Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista de la Facultad de Medicina Humana
Print version ISSN 1814-5469On-line version ISSN 2308-0531
Rev. Fac. Med. Hum. vol.20 no.3 Lima Jul-Sep 2020
http://dx.doi.org/10.25176/rfmh.v20i3.3170
Original article
Prognostic factors and survival study in high-grade glioma in a Hospital in Lima, Peru
1Universidad Nacional de Trujillo, Trujillo-Perú
2Facultad de Ciencias de la Salud, Universidad Científica del Sur, Lima-Perú.
Introduction:
Gliomas are primary tumors of the central nervous system. They are classified from grade I-IV, with high grade III and IV being the most frequent and with poor prognosis.
Objective:
To determine the prognostic factors of survival in patients with high-grade gliomas in a hospital in Lima, Peru.
Methods:
The medical records with high-grade glioma from 2010-2014 were retrospectively reviewed, ten variables were analyzed with Kaplan-Meier and Log Rank survival graphs and the Cox regression model.
Results:
Out of a total of 278 patients with high-grade gliomas, 136 were men and 142 women. The analysis of Progression-Free Survival (SLP) had a range of 5.6-80.3 (median 22.7) and the analysis of overall survival (PS) had a range of 4-83.2 (median 26, 2 months. The overall survival for the IV grade tumor was 15.7 months (95% CI 14.2-17.1); the III degree was 38.4 months (95% CI 35.8-40.9). The grade (PS: HR 15; SLP: HR 25.1); surgical treatment (PS: HR 0.6; SLP: HR 0.49), age (PS: HR 1.47; SLP: HR 1.7), adjuvant treatment (PS: HR 0.6; SLP: HR 0 , 58) and karnofsky (PS: HR 0.7) were correlated; while the Karnofsky for SLP does not (P = 0.146).
Conclusion:
Age, functional status, surgical treatment, adjuvant treatment, and tumor grade are prognostic factors for PS. In contrast, for SLP the prognostic factors were age, surgical treatment, adjuvant treatment, and tumor grade.
Keywords: progression-free survival; Karnofsky Performance Status; glioma (source MeSH NLM)
INTRODUCTION
Glioma is a primary tumor of the central nervous system and is classified in grades I-IV according to histopathological criteria1, according to 2007 WHO classification criteria, grades III-IV are called high grade (two).
The term "high-grade glioma" includes several tumor names such as glioblastoma multiforme (GBM), anaplastic astrocytoma (AA), and anaplastic oligodendroglioma (OA). GBM is the most frequent tumor and corresponds to 80% of gliomas and the most aggressive, and affects approximately2-3people out of every 100,000 annually3,4. However, the overall prognosis for glioma remains bad despite aggressive treatments, especially in patients with high-grade glioma, whose average survival time after surgery is only 12 to 15 months for glioblastoma and 2 to 5 years anaplastic glioma.5,7
Treatment of patients with high-grade gliomas remains a challenge for modern therapy. The prognosis of these patients is poor, the median patient survival after diagnosis is approximately 1 year5,8. The need for histological diagnosis of tumor tissue in each case and the importance of decompression in symptomatic patients are well established, however, there is still controversy regarding the extent of surgical resection to be performed. Although many neurosurgeons recommend that gliomas can be resected as widely as possible9,10, rigorous literature reviews have shown that there is little scientific evidence that aggressive surgical treatment significantly prolongs survival.11,12
The standard treatment for high-grade gliomas is multidisciplinary, but above all, the treatment is surgical13,14. Total surgical resection is essential to increase patient survival, associated with chemotherapy and post-surgical adjuvant radiation therapy. In the past, surgical treatment was accompanied by important sequelae that led to low quality of life. Precisely, the maximum possible resection allows a better effect of radiotherapy in the control of the disease, increasing the survival of patients. Chemotherapy is part of the multidisciplinary management of gliomas, with an improvement in survival observed when associated with radiation therapy.15,16
Due to the fact that the survival factors in our environment are not yet clear, and the impact on health in the population is also uncertain, it is necessary to know a profile of patients with a greater and lesser chance of survival, for better decision-making, based on the evidence of our environment.
