Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista de Gastroenterología del Perú
Print version ISSN 1022-5129
Rev. gastroenterol. Perú vol.39 no.3 Lima July/Sep 2019
ARTÍCULOS ORIGINALES
Trends in mortality due to gastrointestinal diseases attributed to alcohol use in Peru from 2003 to 2016
Tendencias en mortalidad por enfermedades gastrointestinales debidas al uso de alcohol en el Perú del 2003 al 2016
Akram Hernández-Vásquez1, Rodrigo Vargas-Fernández2, Alexis Rebatta-Acuña3, Guido Bendezu-Quispe4
1 Universidad San Ignacio de Loyola, Vicerrectorado de Investigación, Centro de Excelencia en Investigaciones Económicas y Sociales en Salud. Lima, Peru.
2 Universidad Científica del Sur. Lima, Peru.
3 Universidad Nacional San Luis Gonzaga. Ica, Peru.
4 Universidad San Ignacio de Loyola, Vicerrectorado de Investigación, Unidad de Investigación para la Generación y Síntesis de Evidencias en Salud. Lima, Peru.
ABSTRACT
Objective: To assess and identify changes in the temporal trend in mortality from alcohol-attributable gastrointestinal diseases and their disease burden based on years of life lost (YLL) in Peru. Materials and methods: An ecological study of the death records of the Ministry of Health of Peru was conducted from 2003-2016. A gastrointestinal death attributable to alcohol was considered if the basic, intermediate, or final cause of death included ICD-10 codes: K70, K700-4, K709, K292, K852, and K860. Crude and age-adjusted mortality rates were calculated for the general population aged 15 or older and by sex, and YLL. Joinpoint regression analysis was performed to evaluate trends in mortality. Results: There were 11 148 deaths by alcohol-attributable gastrointestinal diseases, being more frequent in males (74.89%), in adults aged 45 years and above (83.67%), living in urban area (69.87%) and the Andes region (60.0%), and in subjects with liver disease (85.98%). Adjusted mortality rates varied from 6.21 (95% CI: 5.78- 6.63) in 2003 to 3.95 (95% CI: 3.67-4.22) in 2016. The trend of mortality decreased in the general population (APC: -6.17, 95% CI: -9.9 to -2.2, p=0.007) during the period 2008-2016. Deaths from the causes studied generated 224 545 YLL. Conclusions: A declining trend was found in gastrointestinal deaths attributable to alcohol in the period 2008-2016. The highest mortality occurred in males, individuals aged 45 years and above, living in urban areas and the Andes region.
Keywords: Alcohol-related disorders; Mortality; Liver cirrhosis (source: MeSH NLM).
RESUMEN
Objetivo: Evaluar e identificar los cambios en la tendencia temporal en mortalidad debida a las enfermedades gastrointestinal causadas por el alcohol y su carga de enfermedad basada en años de vida potencialmente perdidos (AVPP) en Perú. Material y métodos: Un estudio ecológico de los reportes de muerte del Ministerio de Salud del Perú entre 2013 a 2016. Se consideró una enfermedad gastrointestinal asociada al alcohol si la causa final o básica o intermedia de la muerta incluía los códigos CIE 10: K70, K700-4 K709 K292 K852 y K860. Los índices de mortalidad bruta y ajustada a la edad se calcularon para población general mayor de 15 años y por sexo y AVPP. Se realizaron análisis de regresión joinpoint para evaluar las tendencias en mortalidad. Resultados: Hubieron 11 148 muertes por enfermedades gastrointestinal atribuidas al uso de alcohol, siendo más frecuente en hombres (74,89%), en personas de 45 a más años de edad (83,67%), pobladores de área urbana (69,87%), en la región de los Andes (60,0%) y en sujetos con enfermedad hepática (85,98%). La tasa de mortalidad ajustada varió de 6,21 (95% IC 5,78 - 6,63) en 2003 a 3,95 (95% IC 3,67 - 4,22) en el 2016. La tendencia de la mortalidad disminuyó en la población general (APC: -6,17, 95% IC: -9,9 a -2,2, p=0,007) durante el periodo 2008-2016. Las muertes debidas a las causas estudiadas generaron 224 545 años perdidos. Conclusiones: Se encontró una tendencia decreciente en las muertes por enfermedades gastrointestinal atribuidas al alcohol en el periodo 2008-2016. La mortalidad más alta ocurrió en hombres, personas de 45 a más años, procedentes de áreas urbanas y de la región de los Andes.
