Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista Peruana de Ginecología y Obstetricia
versión On-line ISSN 2304-5132
Rev. peru. ginecol. obstet. vol.67 no.4 Lima oct./dic 2021
http://dx.doi.org/10.31403/rpgo.v67i2367
Original Articles
Prenatal diagnosis of intra-abdominal varicose vein of the fetal umbilical vein
1 Directorate of Integrated Health Networks Lima Centro, Lima, Peru
2 Academic Department of Obstetrics and Gynecology, Faculty of Human Medicine, Universidad Nacional Mayor de San Marcos, Lima, Peru
3 Fetal Medicine Service, Instituto Nacional Materno Perinatal, Lima, Peru
Objective
: To determine by ultrasound the frequency and type of perinatal complications in pregnant women with grade 3 placenta before 35 weeks.
Methods
: Analytical, observational, retrospective, cross-sectional, retrospective study that included all pregnant women diagnosed with grade 3 placenta by ultrasound between 23 and before 35 weeks. The pregnant women did not present comorbidity, multiple pregnancy or fetuses with malformations.
Results
: A total of 235 pregnant women with grade 3 placenta by ultrasound were found, of which 119 were randomly sampled. The frequency of perinatal complications in pregnant women with grade 3 placenta by ultrasound before 35 weeks was 29.4%, the most frequent being low birth weight (18.5%) and respiratory distress syndrome (17.6%). The chi-square test resulted 0.000 for gestational age at birth and 0.015 for gestational age at diagnosis, with significance level p < 0.05 of association of complications in pregnant women with placenta grade 3 before 35 weeks.
Conclusion
: Ultrasound diagnosis of early placental aging was associated with a high frequency of perinatal complications.
Key words: Placenta; Ultrasonography; Pregnancy complications
INTRODUCTION
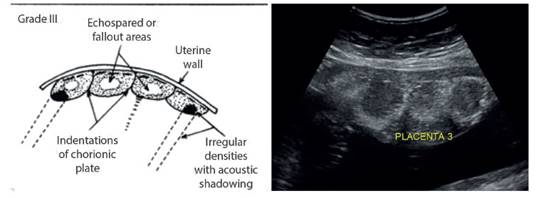
Grannum1, in 1979, was the first to propose a classification of placental maturity based on its ultrasound characteristics. According to his research, there are four grades of placental maturation, from grade 0 to grade 3, the latter representing the mature placenta. The chorionic plate appears interrupted by indentations that extend to the basal layer and probably represent the inter cotyledonary septa. As a result, the placental substance is divided into compartments that presumably demarcate the cotyledons. The central part of these compartments shows econegative areas. In addition, irregularly shaped dense echogenic areas appear near the chorionic plate (Figure 1).
According to the review of the scientific literature, the importance or clinical significance of early placental calcifications is controversial, since for some it is associated with adverse perinatal outcomes such as intrauterine growth restriction (IUGR)2-5), low birth weight2-4,6-7, Apgar less than 77, fetal distress4 and pregnancy-induced hypertension(3,6,8) -, while for others there is no association with these findings5,11.
There are only two national publications on placental aging before 35 weeks, carried out in the 1980s and 1990s, which aim to evaluate perinatal outcomes and in which only IUGR and respiratory problems are taken into account12,13. There are also no management protocols when the diagnosis of early placental aging is made, despite the fact that the incidence reported internationally is very variable, ranging from 0.8% to 15.4%4), depending on the population studied.
In the Fetal Medicine Service of the National Maternal-Perinatal Institute, an average of 700 ultrasound scans are performed per month14, most of which (approximately 60%) are done on pregnant women between 26 and 36 weeks. The percentage of pregnant women diagnosed with grade 3 placenta before 35 weeks was 7.7%, which is within the international average and for which there is no consensus regarding prognosis and perinatal complications.
The present study aims to determine the frequency, type and relationship between the ultrasound finding of a grade 3 placenta before 35 weeks (early placental aging) and perinatal complications, in order to define management strategies in patients with this finding.
METHODS
This is an observational study, with data obtained retrospectively and analyzed cross-sectionally. All pregnant women who attended the Fetal Medicine service for ultrasound evaluation between 23 and 34 weeks during 2017 had their placental maturation grade recorded. Only pregnant women with placenta grade 3 at the time of evaluation were included in the study. Pregnant women with unknown date of last menstrual period or who did not have a first trimester ultrasound were excluded, as well as those with multiple pregnancies, fetuses with malformations, mothers smokers, hypertensive women or with a previous diagnosis of preeclampsia. The data were recorded in an Excel spreadsheet and processed in SPSS v24.0.