METHODS
Design and setting
Analytical, longitudinal, retrospective of survival. Performed in postoperative patients with high-grade glioma from the 2010-2014 period in the neurosurgery service of the Hospital Nacional Edgardo Rebagliati Martins.
Population and sample.
The population is all patients operated on for glioma, who were attended in the consulting room and emergency of the neurosurgery service of the Hospital Nacional Edgardo Rebagliati Martins.
Consecutive non-random sample. Information was collected from the medical records of the postoperative patients with high-grade glioma from the 2010-2014 period.
Inclusion criteria: 1) Patients older than 18 at the time of diagnosis; 2) Patients with a diagnosis of high-grade glioma confirmed by the pathological study, and 3) Patients who have undergone some type of surgical treatment.
Exclusion criteria: 1) Patients who have undergone more than one surgical intervention; and 2) Patients who have an incomplete imaging study; 3) Patients who have presented post-surgical complications inherent to the procedure, and 4) Incomplete medical records
Variables and instruments
Dependent variables
Overall Survival (PS):These are the months of life from the time of surgery to death from the disease. The final expression was in months. It was measured through the logarithmic range method and the Cox proportional hazards regression analysis.
Progression-free survival (PFS):These are the months of life from the moment of the surgical intervention until the reappearance of tumor recurrence. The final expression was in months. It was measured using the logarithmic range method and Cox proportional hazards regression analysis.
Independent variables
Histological grade:Defined by the microscopic characteristics of the tumor tissue and classified according to the WHO, defined by the anatomic pathology report. In the study, it was measured in (1) grade III or (2) IV.
Age:It is the lifetime of the patient taken since birth, which has been measured in years recorded on your health insurance. It was categorized into three stages: (1) 14-30 years; (2) 31-60 years; and (3)> 60 years.
Gender:It is either male or female, as registered on your health insurance affiliation sheet (qualitative - nominal).
Seizures:It is the generalized clonic tonic movement that is part of the symptomatic picture at the time of diagnosis. It was categorized as "yes" and "no" according to medical history.
Ability to perform routine tasks:It is a way to quantify the ability of cancer patients to perform routine and/or daily tasks. For this, we will use the Karnofsky Performance Scale (KPS). It was categorized with a cutoff point "≥ 70" and "<70" according to what is recorded in medical history.
Glioma location: It is the location of the tumor lesion in the cerebral hemisphere, visualized in cerebral magnetic resonance imaging. It was categorized into: (1) Frontal; (2) Parietal; (3) Occipital; (4) Temporary; (5) More than 1 area involved; and (6) Infratentorial.
Tumor diameter:It is the measurement in centimeters of the largest diameter (in any dimension) on FLAIR images and / or T2 sequence of magnetic resonance imaging. It was categorized into (1) ≥ 5 cm and (2) <5 cm.
Enveloping eloquent area:It is the location of the tumor in areas that dominate the sensory-motor functions (precentral and postcentral gyrus), language areas (upper temporal area, lower frontal area, and lower parietal area), basal ganglia, visual area (calcarine visual cortex). It was categorized as "yes" when it compromised these areas, and "no" if it did not.
Surgical resection extension:It is the percentage of tumor extraction taking into account the pre-surgical and post-surgical images. It was categorized into: (1) Total; (2) Partial; and (3) Biopsy.
Adjuvant Treatment:It is the presence of Radiotherapy and/or chemotherapy treatment after surgery. Evidenced in medical history by the sessions it received. It was categorized into: (1) RT / QT; (2) RT; and (3) No RT.
Procedures
Patient Selection:
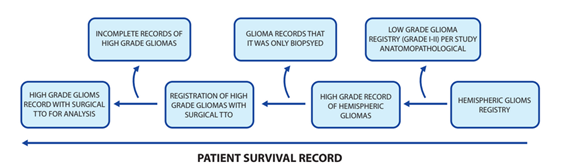
In the database of the archive of medical histories the Hospital Nacional Edgardo Rebagliati Martins, 200 histories of patients with high-grade glioma who received surgical treatment, craniectomy plus tumor excision, was chosen between the years 2010-2014. All patients present histological confirmation of high-grade glioma, grade III, and IV according to the classification system of the
World Health Organization.