Palabras clave: Trastornos relacionados con alcohol; Mortalidad; Cirrosis hepática (fuente: DeCS BIREME).
INTRODUCTION
Alcohol consumption is one of the main risk factors for reduced public health due to the significant burden of disease it produces, and it is related to around 60 acute and chronic diseases (1,2). The direct and indirect harmful effects of alcohol on health are produced by three inter-related mechanisms: organ and tissue damage, dependence, and intoxication (3). Likewise, the potential damage attributable to alcohol is related to the volume, frequency, and quality of alcohol consumed (2,3).
The need to control alcohol consumption was established in 2015 as part of the 17 Sustainable Development Goals (SDGs) defined by the United Nations (UN) General Assembly (4). Compliance with this objective is relevant, considering that despite the decrease in alcohol-attributable mortality worldwide (from 44.6 in 2010 to 38.8 in 2016 per 100 000 inhabitants) (4), the burden of disease by this substance is still high (4). For the region of the Americas, 5.5% of deaths and 6.7% of disability-adjusted life years (DALYs) were attributable to alcohol consumption in 2016 (4). In this region, alcohol consumption is frequent, with a lifetime prevalence higher than 50% (4).
Alcohol is a risk factor for the development of gastrointestinal diseases that can lead to death, especially hepatic cirrhosis and pancreatitis (4). For example, around 230 International Statistical Classification of Diseases and Related Health Problems- tenth edition (ICD-10) codes are related to alcohol, with digestive diseases being those with high alcohol- attributable mortality (4). Of the total deaths attributable to alcohol worldwide in 2016, 21.3% were due to gastrointestinal diseases that originated 23.3 million DALYs due to alcohol intake (2,4).
It has been described that the leading causes of death from gastrointestinal diseases in Peru are hepatic cirrhosis, malignant tumors of the stomach and metastases to the liver and gallbladder, pancreas and colon (5.6). While alcohol consumption is related to these diseases, especially to hepatic cirrhosis as a specific cause for its development (7), there are no data on mortality or trends in disease burden for gastrointestinal diseases attributable to alcohol. Therefore, the objective of this study was to evaluate and identify the presence of temporary changes in mortality from gastrointestinal diseases, and the burden of alcohol-attributable disease measured in years of life lost (YLL) in Peru in the period from 2003 to 2016.
MATERIALS AND METHODS
An ecological study of the mortality by gastrointestinal disease attributable to alcohol in Peru during the period 2003-2016 was carried out using the database of deaths of the Ministry of Health of Peru (MINSA). This database was provided by MINSA after requesting it through its official online form (https://www.minsa. gob.pe/portada/transparencia/solicitud/). It includes the reporting of death certificates at the national level containing the basic, intermediate and final cause of death using ICD-10 codes. The number of inhabitants for each year of study was obtained from the National Institute of Statistics and Informatics of Peru (http:// proyectos.inei.gob.pe/web/poblacion/)
The presence of the ICD-10 codes in the records of deaths served to generate the variable of interest for the analysis: death by gastrointestinal disease attributable to alcohol. Additionally, the data on sex, age at the time of death, the area of residence (urban/rural), and geographic domain (Coast/Andes/Amazon forest) of residence of the deceased.
For the study, the following ICD-10 death diagnoses were included: for hepatic causes, K70 codes (alcoholic liver disease), K70.0 (fatty alcoholic liver), K70.1 (alcoholic hepatitis), K70.2 (fibrosis and sclerosis of the liver), K70.3 (alcoholic hepatic cirrhosis), K70.4 (alcoholic liver failure), and K70.9 (alcoholic liver disease, not specified); for gastric causes, the K29.2 code (alcoholic gastritis) was included, and for pancreatic causes, codes K85.2 (alcohol-induced acute pancreatitis) and K86.0 (alcohol-induced chronic pancreatitis) were included.
