Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista Peruana de Medicina Experimental y Salud Publica
versión impresa ISSN 1726-4634
Rev. perú. med. exp. salud publica vol.37 no.1 Lima ene./mar 2020
http://dx.doi.org/10.17843/rpmesp.2020.371.4460
Brief Report
Sensitization to aeroallergens in a peruvian pediatric population with allergic diseases
1 Centro de Referencia Nacional de Alergia, Asma e Inmunología, Instituto Nacional de Salud del Niño, Lima, Perú.
2 Facultad de Medicina, Universidad Nacional Mayor de San Marcos, Lima, Perú.
INTRODUCTION
Asthma and allergic rhinitis (AR) are the most important chronic inflammatory diseases in children, with a significant effect on the finances and life quality of these patients 1-3. The prevalence of these diseases is increasing worldwide, possibly due to factors, such as environment, diet or climate change (1. Based on different studies conducted in Peru, asthma and AR have a prevalence greater than 30% 4,5, and they constitute the most frequent chronic non-infectious diseases in patients of pediatric age.
Extra- or intradomiciliary aeroallergens are the main triggers of allergic diseases 1. During the first two years, children are exposed to intradomiciliary aeroallergens (dust mites, fungi, particles or animal excretions), and since the age of five they are exposed to extradomiciliary aeroallergens (pollen, fungi, grass) 1-3,6. Early exposure and the presence of atopy in patients with asthma or AR contribute to the persistence of these enzymes in adulthood 1-3. Sensitizing aeroallergens can vary between countries; however, their identification is necessary for a better clinical approach 1-3.
Atopy is the personal or familiar tendency to produce specific immunoglobulin E (IgE) antibodies in response to allergen sensitization (7. Its diagnosis is established by a compatible clinical history and is supported by skin testing (prick test) or in vitro tests that confirm sensitization or the presence of IgE against certain allergens 1-3. Skin testing is the most common test used to detect IgE-mediated reactions in patients with asthma and AR 1-3, because it has shown greater sensitivity and specificity 8 and has a lower rate of patient complications and discomfort 1-3.
KEY MESSAGES
Motivation for the study: To determine the sensitization profile of pediatric patients with asthma or allergic rhinitis using a skin test, a fundamental step for an adequate and specific management of allergic diseases.
Main findings: Most patients with asthma or allergic rhinitis present Dermatophagoides farinae sensitivity. It is associated with age, age groups and IgE level.
Implications: Our results should be considered complementary to the treatment of patients with asthma or allergic rhinitis with specific immunotherapy based on their sensitization.
Because of this, the identification of aeroallergens-sensitivity in patients with asthma or AR is useful to implement preventive measures and to develope more effective and targeted treatment strategies, such as allergen-specific immunotherapy, the only type of therapy capable of modifying the abnormal immune response in patients with allergic diseases, providing improvement in the symptomatology and quality of life 1-3.
The aim of this study is to establish the profile of aeroallergen sensitization in Peruvian children with diagnosis of asthma or AR due to the epidemiological significance and the need for specific interventions in these patients.
THE STUDY
Cross-sectional design. Patients were enrolled from January 2013 to December 2015 at the National Reference Center for Allergy, Asthma and Clinical Immunology (CERNAAI) of the National Institute of Children’s Health (INSN), a center specialized in allergic and immunological diseases that receives patients from all over Peru.
The study population was of 411 patients who were selected through a census sampling. We included patients from 2 to 17 years old, with clinical diagnosis of asthma or AR, based on the GINA and ARIA criteria, respectively 2,3. We excluded patients who had used antihistamines or systemic corticosteroids, at least seven days before skin testing; topical corticosteroids in the test area, at least 10 days before; patients in immunotherapy, at least six months before; in immunoregulatory therapy (use of intravenous immunoglobulin); with other immunological diseases (autoimmune or lymphoproliferative diseases); with dermography and with hyper or hyporreactive skin.
Data collected: age (categorized in groups: 2-5, 6-11 and 12-18 years old), gender, total IgE levels (IU/mL) and number of eosinophils in the hemogram (cells/mm3). All patients were skin tested using the Prick-Film® method to determine their specific allergens sensitivity. Results were obtained in mm2 (papule area) and in mm (welt diameter). The method used standard recommendations to indicate a positive result 9.
Sensitization was considered as a positive skin test result with one aeroallergen and in the poly-sensitization with two or more aeroallergens. The sensitization profile was classified by aeroallergen groups: dust mites, insects, fungi and animal epithelium. Fourteen aeroallergens were applied (7 dust mites, 2 cockroaches, 3 fungi and dog and cat epithelium).