Acquisition of the variables:
The following data were obtained from the medical records of the patients:1Demographic Data (age and sex) and the ability to perform routine tasks (KFS) before the operation.2preoperative clinical symptoms: intracranial hypertension, irritation, and symptoms of nervous exhaustion and its duration.3Preoperative Magnetic Resonance Imaging (MRI): before the operation, MRI contrast was performed to determine if there was hemorrhage or necrosis of the tumor, tumor location, the extent of tumor invasion, and tumor size. The extent of tumor invasion is based on the number of lobes with high T2-weighted MRI signals4. Treatment of: (a) surgical resection is the extent of tumor resection during operation by neurosurgeons and during the study of post-operative images analyzed by radiologists. Total resection of the tumor mass was less than 5% tumor residue (to protect important neurological functions). Subtotal resection was the removal of more than 80% of the tumor mass (b) Postoperative Radiotherapy is the postoperative radiotherapy which was given to patients at a routine dose: 40-60 Gy / 28 days to the tumor and edematous peripheral area 2 cm outside of it, plus 10 to 14 Gy applied to the region of the brain that surrounds 2 cm. (c) postoperative chemotherapy: standard chemotherapy (200 mg temozolomide / m2 body surface area) was administered 4-6 course of treatment and during radiotherapy, the temozolomide dose was halved.5Postoperative pathologic data: Based on pathologic examinations, patients were diagnosed with anaplastic astrocytoma, anaplastic oligodendroglioma, or anaplastic mixed glioma and with grades III and IV.6Follow-up data include disease outcomes with PS and SLP. Follow-up data was collected mainly when patients visited outpatient clinics and in telephone interviews with patients and / or family members. The rest of the data was obtained from medical records.
Statistical analysis
The summary measures of the data were presented as means ± standard deviations for the parametric data and as medians with IQRs for non-parametric data. Statistical methods were performed with the SPSS v23.0 program. The Kaplan-Meier survival analysis, the logarithmic range method, and the Cox proportional hazards regression analysis were used to analyze the effect of the different variables with time on PS and SLP. A p-value of less than 0.05 was considered statistically significant.
Ethical aspects.
The data was collected by the study researchers. At the same time, permission was obtained from the hospital for the investigation. Finally, the information of the participants was delivered in a Microsoft Excel 2016 spreadsheet without biological identifiers, maintaining the confidentiality of the data.
RESULTS
Of a total of 305 patients with high-grade gliomas, which were identified in the collected database, 278 patients met the inclusion criteria. Of these 136 were men and 142 women; the median age of the total was 51 years of age. The most frequent high-grade glioma was grade IV (51.4%). Most of the high-grade gliomas had supratentorial location (252 patients, 90.7%); 23.4% of the patients had their tumor located in eloquent areas; 65.5% of the patients had tumors with a diameter ≥ 5cm. The initial surgical treatment was resection in 95.7% of cases. Only 12 patients underwent biopsy. 174 (62.6%) patients presented a functional state greater than or equal to 70% on the Karnofsky scale. Headache was present in 69.1%. Furthermore, 20.5% of the patients presented with Idiopathic intracranial hypertension (IIH). In the adjuvant treatment, 83.5% received radiotherapy and 60.8% received chemotherapy. The analysis of PFS time had a range of 5.6-80.3 with a mean of 22.7 months and the analysis of the follow-up of survival time had a range of 4-83.2 and a mean of 26.2 months .