Crude mortality rates were calculated for each year of study as well as the specific rates of death according to sex, by age groups (15-19, 20-24, 25-29, 30-34, 35-39, 40-44, 45-49, 50-54, 55-59, 60-64, 65-69, 70-74, 75-79, and 80 plus). In addition, age-adjusted rates were calculated for the Peruvian population older than 15 years, using the direct method utilizing the population standard of the World Health Organization (8). All rates were reported for every 100 000 inhabitants. No corrections were made for death sub-registry. The characterization of the condition of the area of urban and rural residence was carried out by the Supreme Decree N° 090-2011-PCM that contains the list of district municipalities in rural Peru, and the geographic domain was categorized using the classification of the Peruvian Institute of Data (http://usmp.edu.pe/idp/ distritos-datos/).
The YLL by gastrointestinal deaths related to alcohol consumption were calculated considering 80 years as the value of life expectancy for both sexes using the male life expectancy at birth of model 26 of the modified Princeton West life tables as the reference value (9). The total YLL were reported at the national level for all the years included in the study.
A joinpoint regression model was used for the identification of periods with significant changes in the mortality rate, that is, the years in which a significant change occurred in the linear slope of the temporal trend. The joinpoint regression analysis was carried out using the Joinpoint Trend Analysis Software v 4.6.0.0 (Surveillance Research Program of the US National Cancer Institute) in order to identify possible changes with significant differences in the trends in deaths from gastrointestinal diseases related to alcohol consumption. The method applied identified union points according to the model with up to three points of change. The final model selected was the most adjusted method, with an annual percentage change (APC) based on the trend of each segment. All analyses were performed considering a p-value < 0,05 as significant.
Ethics statement
This study did not require approval from an institutional ethics committee because it was an ecological study that uses grouped secondary data that does not have identifiers of individual subjects.
RESULTS
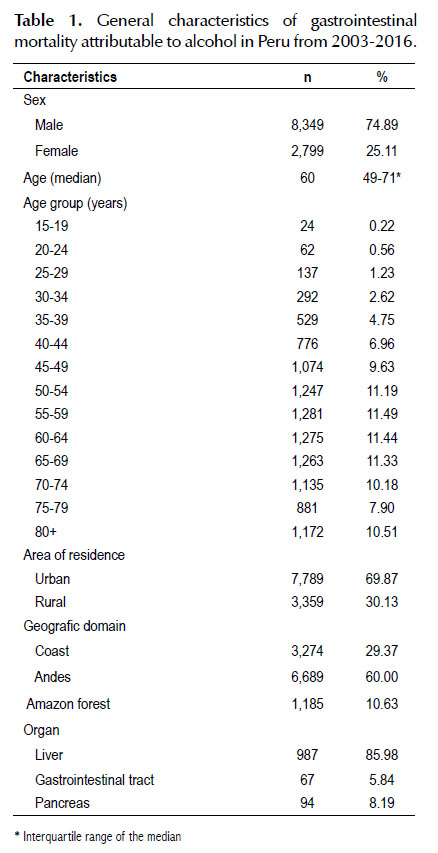
Between 2003 and 2016, a total of 11 148 deaths attributables to gastrointestinal diseases related to alcohol consumption were recorded, 8 349 (74.89%) of which occurred in males. Men had a mean age of 58.77 ± 14.93 and women 63.54 ± 15.32 years. The median age of the deceased was 60 (Interquartile Range (IQR): 49-71). The highest number of deaths was presented in individuals aged 45 years and above (83.67%), with the highest gastrointestinal mortality attributable to alcohol being found in the age groups of 55-59, 60-64 and 65-69 years, with 1 281, 1 275 and 1 263 deaths, respectively.
Concerning the area of residence, 7 789 (69.87%) lived in an urban area. Regarding the geographic domain, the majority of deaths occurred in the Andes region with 6 689 cases, followed by the Coast region with 3 274 (29.31%) and the Amazon forest region with 1 185 deaths (10.63%) (Table 1).
