Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista Peruana de Ginecología y Obstetricia
On-line version ISSN 2304-5132
Rev. peru. ginecol. obstet. vol.68 no.3 Lima July/Sep. 2022 Epub Sep 22, 2022
http://dx.doi.org/10.31403/rpgo.v68i2439
Case report
Vulvar fibroadenoma: case report
1. Pathologist, Institute of Pathology, Universidad Nacional Mayor de San Marcos, Lima, Peru. Hospital Carlos Lanfranco La Hoz, Puente Piedra, Lima, Peru
Fibroadenoma is a benign neoplasm usually located in the breast. Its vulvar location is extremely rare, with few cases published. Its origin is uncertain and highly debatable, as it is thought that it may originate from vulvar ectopic breast tissue or from anogenital glands similar to normally existing breast tissue. An unusual case of vulvar fibroadenoma is presented in a 29-year-old woman who for two years presented with a vulvar lump that caused dyspareunia and postcoital bleeding. At the level of the labium majus of the vulva, a well-demarcated tumor measuring 3 x 2 x 2 cm, whitish, with a firm consistency was excised. Microscopy showed a fibroadenoma which by immunohistochemistry showed positivity for estrogen and progesterone receptors.
Keywords: Fibroadenoma; Vulva
INTRODUCCIÓN
Fibroadenoma is a benign tumor consisting of mixed glandular epithelial and fibrous stromal tissue. It occurs very frequently in the breast, but its presence in the vulva is exceptional and of very low incidence. Few cases have been published in the world literature. The first case was reported by Friedel(1), in Germany in 1932, then Fisher2 in 1947, Siegler3 in 1951, Burger4 in 1954 and Baruah5 in 1967. It is indicated that there are about 50 cases.
The histogenesis of vulvar fibroadenoma is uncertain and controversial. Two hypotheses have been proposed. The first one is that it would originate in an aberrant mammary tissue in the vulva when the embryonic involution of the primitive mammary crest fails. The second hypothesis exposed by Van der Putte6), in 1994, is that it would originate not from a true mammary tissue but from specialized anogenital glands similar to mammary glands (mammary-like glands), with strong relation to the eccrine glands that normally exist in that area. This second hypothesis had already been suggested by Champneys, in 18845), who considered that the supernumerary mammary glands in vulva are enlarged sweat glands or eccrine sweat glands with mammary differentiation and not true mammary tissue. Recent observations in human embryos have not shown that the migration of mammary gland cells from the primordium extends to the anogenital area; hence the concept of the presence of vulvar mammary tissue as a derivation of the primitive mammary crest is not sustainable, according to Van der Putte6).
Vulvar fibroadenoma has been found in women between 18 and 80 years of age and clinically presents as a subcutaneous nodular mass of insidious growth, mostly sessile, with a few pedunculated cases7). The size varies from 1 to 12 cm in diameter, although Zhang8 reported in an 18-year-old girl a vulvar tumor that had appeared 7 years earlier and was typified as fibroma and fibroadenoma, measuring 30 x 40 x 4 cm and weighing 2000 g. Most cases are of unilateral location, but some cases of bilateral presentation have also been published(9). The treatment is tumor excision, the prognosis is good, and no recurrence has been observed.
CASE REPORT
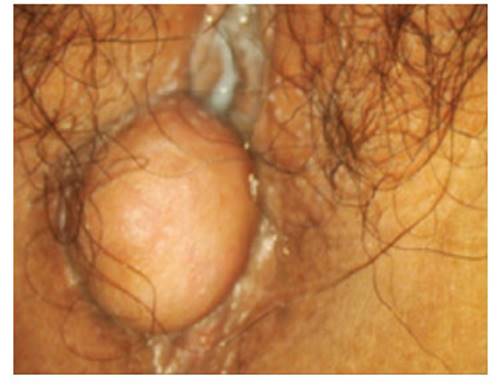
A 29-year-old woman presented two years ago with a tumor at the level of the perineum that grew slowly and progressively; recently it was accompanied by dyspareunia and postcoital bleeding. On gynecological examination, a subcutaneous, rounded, mobile, firm, well-defined, well-defined tumor of firm consistency, not adherent to the deep planes, was observed at the level of the right labium majus of the vulva. It was excised in its entirety (Figure 1).