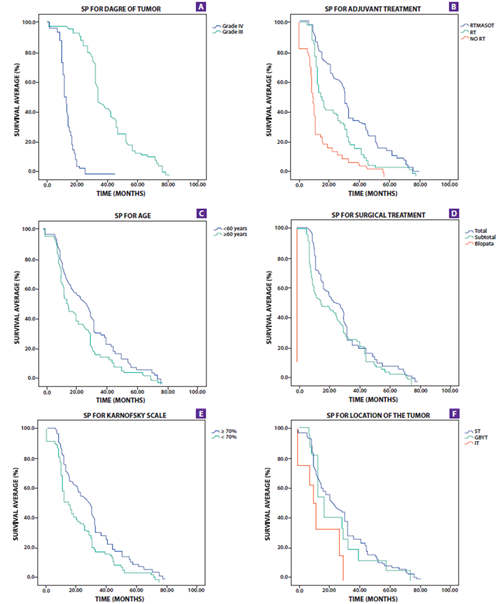
Tumor grade, Karnofsky scale, surgical treatment, age, and adjuvant treatment were significantly associated with the PS that can be seen inTable 2andFigure 1. The PS for the IV degree tumor was 15.7 months (95% CI 14.2-17.1) and for the III degree it was 38.4 months (95% CI 35.8-40.9); the patients under 60 years of age had a long PS of 32.6 months (P =0.015); for patients with a Karnofsky scale greater than 70%, they also presented 32.6 months of PS (95% CI 29.5-35.6); the patients with surgical treatment underwent total resection of the tumor, subtotal and biopsy, which had a PS of 30.8, 28.6 and 7.3 months, respectively; adjuvant radiotherapy/chemotherapy treatment had long PS (p <0.001). In the multivariate analysis, the tumor grade was the variable that had the highest correlation with PS (HR=1 5.5; p<0.001); while surgical treatment, age, adjuvant treatment, and karnofsky also correlated with PS (p=0 .07, p=0 .025, p=0.018, and p=0 .035 respectively)Table 4.
Table 3andFigure 2. show the SLP analysis. The SLP for the IV degree tumor was 11.3 months (95% CI 10.3-12.2) while for the III degree it was 32.8 months (95% CI 29.4-36.1); for the PS it was 15.7 months (95% CI: 14.2-17.1) and 38.4 months (95% CI 35.8-40.9) respectively. In univariate analysis, SLP varies significantly with tumor grade, surgical treatment, age, Karnofsky scale, and adjuvant treatment. Patients with a cut point at 60 years had a significant variation in PFS (p= 0.01).
The multivariate analysis shown inTable 4indicates that the tumor grade, surgical treatment, age, and adjuvant treatment were significantly correlated with PFS (p <0.001, p<0.001, p=0 .01 and p=0 .02 respectively) but no correlation was shown with the assessment of functional status (karnofsky scale).
Table 1. General characteristics of patients with high-grade glioma from the 2010-2014 period.
| Variable | n | % |
|---|---|---|
| Age | ||
| 14-30 | 35 | 12.6 |
| 31-60 | 150 | 54.0 |
| 61 and older | 93 | 33.5 |
| Mean | 49 | |
| Sex | ||
| Male | 136 | 48.9 |
| Female | 142 | 51.1 |
| Location of the Tumor | ||
| Supratentorial | ||
| Frontal | 58 | 20.9 |
| Parietal | 60 | 21.6 |
| Occipital | 10 | 3.6 |
| Temporal | 52 | 18.7 |
| More than 1 affected area | 72 | 25.9 |
| Thalamus and Basal ganglia | 18 | 6.5 |
| Infratentorial | ||
| Brain stem | 2 | 0.7 |
| Cerebellum | 6 | 1.7 |
| Karnofsky | ||
| ≥ 70 | 174 | 62.6 |
| <70 | 104 | 37.4 |
| Eloquent area | ||
| No | 213 | 76.6 |
| Yes | 65 | 23.4 |
| Tumor resection | ||
| Total | 179 | 64.4 |
| Subtotal | 87 | 31.3 |
| Biopsy | 12 | 4.3 |
| High-grade tumor | ||
| Grade IV | 144 | 51.8 |
| Grade III | 134 | 48.2 |
| Tumor diameter | ||
| <5 cm | 96 | 34.5 |
| ≥ 5 cm | 182 | 65.5 |
| Symptoms | ||
| Seizures | 84 | 30.2 |
| Headache | 192 | 69.1 |
| Hemiparesis | 85 | 30.6 |
| Aphasia | 50 | 18.0 |
| Dysarthria | 44 | 15.8 |
| IIH | 57 | 20.5 |
| Others | 52 | 18.7 |
| Adjuvant treatment | ||
| RT/QT | 162 | 58.3 |
| RT | 71 | 25.5 |
| NO RT | 45 | 16.2 |
Table 2. Median overall survival by a group of patients with high-grade glioma from the 2010-2014 period.