The data were analyzed with the SPSS program for Windows 20.0. Percentages and frequencies were used for the description of qualitative variables, and mean and standard deviation for quantitative variables. The distribution of quantitative variables was analyzed using histograms, box plots and the Kolmogorov-Smirnov test. The chi-square test was used to evaluate the association between sensitization and age groups and gender. The Student T-test was used for comparing means of the independent samples. Both tests used a 95% confidence level.
Prior to any procedure, parents or legal guardians voluntarily signed an informed consent form. Patients over the age of seven were asked to sign an assent form. The study protocol and the consent and assent forms were approved by the INSN Institutional Research Ethics Committee and were in accordance with the principles of the Helsinki Declaration (Project CL26-12).
RESULTS
The average age of the population was 8.1 ± 3.8 years old. 60.6% were male, 83.5% had asthma, 91.7% had rhinitis and 75.7% had AR. Among the patients with asthma, 69.8% (287/343) had a positive skin test, and 83.7% (311/377) of patients with AR had also a positive skin test. There is an increased frequency of allergic phenotype (positive test) in patients with asthma and AR (Figure 1).
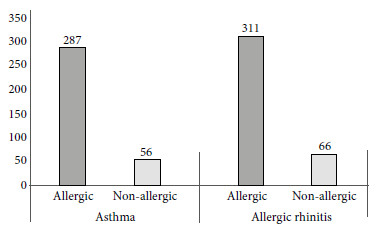
Figure 1 Allergic phenotype in 411 Peruvian pediatric patients with asthma and allergic rhinitis from the National Reference Center for Allergy, Asthma and Immunology, Lima.
The mean for eosinophils was 450.1 ± 377.3 cells/mm3 and the total mean for IgE was 861.7 ± 757.6 IU/mL. As for the age groups, 32.4% were between 2 and 5 years old, 47.9% between 6 and 11 years old and 19.7% between 12 and 18 years old (Table 1).
Table 1 Characteristics of 411 Peruvian pediatric patients with asthma or allergic rhinitis from the National Reference Center for Allergy, Asthma and Immunology, Lima.
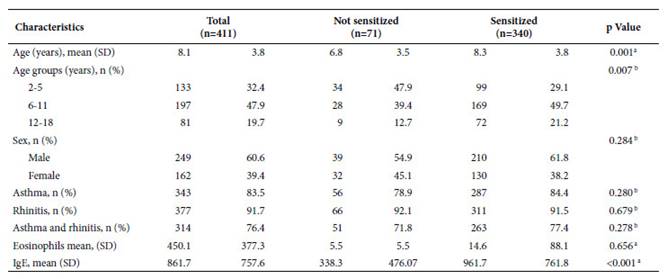
a Student T-test; b Chi-square test
SD: Standard Deviation
Sensitization profile
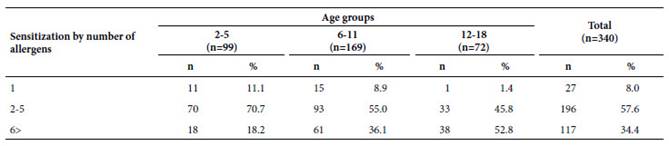
Sensitization was present in 82.7% of the patients. Sensitization was associated with age, age groups and total IgE levels (Table 1). The frequency of sensitization increased with age (Table 2). The most frequent sensitizing agents were mites (79.8%), followed by insects (42.3%) (Table 2). Only 6.6% of the patients were sensitized by a single aeroallergen, while 47.7% of the patients were sensitized by two to five aeroallergens, and 28.5% by six or more aeroallergens (Table 3).
Table 2 Sensitization profile in 411 Peruvian pediatric patients with asthma or allergic rhinitis from the National Reference Center for Allergy, Asthma and Immunology. Lima.
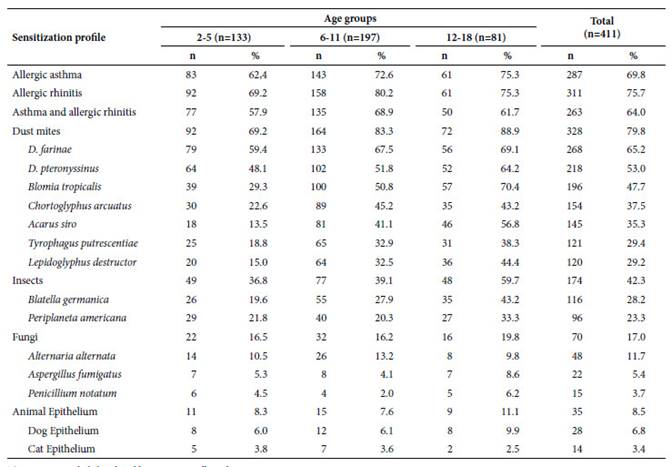
The categories included in the table are not mutually exclusive.