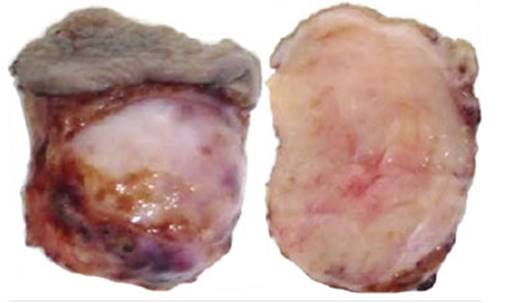
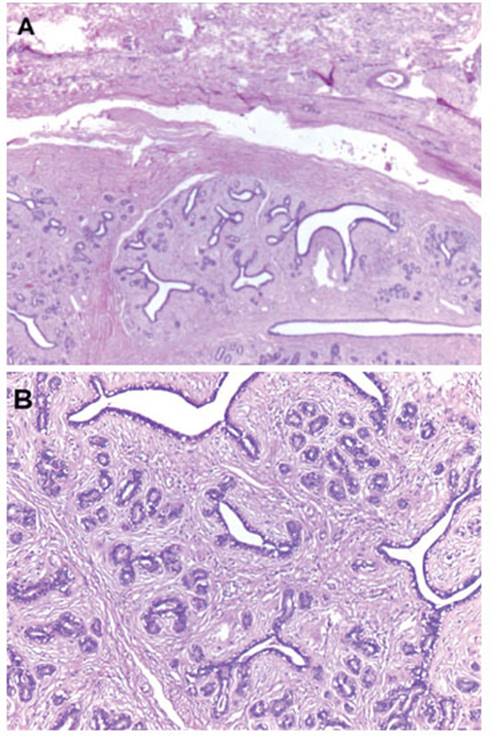
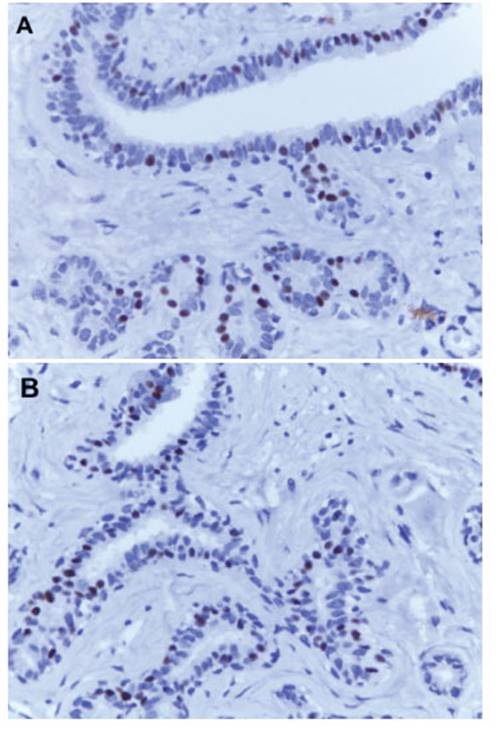
In pathological anatomy, a 2 x 0.8 cm skin slough with a whitish nodular subcutaneous tumor of 3 x 2 x 2 cm of major diameters was received. The external surface was smooth, well defined, regular cut (Figure 2). Microscopy showed the histology of a fibroadenoma (Figure 3A and 3B), a biphasic neoplasm composed of benign proliferation of ductal structures and dense conjunctival tissue, well delimited by scarce fibrous tissue. On immunohistochemistry, the ductal structures were positive for estrogen (Figure 4A) and progesterone receptors (Figure 4B). No glandular tissue was observed adjacent to the fibroadenoma.
DISCUSSION
Tow SH (1962)10 mentions that Hartur, in 1874, would have made the first report of a mammary gland in the vulva that presented with milky discharge. In the publication of Deber and McFarland9,10), in 1918, of 430 cases of extramammary tissue, 90% were in the axilla, others in the thorax, abdomen and only one case in the vulva. Baruah5), in 1967, compiled from the English literature 17 cases of mammary tissue in the vulva; in this casuistry he presented 4 cases of fibroadenoma, including his own. Kasakov11, in 2011, from his personal experience published 300 cases of various lesions related to the anogenital mammary glands, both benign and malignant lesions that showed similar morphology with their mammary counterparts. In 2021, Buitrago SM collected 126 cases from 94 reports of mammary tissue in vulva and found 23 cases of vulvar fibroadenoma12).
VULVAR FIBROADENOMA: CASE REPORT
To date, the hypothesis that the presence of specialized anogenital glands similar to the breast would be part of the normal structure of the vulva is gaining more relevance, despite the fact that the histological structure and immunohistochemical pattern are identical to those of their breast tissue counterparts. So is the presence of benign and malignant tumor lesions such as fibroma, intracystic papilloma, lactational adenoma13), phyllodes14), fibrocystic disease, pseudoangiomatous stromal hyperplasia, sclerosing adenosis, extramammary Paget's disease, ductal adenocarcinoma15, lobular and mucinous adenocarcinoma7 and sarcoma, whose behavior, clinical presentation, histology, treatment and prognosis are similar to those of the breast and with which the differential diagnosis should be made.