| Variable | Median (months) | 95% CI | p ** |
|---|---|---|---|
| Degree of Tumor | |||
| Grade IV | 15.7 | 14.2 - 17.1 | <0.001 |
| Grade III | 39.4 | 35.8 - 40.9 | |
| Gender | |||
| Male | 36.4 | 20.2 - 32.5 | 0.59 |
| Female | 30.8 | 24.1 - 37.4 | |
| Clinical Manifestations | |||
| Seizures | 32.1 | 26.8 - 37, 3 | 0.54 |
| IIH | 29.5 | 21.1 - 35.4 | 0.82 |
| Karnofsky | |||
| ≥ 70% | 32.6 | 39.5 - 35.6 | 0.005 |
| <70% | 21.4 | 13.0 - 37.8 | |
| Tumor Diameter | |||
| ≥ 5 cm | 24.7 | 17.3 - 32.0 | 0.54 |
| <5 cm | 30.8 | 26.1 - 35.4 | |
| Type of surgical treatment | |||
| Total | 30.8 | 25.0 - 36.5 | <0.001 |
| Subtotal | 20.60 | 18 , 2 - 38.9 | |
| Biopsy | 7.3 | 4.6 - 9.9 | |
| tumor | |||
| Supratentorial location | 29.6 | 24.6 - 34.5 | 0.56 |
| Basal ganglia and thalamus | 22.8 | 8.1 - 37.4 | |
| Infratentorial | 12 , 3 | 7.4 - 17.1 | |
| Age | |||
| <60 years | 32.6 | 29.2 - 35.9 | 0.015 |
| ≥ 60 years | 22.4 | 17.5 - 27.2 | |
| Eloquence | |||
| Yes | 32.8 | 27.4 - 38.1 | 0 , 43 |
| No | 26.4 | 21.3 - 31.4 | |
| Adjuvant Treatment | |||
| RT / QT | 32.9 | 30.1 - 35.6 | <0.001 |
| RT | 26.4 | 14.2 - 38.5 | |
| NO RT | 12.6 | 10.7 - 14.4 |
Table 3. Median progression-free survival by groups of patients with high-grade glioma for the period 2010-2014
| Variable | Median (months) | 95% CI | p ** |
|---|---|---|---|
| Degree of Tumor | |||
| Grade IV | 13.3 | 10.3 - 12.2 | <0.001 |
| Grade III | 32.8 | 29.4 - 36.1 | |
| Gender | |||
| Male | 20.4 | 12.2 - 29.5 | 0.61 |
| Female | 24.8 | 17.9 - 31.6 | |
| Clinical Manifestations | |||
| Seizures | 28.6 | 21.5 - 35.6 | 0.57 |
| IIH | 25.7 | 14.2 - 37.1 | 0.961 |
| Karnofsky | |||
| ≥ 70% | 29.7 | 25.1 - 34.2 | 0.045 |
| <70% | 14 , 6 | 9.9 - 19.2 | |
| Tumor Diameter | |||
| ≥ 5 cm | 20.8 | 14.1 - 27.5 | 0.62 |
| <5 cm | 27.9 | 21.7 - 34.0 | |
| Type of surgical treatment | |||
| Total | 28.3 | 25 , 0 - 36.5 | <0.001 |
| Subtotal | 20.4 | 8.9 - 31.8 | |
| Biopsy | - | - | |
| Tumor location | |||
| Supratentorial | 24.8 | 18.8 - 30.7 | 0.58 |
| Basal ganglia and thalamus | 20.4 | 14.5 - 25.7 | |
| Infratentorial | 10.0 | 5.4 - 14.5 | |
| Age | |||
| <60 years | 28.6 | 23.4 - 33.7 | 0.01 |
| ≥ 60 years | 15.4 | 9.5 - 21.2 | |
| Eloquence Area | |||
| Yes | 28.3 | 18 , 9 - 37.6 | 0.465 |
| No | 22.6 | 15.5 - 29.6 | |
| Adjuvant Treatment | |||
| RT/QT | 30.4 | 28.5 - 32.2 | <0.001 |
| RT | 14.9 | 11.1 - 18, 6 | |
| NO RT | 9 | 7.6 - 10.3 |
* * 95% CI: 95% confidence interval. RT: radiotherapy. RT / QT: a combination of radiotherapy and chemotherapy. No RT: No radiation therapy. IIH: Idiopathic intracranial hypertension ** P-value obtained through the Log Rank test
Table 4. Multivariate analysis with the COX proportional hazards ratio model for progression-free survival (SLP) and overall survival (PS).