Table 3 Sensitization by number of allergens in 340 Peruvian pediatric patients with asthma or allergic rhinitis from the National Reference Center for Allergy, Asthma and Immunology. Lima.
Dermatophagoides farin (DF) (65.2%), Dermatophagoides pteronyssinus (DP) (53%) and Blomia tropicalis (47.7%) were the most frequent dust mites, 127 patients (30.9%) had a positive skin test for all three dust mites. Sensitization to insects was mainly due to Blatella germanica (28.2%) and Periplaneta americana (23.4%), while sensitization to fungi was found in 17% of patients, Alternaria alternata being the most frequent agent. Finally, sensitization to animal epithelia was found in 8.5% of patients. Cat epithelium and dog epithelium were found in 6.8% and 3.4%, respectively (Table 3).
DISCUSSION
Our study presents for the first time a sensitization profile using a skin test in a Peruvian pediatric population with a diagnosis of asthma or AR. It was shown that 82.7% of patients were sensitized by some aeroallergen (76.2% to more than one) and was associated with age, age groups and total IgE levels. Mites were the most frequent sensitizing agents, DF being the most common (65.2%). The skin test was chosen for its higher sensitivity and specificity (>85%) 7 and a lower rate of complications and patient discomfort 1-3. The skin test is recommended in clinical practice guidelines for asthma and AR (GINA and ARIA, Respectively) 2,3.
In Peru, some evaluations on sensitization profile have been carried out. The study called PURA (Peru Urban versus Rural Asthma) whose objective was to evaluate the prevalence of asthma and its associated risk factors using the skin test in 13-15-year-old adolescents from two cities (one urban and one rural) 10. The prevalence of asthma and the sensitization was 12% and 3%, and 56% and 38% in Lima and Tumbes, respectively. Further analysis found that 61% of subjects with AR were sensitized 11. Sensitization was lower compared to our study and could be due to the lower number of patients with a diagnosis of asthma and AR. In Lima 84 patients had diagnosis of asthma, and 166 had diagnosis of AR. On the other hand, in Tumbes 22 patients had diagnosis of asthma and 95 had diagnosis of AR.
On the other hand, a case-control study conducted in two communities in Lima included children between the ages of 9 and 19. From 412 asthmatic patients, 315 (78.2%) were atopic 12. These results are similar to ours; however, it should be noted that the evaluation of atopy was performed using ImmunoCap 250 (specific IgE serum detection) for three allergens (animal, mold and dust mites) where a specific IgE level > 0.1 kU/L is a positive result. This level may explain the high frequency of atopy, since a cut-off point of > 0.35 kU/L is commonly used in other studies.
Different results exist in other contexts. The National Health and Nutrition Examination Survey (NHANES) III, conducted in the United States between 1988 and 1994, found a frequency of sensitization using a skin test in 54.3% of the 6-59-year-old study subjects (multiethnic population). 13. On the other hand, a study in Morocco involving 379 patients found that 3.2% of asthmatic patients were mono- and polysensitized, while 18.2% and 39.8% of patients with AR were mono- and polysensitized, respectively 14. A study performed in Spain showed sensitization to aeroallergens (measuring specific IgE) in 25.9% (121/468) of patients between 0 and 5 years of age with wheezing or atopic dermatitis 15. This difference in results could be explained by the high prevalence of atopy and allergic diseases in our country, as well as environmental factors such as climate, altitude and economic status.
DF was the most common aeroallergen; similar results have been reported by other authors 13,15. However, some other authors describe a greater sensitization to PD. A study carried out in an urban area of Mexico found that this mite (DF) was the most frequent allergen in school children with asthma (61%) (16, as well as in Jordan (11.9%) 6 and in the United States (31.2%) 17, the latter (US) being carried out on children with asthma who attended a pediatric pulmonary center. On the other hand, the most frequent sensitizing agents were olive pollen (18%) in Jordan (6. And in a study conducted in Spain 18 the most frequent sensitizing agents were grass (48%), tree (34%) and weed pollens (18%).