In conclusion, fibroadenomas located in the vulva are extremely rare. Their origin remains under debate and, despite their macroscopic characteristics of benign lesion, histologic study with relevant immunohistochemical techniques should be performed in order to have an accurate diagnosis and to rule out other vulvar tumors. We present the case to add it to the casuistry of this rare presentation.
REFERENCES
1. Friedel R. Ein Fibroadenom einer Nebenbrustdriise im rechten Labium maius. Virchovvs Arch f path Anat. 1932;286:62-9. [ Links ]
2. Fisher JH. Fibroadenoma of supernumerary gland tissue in vulva. Am J Obstet Gynecol. 1947;53;335-7. doi: 10.1016/0002-9378(47)90361-x [ Links ]
3. Siegler AM, Gordon R. Fibroadenoma in a supernumerary breast of the vulva. Am J Obstet Gynecol. 1951;62(6):1367-9. doi:10.1016/0002-9378(51)90069-5 [ Links ]
4. Burger RA, Marcuse PM. Fibroadenoma of vulva. Am J Clin Pathol. 1954;24;965-8. doi: 10.1093/ajcp/24.8.965. PMID: 13197326 [ Links ]
5. Baruah BD, Dam PK, Choudhury MA. Fibroadenoma in a supernumerary gland of the vulva. J Obstet Gynaecol India. 1968;302-9. [ Links ]
6. van der Putte SC. Mammary-like glands of the vulva and their disorders. Int J Gynecol Pathol. 1994 Apr;13(2):150-60. doi: 10.1097/00004347-199404000-00009 [ Links ]
7. Kalyani R, Srinivas MV, Veda P. Vulval fibroadenoma a report of two cases with review of literature. Int J Biomed Sci. 2014;10(2):143-5. PMID: 25018684; PMCID: PMC4092083 [ Links ]
8. Zhang J, Chen Y, Wang K, Xi M, Yang K, Liu H. Prepuberal vulvar Fibroma with a coincidental ectopic breast Fibroadenoma: Report of an unusual case with literature review. J Obstet Gynecol Res. 2011;37(11):1720-5. doi:10.1111/j.14470756.2011.01580.x [ Links ]
9. Hassim AM: Bilateral fibroadenoma in supernumerary breast of the vulva. Br J Obstet Gynaecol Common.1969;76:275-7. doi: 10.1111/j.14710528.1969.tb05834.x.PMID: 5775152 [ Links ]
10. Tow SH, Shanmugaratnam K. Supernumerary Mammary Gland in the Vulva. Brit Med J. 1963;10:1234-6. doi:10.1136/ bmj.2.5314.1234 [ Links ]
11. Kazakov DV, Spagnolo DV, Kacerovska D, Michal M. Lesions of anogenital mammary-like glands: an update. Adv Anat Pathol. 2011 Jan;18(1):1-28. doi: 10.1097/PAP.0b013e318202eba5. PMID: 21169735 [ Links ]
12. Buitrago SM, Barrera SH, Morante C. Tejido mamario ectópico en vulva: reporte de caso y revisión sistemática de la literatura. Rev Colomb Obstet Ginecol. 2021;72:271-90. ISSN 2463-0225 [ Links ]
13. Anunobi CC, Obiajulu FJ, Banjo AA, Okonkwo AO. Vulva fibroadenoma associated with lactating adenoma in a 26-yearold Nigerian female. Case Rep Pathol. 2013;2013:195703. doi:10.1155/2013/195703 [ Links ]
14. Lee S, Nodit L. Phyllodes tumor of vulva: a brief diagnostic review. Arch Pathol Lab Med. 2014 Nov;138(11):1546-50. doi: 10.5858/arpa.2013-0581-RS. PMID: 25357118 [ Links ]
15. Intra M, Maggioni A, Sonzogni A, De Cicco C, Machado LS, Sagona A, Talakhadze N. A rare association of synchronous intraductal carcinoma of the breast and invasive carcinoma of ectopic breast tissue of the vulva: case report and literature review. Intern J Gynecol Cancer. 2006;16(S1):428-33. doi:10.1111/j.1525-1438.2006.00237.x [ Links ]
Received: March 09, 2022; Accepted: July 07, 2022











 text in
text in