| SLP | PS | |||||
|---|---|---|---|---|---|---|
| Variable | HR Adjusted | 95% CI | P ** | HR Adjusted | 95% CI | P ** |
| Tumor | ||||||
| Grade IV | Ref. | Ref. | ||||
| Grade III | 25.1 | 14.6 - 42.9 | <0.001 | 15.5 | 9.4 - 25.4 | <0, 01 |
| Surgical Treatment | ||||||
| Total | Ref. | Ref. | ||||
| Subtotal | 0.49 | 0.33 - 0.70 | <0.001 | 0.6 | 0.41 - 0.87 | 0.07 |
| Age | ||||||
| <60 years | Ref. | |||||
| ≥ 60 years | 1.7 | 1.23 - 2.44 | 0.02 | 1.47 | 1.4 - 2.07 | 0.025 |
| Adjuvant Treatment | ||||||
| RT / QT | Ref. | Ref. | ||||
| RT | 0.58 | 0.41 - 0.81 | 0.02 | 0.667 | 0.47 - 0.93 | 0.018 |
| Karnofsky | ||||||
| ≥ 70% | Ref. | Ref. | ||||
| <70% | 1.3 | 0.91 - 1.88 | 0.146 | 0.7 | 0.52 - 0.97 | 0.035 |
* 95% CI: 95% confidence interval. HR: Hazard Ratio. RT: radiotherapy. RT / QT: a combination of radiotherapy and chemotherapy. ** p-value obtained through the Log Rank test
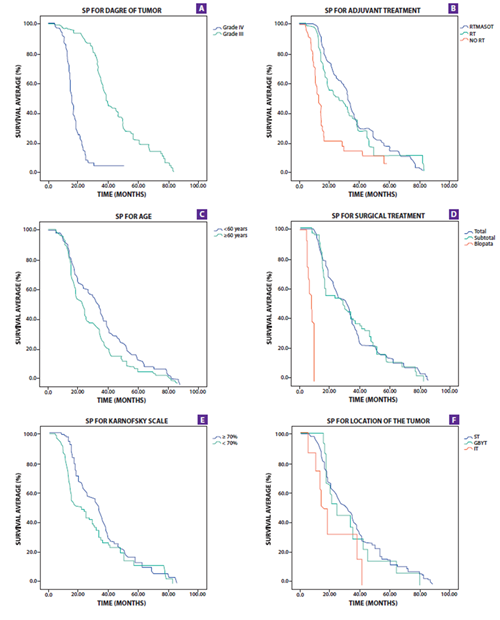
Figure 2. Survival charts showing overall survival (PS) by tumor grade (A), Adjuvant Treatment (B), age (C), Surgical Treatment (D), Karnosfsky (E) and Tumor location (F).