Other studies report insects in second or third place when talking about frequency, reaching 21.6% 19, 26.1% 13 or 32% 17. The high sensitivity to insects found in our study may be due to differences in housing and community environments 13. In our study, Alternaria alternata was predominant in fungal types. In contrast, Candida albicans and Cladosporum were the predominant fungi in a Colombian study in 12.9% of the patients (20. The frequency of sensitization was similar for cat and dog epithelium; similar results are evident in other reports 13,14,16-19.
The limitations of our study comprise not considering the climate where our patients reside, an aspect considered and recommended in other studies that found a greater frequency of sensitization for pollens and other allergens (6,18, moreover, we used only the skin test to evaluate sensitization and not the specific IgE level as other studies did 12,15,18.
In conclusion, most patients with asthma or AR were sensitized based on skin test results. The main sensitizing agent was DF, and sensitization was associated with age, age groups and total IgE level.
Acknowledgements:
The authors are grateful to all the study participants, to the Executive Office of Support for Research and Specialized Teaching (OASIDE) and to the Institutional Committee on Research Ethics (CIEI) of the National Institute of Child Health (INSN).
REFERENCES
1. World Allergy Organization. WAO White Book on Allergy: Update 2013 [Internet]. Milwaukee: WAO;2013 [citado el 3 de diciembre de 2019]. Disponible en: https://www.worldallergy.org/wao-white-book-on-allergy. [ Links ]
2. Global Initiative for Asthma. Global Strategy for Asthma Management and Prevention [Internet]. Fontana: GINA; 2019 [citado el 26 de noviembre de 2019]. Disponible en: https://ginasthma.org/2018-gina-report-global-strategy-for-asthma-management-and-prevention/. [ Links ]
3. Bousquet J, Khaltaev N, Cruz AA, Denburg J, Fokkens WJ, Togias A, et al. Allergic Rhinitis and its Impact on Asthma (ARIA) 2008 update (in collaboration with the World Health Organization, GA(2)LEN and AllerGen). Allergy. 2008;63 Suppl 86:8-160. doi: 10.1111/j.1398-9995.2007.01620.x. [ Links ]
4. Pearce N, Aït-Khaled N, Beasley R, Mallol J, Keil U, Mitchell E, et al. Worldwide trends in the prevalence of asthma symptoms: phase III of the International Study of Asthma and Allergies in Childhood (ISAAC). Thorax. 2007;62(9):758-66. doi: 10.1136/thx.2006.070169. [ Links ]
5. Björkstén B, Clayton T, Ellwood P, Stewart A, Strachan D, ISAAC Phase III Study Group. Worldwide time trends for symptoms of rhinitis and conjunctivitis: Phase III of the International Study of Asthma and Allergies in Childhood. Pediatr Allergy Immunol. 2008;19(2):110-24. doi: 10.1111/j.1399-3038.2007.00601.x. [ Links ]
6. Al-Zayadneh EM, Alnawaiseh NA, Altarawneh AH, Aldmour IH, Albataineh EM, Al-Shagahin H, et al. Sensitization to inhaled allergens in asthmatic children in southern Jordan: a cross-sectional study. Multidiscip Respir Med. 2019;14:37. doi: 10.1186/s40248-019-0199-y. [ Links ]
7. Johansson SGO, Bieber T, Dahl R, Friedmann PS, Lanier BQ, Lockey RF, et al. Revised nomenclature for allergy for global use: Report of the Nomenclature Review Committee of the World Allergy Organization, October 2003. J Allergy Clin Immunol. 2004;113(5):832-6. doi: 10.1016/j.jaci.2003.12.591. [ Links ]
8. Tschopp JM, Sistek D, Schindler C, Leuenberger P, Perruchoud AP, Wüthrich B, et al. Current allergic asthma and rhinitis: diagnostic efficiency of three commonly used atopic markers (IgE, skin prick tests, and Phadiatop). Results from 8329 randomized adults from the SAPALDIA Study. Swiss Study on Air Pollution and Lung Diseases in Adults. Allergy. 1998;53(6):608-13. doi: 10.1111/j.1398-9995.1998.tb03937.x. [ Links ]