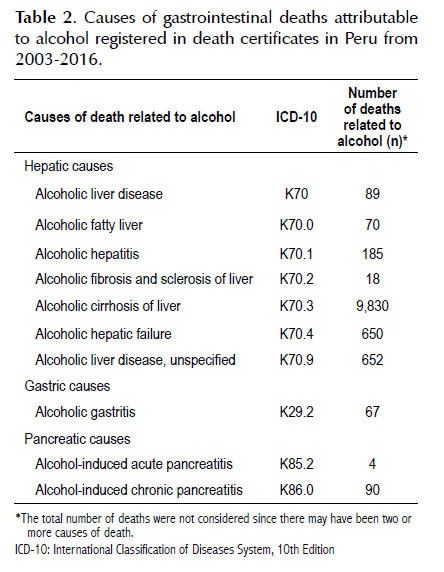
Concerning the organ involved in gastrointestinal death attributable to alcohol, the liver was the organ most frequently involved with 987 deaths (85.98%), followed by the pancreas with 94 (8.19%) and gastrointestinal tract with 67 deaths (5.84%) (Table 1). Of the ICD-10 codes related to death attributable to alcohol consumption in Peru, the K70.3 code (alcoholic liver cirrhosis ) was the most frequently reported with 9 830 deaths, followed by codes K70.9 (alcoholic liver disease, unspecified) and K70.4 (alcoholic liver failure) with 650 and 652 deaths, respectively (Table 2).
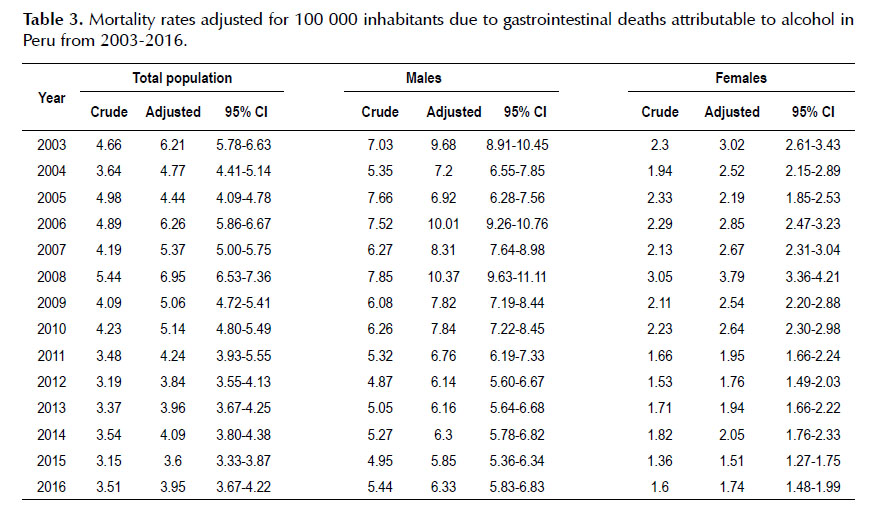
The adjusted mortality rates ranged from 6.21 (95% confidence interval [CI]: 5.78-6.63) in 2003 to 3.95 (95% CI: 3.67-4.22) in 2016 for the total population (Table 3). In terms of sex, males presented the highest adjusted mortality rates varying from 9.68 (95% CI: 8.91- 10.45) in 2003 to 6.33 (95% CI: 5.83-6.83) in 2016.
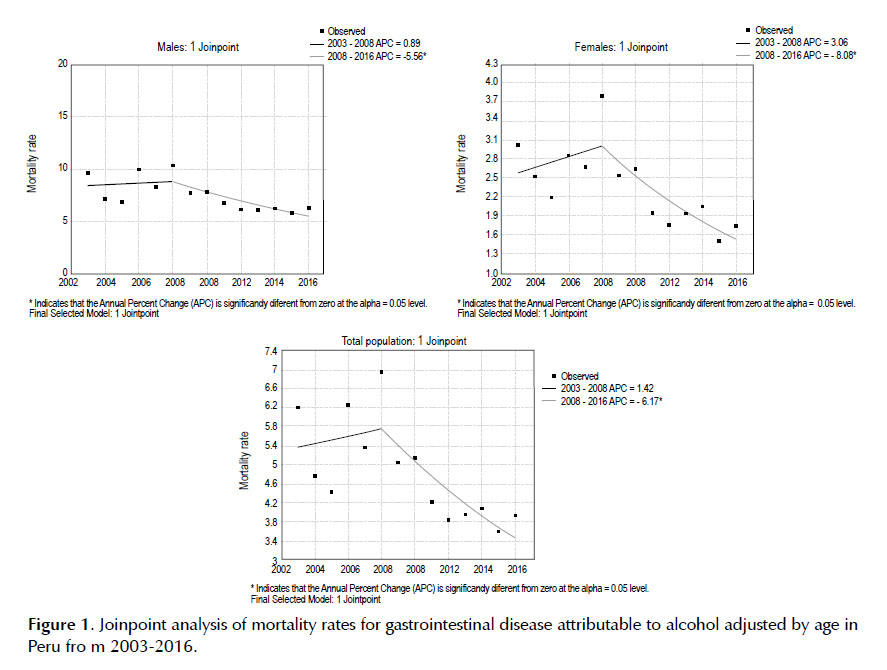
For the total population, the joinpoint regression analysis found an initial period of increase in mortality between the years 2003 and 2008, although this was not significant (APC: 1.42, 95% CI: -6.7 to 10.2, p=0.710).