The descriptive characteristics of the pregnant women with grade 3 placenta before 35 weeks were tabulated, determining the mean and standard deviation. Perinatal complications were evaluated according to maternal age, parity, delivery route and gestational age at birth, using Spearman's correlation for quantitative and qualitative variables and chi-square for qualitative variables only22.
RESULTS
A total of 3,065 ultrasound scans were performed in pregnant women between 23 and 34 weeks. After excluding the pregnant women who did not meet the inclusion requirements, 235 pregnant women with grade 3 placenta were left, from which a sample of 119 pregnant women was obtained by simple random probabilistic sampling, the results of which are analyzed.
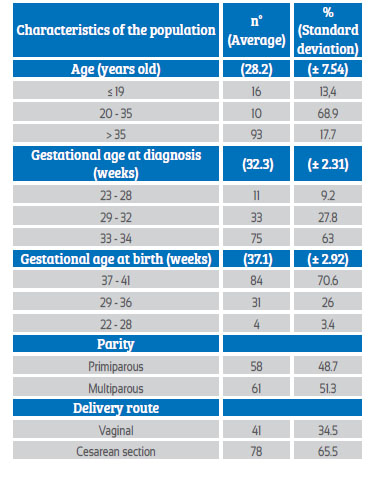
The mean age of the pregnant women diagnosed with grade 3 placenta by ultrasound was 28.2 years, with a minimum age of 15 years and a maximum age of 46 years. Regarding parity, most were multiparous (51.3%) and the route of delivery was predominantly cesarean section (65.5%). The mean gestational age at the time of diagnosis of grade 3 placenta was 32.3 weeks, with the minimum gestational age at diagnosis being 25 weeks and the maximum 34 weeks. As for gestational age at birth, the mean was 37 weeks, with the minimum gestational age at birth being 27 weeks and the maximum age 41 weeks (Table 1).
Table 1 Descriptive characteristics of pregnant women with grade 3 placenta by ultrasound before 35 weeks.

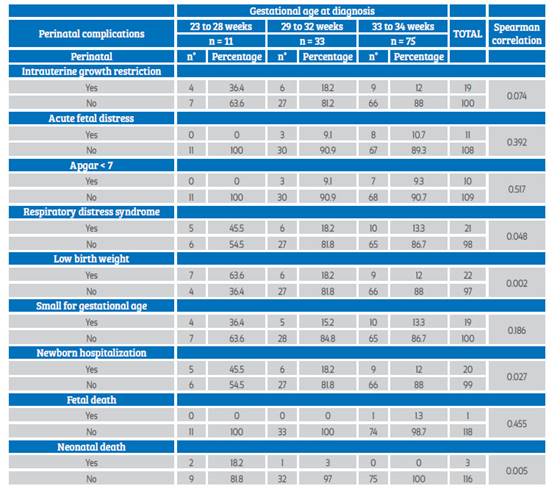
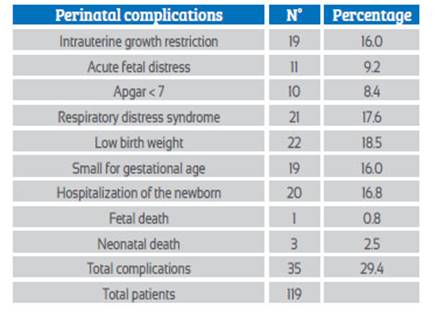
35 patients out of a total of 119 presented one or more of the complications studied, which constitutes a high percentage (29.4%), the most frequent complication being low birth weight (18.5%) followed by respiratory distress syndrome (17.6%). 16.8% of the newborns born to mothers with placenta G3 before 35 weeks required hospitalization. Only one case of fetal death (0.8%) and 3 cases of neonatal death (2.5%) were recorded (Table 2).