9. Dreborg S, Backman A, Basomba A, Bousquet J, Dieges P, Malling HJ. Skin tests used in type I allergy testing Position paper. Sub-Committee on Skin Tests of the European Academy of Allergology and Clinical Immunology. Allergy. 1989;44 Suppl 10:1-59. [ Links ]
10. Robinson CL, Baumann LM, Gilman RH, Romero K, Combe JM, Cabrera L, et al. The Peru Urban versus Rural Asthma (PURA) Study: methods and baseline quality control data from a cross-sectional investigation into the prevalence, severity, genetics, immunology and environmental factors affecting asthma in adolescence in Peru. BMJ Open. 2012;2(1):e00421. doi: 10.1136/bmjopen-2011-000421. [ Links ]
11. Baumann LM, Romero KM, Robinson CL, Hansel NN, Gilman RH, Hamilton RG, et al. Prevalence and risk factors for allergic rhinitis in two resource-limited settings in Peru with disparate degrees of urbanization. Clin Exp Allergy. 2015;45(1):192-9. doi: 10.1111/cea.12379. [ Links ]
12. Nicholson A, Pollard SL, Lima JJ, Romero K, Tarazona-Meza C, Malpartida-Guzmán G, et al. Serum folate concentrations, asthma, atopy, and asthma control in Peruvian children. Respir Med. 2017;133:29-35. doi: 10.1016/j.rmed.2017.10.026. [ Links ]
13. Arbes SJ Jr, Gergen PJ, Elliott L, Zeldin DC. Prevalences of positive skin test responses to 10 common allergens in the US population: results from the third National Health and Nutrition Examination Survey. J Allergy Clin Immunol. 2005;116(2):377-83. doi: 10.1016/j.jaci.2005.05.017. [ Links ]
14. Bardei F, Bouziane H, Kadiri M, Rkiek B, Tebay A, Saoud A. Skin sensitisation profiles to inhalant allergens for patients in Tétouan city (North West of Morocco). Rev Pneumol Clin. 2016;72(4):221-7. doi: 10.1016/j.pneumo.2016.04.005. [ Links ]
15. Carvajal Urueña I, Díaz Vázquez C, Cano Garcinuño A, García Merino A, Morell Bernabé JJ, Pascual Pérez JM, et al. Perfil de sensibilización alérgica en niños de 0 a 5 años con sibilancias o dermatitis atópica. An Pediatría. 2010;72(1):30-41. doi: 10.1016/j.anpedi.2009.09.011. [ Links ]
16. Alcalá-Padilla G, Bedolla-Barajas M, Kestler-Gramajo A, Valdez-López F. Prevalencia de sensbilización a alergenos en niños escolares con asma que viven en la zona metropolitana de Guadalajara. Rev Alerg Mex. 2016;63(2):135-42. doi: 10.29262/ram.v63i2.184. [ Links ]
17. Nagarajan S, Ahmad S, Quinn M, Agrawal S, Manilich E, Concepcion E, et al. Allergic sensitization and clinical outcomes in urban children with asthma, 2013-2016. Allergy Asthma Proc. 2018;39(4):281-8. doi: 10.2500/aap.2018.39.4147. [ Links ]
18. Caro Rebollo J, Moneo Hernández MI, Cabañas Bravo MJ, Garín Moreno AL, Oliván Otal MP, Cenarro Guerrero T. Valoración del estudio alérgico en niños con atopia. Pediatría Aten Primaria. 2010;12(46):227-37. [ Links ]
19. Sánchez-Borges M, Capriles-Hulett A, Torres J, Ansotegui-Zubeldia IJ, Castillo A, Dhersy A, et al. Diagnosis of allergic sensitization in patients with allergic rhinitis and asthma in a tropical environment. Rev Alerg Mex. 2019;66(1):44-54. doi: 10.29262/ram.v66i1.570. [ Links ]
20. Bissinger I, Bareño J. Perfil de sensibilización a hongos en Medellín, Colombia. Rev Alerg Mex. 2016;63(2):123-34. doi: 10.29262/ram.v63i2.108. [ Links ]
Funding: Financial support was provided by the Executive Office of Support for Research and Specialized Teaching (OASIDE) of the National Institute of Child Health (INSN) (Project CL26-12).
Citation: García-Gomero D, López-Talledo MDC, Galván-Calle C, Muñoz-León R, Matos-Benavides E, Toribio-Dionicio C, et al. Sensibilización a aeroalérgenos en una población pediátrica peruana con enfermedades alérgicas. Rev Peru Med Exp Salud Publica. 2020;37(1):57-62. Doi: https://doi.org/10.17843/rpmesp.2020.371.4460.
Received: May 09, 2019; Accepted: January 08, 2020











 texto en
texto en 