On the other hand, a significant decrease in mortality was observed between 2008 and 2016 (APC: -6.17, 95% CI: -9.9 to-2.2, p=0.007) (Figure 1). In the period 2003-2008, males showed a non-significant rise in mortality (APC: 0.89, 95% CI: -7.4 to 9.9, p=0.820), while from 2008 to 2016 a significant decrease in mortality was presented (APC =-5.56, 95% CI: -9.5 to-1.5, p=0.013) (Figure 1). A non-significant increase in mortality was shown in women between 2003 and 2008 (APC: 3.06, 95% CI: -5.5 to 12.4, p=0.451), and there was a significant decrease in mortality for the period 2008-2016 (APC:-8.08, 95% CI: -12.0 A-4.0, p=0.002) (Figure 1).
Regarding YLL, deaths from alcohol-related gastrointestinal diseases generated a total of 224 545 YLL during the period 2003-2016, ranging from 12 543 (2005) to 20 435 (2008).
DISCUSSION
The results of this study show, a decrease in gastrointestinal mortality attributable to alcohol for the total population during the study period (2003- 2016), with a significant declining trend in mortality in both sexes from 2008 to 2016. The majority of gastrointestinal deaths attributable to alcohol consumption were related to liver diseases, with higher mortality in men, individuals living in urban areas, and in the Andes region.
Mortality from gastrointestinal disease attributable to alcohol showed a decrease in the rate adjusted for age between 2003 and 2016, and there was a significant trend towards a decrease in mortality from 2008 to 2016, in both the whole population and in both sexes. This finding is similar to the global trend of alcohol-attributable mortality, with a decrease from 44.6 (2010) to 38.8 (2016) in deaths per 100 000 inhabitants (4). Despite this, the impact of alcohol- attributable mortality remains high, being even higher than that reported for diseases such as tuberculosis, HIV/AIDS and diabetes (4). It is, therefore, necessary to develop public health policies and interventions to reduce mortality due to alcohol consumption, bearing in mind that all these deaths are preventable.
We found deaths attributable to alcohol to be more common in males similar to the pattern of greater chronic alcohol consumption reported in men worldwide (4,10,11) and in countries such as Peru (4,12,13) as well as other Latin American countries such as Brazil, Chile and Mexico (14-16). In recent years, there has been an increase in the consumption of alcohol in the female population, related to changes in cultural conceptions. However, the consumption of this group is lower compared to their male peers (10,11,17). In the Peruvian population, starting in adolescence, males have a higher consumption of alcohol than females (17), being a pattern historically supported by a greater acceptance of the consumption of this substance in males, leading to a higher burden of disease by this risk factor (10,11,17).
Age groups over 45 years old presented the highest adjusted mortality rates due to gastrointestinal diseases related to alcohol. People over 45 years of age had the highest mortality attributable to chronic alcohol consumption, with the main causes of mortality being due to non-communicable diseases such as cardiovascular diseases and cancers (including various primary cancers of the gastrointestinal tract) (4,16). Although the largest number of alcohol-related deaths occurred in individuals over 45 years of age, alcohol- related gastrointestinal deaths were also reported in people less than or equal to 18 years of age. In Peru, the legal age for the purchase and consumption of alcohol consumption is 18 years (4). In 2015, the age of onset of alcohol consumption in Peru was 12.6 years, with a higher prevalence of alcohol consumption in children in urban areas. (17) In Peru, the family environment is the main risk factor for the onset of alcohol intake (17). Taking into account the initiation of alcohol consumption at an age earlier than legally permitted, morbidity and mortality associated with chronic alcohol consumption can be expected, including death by gastrointestinal diseases, as shown by the data analyzed.