Table 2 Perinatal complications in pregnant women with grade 3 placenta by ultrasound before 35 weeks

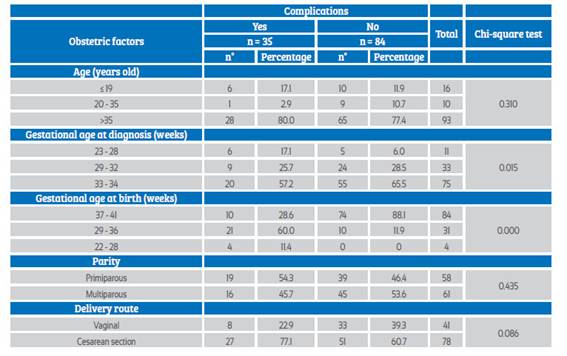
The analysis of perinatal complications according to the obstetric factors studied reveals that neither maternal age, nor parity, nor the route of delivery have a significant influence on the results, unlike gestational age at diagnosis and gestational age at birth, which show a p value of less than 0.05 (Table 3).
Table 3 Perinatal complications in pregnant women with grade 3 placenta before 35 weeks, according to obstetric factors.
A more detailed analysis of perinatal complications according to gestational age at the time of diagnosis of grade 3 placenta by ultrasound allows us to observe that respiratory distress syndrome, low birth weight, hospitalization of the newborn and neonatal death were significantly associated with gestational age at the time of diagnosis (Table 4).
DISCUSSION
The present study allows us to know the relationship between early placental aging and perinatal outcomes in the population evaluated.
The correlational analysis between perinatal complications and obstetric factors revealed a statistically significant relationship only with gestational age at birth and gestational age at the time of diagnosis of grade 3 placenta.
Regarding perinatal complications in the study group, they are similar to those found by other researchers, such as Jamal15, Chen16, Chitlange23, Quinlan(9), the most frequent being low birth weight. It should be pointed out that other researchers did not find an increase in the frequency of perinatal complications in the group of patients with grade 3 placenta, with the exception of IUGR3,12,19.
Regarding gestational age at the time of diagnosis of grade 3 placenta, the results of this study reveal that the lower the gestational age at which grade 3 placenta is diagnosed, the higher the percentage of perinatal complications, a finding similar to that reported by Chen15 and Jamal16.
This last finding is the most important, since it would allow us to infer that when placental aging occurs at early gestational ages it is not a physiological process, but a reflection of an underlying placental dysfunction, which may be due to different pathological processes such as subclinical infections18-19, metabolic disorders20 or hypertension21. In our study we found one case of fetal death and two cases of neonatal death, all in the group of pregnant women with gestational age less than 33 weeks at the time of diagnosis of grade 3 placenta. This finding could correlate with the role of placental aging as a risk factor for placental dysfunction and probably perinatal death16. Larger studies with a larger population may provide more accurate results.
The main limitation of the present study lies in its retrospective nature and small sample size, so prospective multicenter case-control studies are needed to allow stronger associations.
CONCLUSIONS
The diagnosis of early placental aging has a high frequency of perinatal complications. The overall analysis allows us to conclude that both gestational age at birth and at the time of diagnosis are significantly associated with perinatal complications in pregnant women with grade 3 placenta before 35 weeks.
REFERENCES
1. Grannum PA, Berkowitz RL, Hobbins JC. The ultrasonic changes in the maturing placenta and their relation to fetal pulmonic maturity. Am J Obstet Gynecol. 1979;133(8), 91522. [ Links ]
2. Patterson RM, Hayashi RH, Cavazos D. Ultrasonographically observed early placental maturation and perinatal outcome. Am J Obstet Gynecol. 1983;147:773-7. [ Links ]
3. McKenna D, Tharmaratnam S, Mahsud S, Dornan J. Ultrasonic evidence of placental calcification at 36 weeks' gestation: maternal and fetal outcomes. Acta Obstet Gynecol Scand. 2005 Jan;84(1):7-10. doi: 10.1111/j.00016349.2005.00563.x [ Links ]
4. Lei H, Wen SW, Central-South China Fetal Growth Study Group. Distribution of placental grading by gestational age. JSOGC. 2000;22(5),374-6. [ Links ]
