis after endoscopic ultrasound-guided fine needle aspiration of side branch intraductal papillary mucinous neoplasms. Endosc Ultrasound. 2015;4(2):109-14. [ Links ]
11. Adler DG, Jacobson BC, Davila RE, Hirota WK, Leighton JA, Qureshi WA, et al. ASGE guideline: complications of EUS. Gastrointest Endosc. 2005;61(1):8-12. [ Links ]
12. Jonkman EF, van Tuyl BA, Sanders FB, Haas LE. Severe acute pancreatitis after EUS-FNA of a pancreatic cyst: a rare, but serious complication. BMJ Case Reports. 2015;2015. pii: bcr2015209442. [ Links ]
13. Zubarik R, Eisen G, Mastropietro C, Lopez J, Carroll J, Benjamin S, et al. Prospective analysis of complications 30 days after outpatient upper endoscopy. Am J Gastroenterol. 1999;94(6):1539-45. [ Links ]
14. Zubarik R, Fleischer DE, Mastropietro C, Lopez J, Carroll J, Benjamin S, et al. Prospective analysis of complications 30 days after outpatient colonoscopy. Gastrointest Endosc. 1999;50(3):322-8. [ Links ]
15. O’Toole D, Palazzo L, Arotcarena R, Dancour A, Aubert A, Hammel P, et al. Assessment of complications of EUS-guided fine-needle aspiration. Gastrointest Endosc. 2001;53(4):470-4.
16. Mortensen MB, Fristrup C, Holm FS, Pless T, Durup J, Ainsworth AP, et al. Prospective evaluation of patient tolerability, satisfaction with patient information, and complications in endoscopic ultrasonography. Endoscopy. 2005;37(2):146-53. [ Links ]
17. Levin DP, Bret PM. Percutaneous fine-needle aspiration biopsy of the pancreas resulting in death. Gastrointest Radiol. 1991;16(1):67-9. [ Links ]
18. Welch TJ, Sheedy PF, 2nd, Johnson CD, Johnson CM, Stephens DH. CT-guided biopsy: prospective analysis of 1,000 procedures. Radiology. 1989;171(2):493-6. [ Links ]
19. Mueller PR, Miketic LM, Simeone JF, Silverman SG, Saini S, Wittenberg J, et al. Severe acute pancreatitis after percutaneous biopsy of the pancreas. AJR Am J Roentgenol. 1988;151(3):493-4. [ Links ]
Correspondence:
José Celso Ardengh, PhD,
Alameda dos Arapanés, 881 - cj 111
Moema - CEP 04524-001. São Paulo, SP - Brazil Phone: 55 11 50557134
E-mail: jcelso@uol.com.br
Recibido: 25.05.18
Aprobado:15.04.19