Most of the deaths occurred in the geographic domain of the Andes region. A higher prevalence of alcoholism has been previously described in populations living in extreme poverty in Peru (18), which could explain this finding. The Andes region presents the districts with the highest prevalences of poverty and extreme poverty in the country, accompanied by less access to health services (19). On the other hand, most deaths occurred in residents of urban areas. This result can likely be explained by the higher prevalence of male consumers who reside in the urban sector, with a pattern of alcohol intake since adolescence and greater access to alcoholic beverages, in addition to greater psychological and social pressure compared to rural areas (17,20).
The highest mortality attributable to alcohol according to the organ involved was related to the liver. Previous studies in the Peruvian population reported liver cirrhosis as the main cause of the burden of disease by gastrointestinal diseases attributable to alcohol (5,21,22). Hepatic cirrhosis is the leading cause of alcohol-attributable gastrointestinal disease worldwide (4,15), constituting an important public health problem due to the high morbidity and mortality (14,23), together with the development of various cancers and injuries, which are the main causes of the burden of disease produced by alcohol worldwide (4,23).
With regard to YLL due to alcohol-attributable burden of disease by gastrointestinal disease in the Peruvian population from 2003 to 2016, the greatest mortality was related to liver diseases. Alcohol consumption was the seventh major risk factor for death as well as for DALYs in 2016, with more than one-quarter of cancer deaths reported worldwide in the population greater than or equal to 50 years of age (4). In addition, alcohol consumption generated 132.6 million DALYs (5.1% of all DALYs in 2016), of which 107.7 million DALYs were due to premature death (YLL, representing 5.8% of all YLL in 2016) (4). In 2012 in Peru, alcohol produced a mortality rate by hepatic cirrhosis of 24.3 deaths/100 000 people, representing a total of 13.9 DALYs and 1.4 deaths per 100 000 inhabitants in Peru, as well as an additional 0.9 DALYs due to other digestive diseases. In 2015, alcohol and drug use accounted for 9.0% of the lost healthy life years (19). Thus, gastrointestinal deaths from alcohol consumption contribute to the disease burden generated by this substance in the Peruvian population.
Control of alcohol consumption is closely related to SDGs. Peru is committed to achieving the proposed SDG goals by 2030, including a reduction in alcohol consumption (24). In this respect, in 2016, the consumption of pure alcohol per capita in Peru by individuals over 15 years of age was 6.3 liters. Although this value is somewhat lower than the average reported by the WHO for the region of the Americas (8 liters) (4), strategies aimed at reducing alcohol consumption must be developed. Peru has implemented measures to discourage alcohol consumption, including a tax on the purchase and consumption of alcoholic beverages, and has placed restrictions on the purchase of alcoholic beverages at some specific events (4). In addition, the National Drug Control Strategy 2017-2021 seeks to promote healthy lifestyles, strengthen regulatory policies on alcohol consumption, and develop preventive programs for specific populations (25).
This study presents some limitations related to the use of secondary bases, which cannot guarantee the accuracy of the data, including problems related to the quality of the recording of death certificates, specifically in terms of registration of the ICD-10 codes and under- registration of deaths. The contribution of alcohol- related death by chronic liver disease is conventionally determined by the use of ICD-10 codes for death from alcoholic liver disease in death certificates (26,27). This method of evaluating mortality carries a risk of under- registration of diseases, with alcohol intake being potentially attributed as a causality of death. Indeed, one study showed that death attributable to alcohol intake was underreported by up to six-fold when death certificates were the only reporting system assessed, and no additional medical or legal records were used (28). Taking into account that alcohol increases the risk of 230 ICD-10 codes (29,30), we believe that our study provides an overview of the problem at a national level due to the use of a mortality database generated by the Ministry of Health of Peru that consolidates the registration of the causes of death reported in death certificates at both the local and national level.
We conclude that there has been a reduction in the trend of mortality of gastrointestinal origin attributable to alcohol between the years 2008 and 2016 in Peru. The highest mortality was found in males, people from the Andes region, and adults aged 45 years or above, although deaths in minors were also reported. Alcohol consumption is a preventable factor in gastrointestinal mortality, reaffirming the need for programs aimed at identifying and studying alcohol-related factors from early ages (school programs) to decrease the consumption of this substance and thereby reduce the burden of attributable and preventable disease caused by excessive alcohol consumption.
Conflict of interest: The authors have nothing to declare.