5. Hill LM, Breckle R, Ragozzino MW, Wolfgram KR, O'Brien PC. Grade 3 placentation: incidence and neonatal outcome. Obstet Gynecol. 1983;61:728-32. [ Links ]
6. Hills D, Irwin GA, Tuck S, Baim R. Distribution of placental grade in high-risk gravidas. AJR Am J Roentgenol. 1984;143:1011-3. [ Links ]
7. Proud J, Grant AM. Third trimester placental grading by ultrasonography as a test of fetal wellbeing. Br Med J (Clin Res Ed). 1987;294(6588):1641-4. [ Links ]
8. Kazzi GM, Gross TL, Rosen MG, Jaatoul-Kazzi NY. The relationship of placental grade, fetal lung maturity, and neonatal outcome in normal and complicated pregnancies. Am J Obstet Gynecol. 1984;148:54-8. [ Links ]
9. Quinlan RW, Cruz AC, Buhi WC, Martin M. Changes in placental ultrasonic appearance. I. Incidence of grade III changes in the placenta in correlation to fetal pulmonary maturity. Am J Obstet Gynecol. 1982;144:468-70. [ Links ]
10. Vosmar MB, Jongsma HW, van Dongen PW. The value of ultrasonic placental grading: no correlation with intrauterine growth retardation or with maternal smoking. J Perinat Med. 1989;17:137-43. [ Links ]
11. Miller JM, Brown HL, Kissling GA, Gabert HA. The relationship of placental grade to fetal size and growth at term. Am J Perinatol. 1988;5(01):19-21. [ Links ]
12. Robles M, Da Silva A. Madurez placentaria precoz detectada por ultrasonografía: incidencia y resultado perinatal. An Diagnóstico Perú. 1986;18(2):37-43. [ Links ]
13. Robles MH. Madurez placentaria precoz de grado: III. Diagnóstico y utilidad clínica en el Hospital Nacional Cayetano Heredia. [Tesis] Lima: UPCH. Facultad de Medicina Alberto Hurtado; 1993. [ Links ]
14. Oficina de Estadística e Informática INMP. 2018. Boletín Estadístico 2017. Recuperado el 10 de junio del 2021. Website: https://www.inmp.gob.pe/institucional/boletines-estadisticos/1422371837 [ Links ]
15. Chen KH, Chen LR, Lee YH. Exploring the relationship between preterm placental calcification and adverse maternal and fetal outcome. Ultrasound Obstet Gynecol.. 2011 Mar;37(3):328-34. doi: 10.1002/uog.7733 [ Links ]
16. Jamal A, Moshfeghi M, Moshfeghi S, Mohammadi N, Zarean E, Jahangiri N. Is preterm placental calcification related to adverse maternal and foetal outcome? J Obstet Gynaecol. 2017 Jul;37(5):605-9. doi: 10.1080/01443615.2017.1285871 [ Links ]
17. Walker MG, Hindmarsh PC, Geary M, Kingdom JC. Sonographic maturation of the placenta at 30 to 34 weeks is not associated with second trimester markers of placental insufficiency in low-risk pregnancies. J Obstet Gynaecol Canada. 2010 Dec;32(12):1134-9. doi: 10.1016/S17012163(16)34736-3 [ Links ]
18. Agababov RM, Abashina TN, Suzina NE, Vainshtein MB, Schwartsburd PM. Link between the early calcium deposition in placenta and nanobacterial-like infection. J Bio Science. 2007;32:1163-8. [ Links ]
19. Pasquinelli G, Papadopulos F, Nigro M. Nanobacteria and psammoma bodies: ultrastructural observations in a case of pathological placental calcification. Ultrastruct Pathol. 2010 Dec;34(6):344-50. doi: 10.3109/01913123.2010.504323 [ Links ]
20. Emmrich P. Pathology of the placenta. X. Syncytial proliferation, calcification, cysts, pigments and metabolic disorders. Zentralbl Pathol 1992;138:77-84. [ Links ]
21. Sultana Z, Maiti K, Dedman L, Smith R. Is there a role for placental senescence in the genesis of obstetric complications and fetal growth restriction? Am J Obstet Gynecol. 2018 Feb;218(2S):S762-S773. doi: 10.1016/j.ajog.2017.11.567 [ Links ]
22. Lizama P, Bocardo G. Guía de Asociación entre variables (Pearson y Spearman en SPSS). Universidad de Chile Facultad de Ciencias Sociales. 2014. Recuperado el 30 de Julio del 2021. Website: https://www.u-cursos.cl/facso/2014/2/SO01007/1/material_docente/bajar?id_material=994690. [ Links ]
23. Chitlange SM, Hazari KT, Joshi JV, Shah RK, Mehta AC. Ultrasonographically observed preterm grade III placenta and perinatal outcome. Int J Gynaecol Obstet. 1990;31:325-8. [ Links ]
Authorship recognition: Both authors contributed equally to this work Funding: Self-funded publication
Received: June 14, 2021; Accepted: August 06, 2021











 texto en
texto en