Citar como: Hernández-Vásquez A, Vargas-Fernández R, Rebatta-Acuña A, Bendezu-Quispe G. Trends in mortality due to gastrointestinal diseases attributed to alcohol use in Peru from 2003 to 2016. Rev Gastroenterol Peru. 2019;39(3):239-45
REFERENCES
1. Ezzati M, Vander Hoorn S, Lopez AD, Danaei G, Rodgers A, Mathers CD, et al. Comparative Quantification of Mortality and Burden of Disease Attributable to Selected Risk Factors. In: Lopez AD, Mathers CD, Ezzati M, Jamison DT, Murray CJL, editors. Global Burden of Disease and Risk Factors [Internet]. Washington (DC): The International Bank for Reconstruction and Development / The World Bank; 2006 [accessed February 10, 2019]. Available from: https://www. ncbi.nlm.nih.gov/books/NBK11813/ [ Links ]
2. Rehm J, Room R, Graham K, Monteiro M, Gmel G, Sempos CT. The relationship of average volume of alcohol consumption and patterns of drinking to burden of disease: an overview. Addiction. 2003;98(9):1209-28. [ Links ]
3. World Health Organization. Alcohol [Internet]. Geneva: WHO; 2019 [accessed February 25, 2019]. Available from: https://www.who.int/substance_abuse/facts/alcohol/en/ [ Links ]
4. World Health Organization. Global status report on alcohol and health 2018 [Internet]. Geneva: WHO; 2018 [accessed February 20, 2019]. Available from: https://apps.who.int/iris/ bitstream/handle/10665/274603/9789241565639-eng.pdf [ Links ]
5. Farfán G, Cabezas C. Mortalidad por enfermedades digestivas y hepatobiliares en el Perú, 1995-2000. Rev Gastroenterol Peru. 2002;22(4):310-23. [ Links ]
6. Hernández-Vásquez A, Bendezú-Quispe G, Azañedo D, Huarez B, Rodríguez-Lema B. Temporal trends and regional variations in gastrointestinal cancermortality in Peru, 2005- 2014. Rev Gastroenterol Peru. 2016;36(4):320-9. [ Links ]
7. Musayón-Oblitas Y, Meléndez-De la Cruz R. Muerte prematura por consumo de alcohol: estudio en base a datos de mortalidad del Perú. Rev Enferm Herediana. 2016;9(2):79-89. [ Links ]
8. Ahmad OB, Boschi-Pinto C, Lopez AD, Murray CJ, Lozano R, Inoue M. Age standardization of rates: a new WHO standard. Geneva: World Health Organization; 2001. [ Links ]
9. Coale A, Guo G. Revised regional model life tables at very low levels of mortality. Popul Index. 1989;55(4):613-43. [ Links ]
10. Tedor MF, Quinn LM, Wilsnack SC, Wilsnack RW, Greenfield TK. The gender difference in the association between early onset of drinking and problem drinking between the US and Japan. Deviant Behav. 2018;39(12):1578-99. [ Links ]
11. Wilsnack RW, Wilsnack SC, Kristjanson AF, Vogeltanz Holm ND, Gmel G. Gender and alcohol consumption: patterns from the multinational GENACIS project. Addiction. 2009;104(9):1487-500. [ Links ]
12. World Health Organization, Pan American Health Organization. Regional Status Report on Alcohol and Health in the Americas 2015 [Internet]. Geneva: WHO; 2015 [accessed February 20, 2019]. Available from: https://www. paho.org/hq/dmdocuments/2015/Alcohol-Report-Health- Americas-2015.pdf [ Links ]
13. Yamamoto J, Silva JA, Sasao T, Wang C, Nguyen L. Alcoholism in Peru. Am J Psychiatry. 1993;150(7):1059-62. [ Links ]
14. Pérez-Pérez E, Cruz-López L, Hernández-Llanes NF, Gallegos- Cari A, Camacho-Solís RE, Mendoza-Meléndez MÁ. Años de Vida Perdidos (AVP) atribuibles al consumo de alcohol en la ciudad de México. Cien Saude Coletiva. 2016;21(1):37-44. [ Links ]
15. Castillo-Carniglia Á, Kaufman JS, Pino P. Alcohol-attributable mortality and years of potential life lost in Chile in 2009. Alcohol Alcohol. 2013;48(6):729-36. [ Links ]
16. Melo APS, França EB, Malta DC, Garcia LP, Mooney M, Naghavi M. Mortality due to cirrhosis, liver cancer, and disorders attributed to alcohol use: Global Burden of Disease in Brazil, 1990 and 2015. Rev Bras Epidemiol. 2017;20:61-74. [ Links ]
17. Ministerio de Salud del Perú. Documento Técnico: Situación de Salud de los Adolescentes y Jóvenes en el Perú. 2017 [Internet]. Lima: MINSA; 2017 [accessed March 3, 2019]. Available from: http://bvs.minsa.gob.pe/ local/MINSA/4143.pdf [ Links ]
18. Quiñones-Laveriano DM, Espinoza-Chiong C, Scarsi-Mejia O, Rojas-Camayo J, Mejia CR. Altitud geográfica de residencia y dependencia alcohólica en pobladores peruanos. Rev Colomb Psiquiatr. 2016;45(3):178-85. [ Links ]
19. Lazo-Gonzales O, Alcalde-Rabanal J, Espinosa-Henao O. El sistema de salud en Perú: situación y desafíos [Internet]. Lima: Colegio Médico del Perú; 2016 [accessed February 18, 2019]. Available from: http://web2016.cmp.org.pe/wp- content/uploads/2016/12/libroSistemaSaludPeru-.pdf [ Links ]
20. Instituto Nacional de Estadística e Informática. Encuesta Demográfica y de Salud Familiar 2016 [Internet]. Lima: INEI; 2017 [accessed March 1, 2019]. Available from: https://www. inei.gob.pe/media/MenuRecursivo/publicaciones_digitales/ Est/Lib1433/index.html. [ Links ]
21. Bustíos C, Dávalos M, Román R, Zumaeta E. Características epidemiológicas y clínicas de la cirrosis hepática en la Unidad de Hígado del HNERM Es-Salud. Rev Gastroenterol Peru. 2007;27(3):238-45. [ Links ]
22. Malpica-Castillo A, Ticse R, Salazar-Quiñones M, Cheng- Zárate L, Valenzuela-Granados V, Huerta-Mercado Tenorio J. Mortalidad y readmisión en pacientes cirróticos hospitalizados en un hospital general de Lima, Perú. Rev Gastroenterol Peru. 2013;33(4):301-5. [ Links ]
23. Rehm J, Shield KD. Global alcohol-attributable deaths from cancer, liver cirrhosis, and injury in 2010. Alcohol Res. 2013;35(2):174-83. [ Links ]
24. Programa de las Naciones Unidas para el Desarrollo (PNUD). Objetivos de Desarrollo Sostenible [Internet]. Lima; PNUD Peru; 2019 [accessed March 4, 2019]. Available from: http://www.pe.undp.org/content/peru/es/home/sustainable-development-goals.html. [ Links ]
25. DEVIDA. Estrategia Nacional de Lucha Contra las Drogas 2017-2021 [Internet]. Lima; DEVIDA. 2017 [accessed February 28, 2019]. Available from: http://www.devida.gob.pe/ documents/20182/314196/Estrategia_FINAL_castellano2.pdf. [ Links ]
26. Manos MM, Leyden WA, Murphy RC, Terrault NA, Bell BP. Limitations of conventionally derived chronic liver disease mortality rates: Results of a comprehensive assessment. Hepatology. 2008;47(4):1150-7. [ Links ]
27. Vong S, Bell BP. Chronic liver disease mortality in the United States, 1990–1998. Hepatology. 2004;39(2):476-83. [ Links ]
28. Pollock DA, Boyle CA, DeStefano F, Moyer LA, Kirk ML. Underreporting of alcohol-related mortality on death certificates of young US Army veterans. JAMA. 1987;258(3):345-8. [ Links ]
29. Rehm J, Gmel Sr GE, Gmel G, Hasan OS, Imtiaz S, Popova S, et al. The relationship between different dimensions of alcohol use and the burden of disease—an update. Addiction. 2017;112(6):968-1001. [ Links ]
30. World Health Organization. International classification of diseases and related health problems, 10th revision [Internet]. Geneva; WHO; 2010 [accessed February 20, 2019]. Available from: http://www.who.int/classifications/apps/icd/icd10online [ Links ]
Correspondence:
Akram Abdul Hernández Vásquez
Universidad San Ignacio de Loyola, 550 La Fontana Avenue, La Molina, Lima, Peru.
E-mail: ahernandez@usil.edu.pe