DISCUSSION
Glioblastoma multiforme (IV degree tumor) is the most aggressive primary neoplasm of the central nervous system. This neoplasm occurs mainly between 60 and 70 years old. In the present study, the median age of the patients was 51 years, which is consistent with the studies by McGirt and Liang.17,18with a median of 54 years. Furthermore, patients with a range greater than or equal to 60 years had lower average survival. Similar data were found in the studies by Yong-jian19and Lacroix for age ≥ 65 years20and lower progression-free survival .
Men represent the largest number of patients with high-grade glioma; however, in our study, there was no correlation with PS or SLP.8,19,21.
As the most frequent clinical manifestation in our study was a headache, followed by seizures and motor deficit13,22,23, however, none of them was related to patient survival; unlike Liang's study, in which he found an association in survival, by separating symptoms that do or do not belong to the picture of intracranial hypertension.
In our study, the Karnofsky scale (KFS) was used to assess the functional state of the patient, which was considered a good functional state at a KFS≥70, which was the most frequent and was correlated with better survival (median of 32, 6 months)24, other studies such as Lacroix and Chaichana reported similar results but with a KFS ≥8020,23. No association was found regarding PFS .
IV grade tumors, called glioblastoma multiforme, are the tumors with the shortest survival time, so in our study, the PS was 15.7 months, these are corroborated in the literature with many studies17,18,20,22-25and in terms of PFS was 11.3 months, similar to the results of Ahmadloo22in a series of 223 patients; III degree tumor, called anaplastic gliomas, the survival was 38.4 months and PFS was 32.8, similar findings to the Nuño study26; According to the data from our study, the grade of the tumor is a strong prognostic factor .
The location of the tumor is another of the variables that have been evaluated in our study, where tumors of the supratentorial location were the most frequent, and of these tumors that had more than 1 affected area, the parietal and frontal region were the most frequent. affected18, however, there was no correlation with the PS or the SLP22,23,27, unlike Kumar, who found an association between the location of the tumor (parietal lobe) and survival4. In our study we also evaluated the location of the tumor in an eloquent area, most of the tumors were not in these areas and there was also no correlation with PS and PFS, similar results exist in the literature20,23. Few studies take the variable diameter of the tumor with a cut point between 4 or 5 cm in diameter, our study used the latter, without finding a correlation19,22,24.
As for the treatment of tumors, the surgical option remains the choice for the management of this pathology, with total or near-total resection providing the best PS (median of 30.8 months) when compared to the subtotal (median of 20.6 months) or biopsy (median of 7 months) In addition, it forms a good prognostic factor23,24.similar to most studies; thus, it also influences PFS with a median of 28.3 and 20.4 for total and subtotal resection, respectively22,23.. Adjuvant treatment with radiotherapy and chemotherapy or a combination of these improves the average survival and PFS, as well as being a good prognostic factor22,23.; at this point in reference, it coincides with many of the published studies.
There are some limitations to the study to consider. First, the study population is only from a hospital, so extrapolating all these results to the population may not be completely recommended; however, since the hospital is a place where most cases arrive from all over the country, some inference can be made, and the results should not vary in the magnitude of the result. Then, we can consider Berkson's bias, which tells us about the impact of working with people enrolled in a hospital; But, as this is a single-arm study, looking only at the prognostic factors for high-grade glioma, its impact on the outcome should not be significant. .
CONCLUSION
According to the data in our study, age, functional status, surgical treatment, adjuvant treatment, and tumor grade are prognostic factors for overall survival in patients with high-grade glioma. In contrast to progression-free survival, prognostic factors were age, surgical treatment, adjuvant treatment, and tumor grade.
REFERENCES
1. Prabhu VC, Khaldi A, Barton KP, Melian E, Schneck MJ, Primeau MJ, et al. Management of diffuse low-grade cerebral gliomas. Neurol Clin. 2010;28(4):1037-59. DOI: https://doi.org/10.1016/j.ncl.2010.03.022 [ Links ]
2. Wen PY, Kesari S. Malignant gliomas in adults. N Engl J Med. 2008;359(5):492-507. DOI: 10.1056/NEJMra0708126 [ Links ]
3. Bradley D, Rees J. Updates in the management of high-grade glioma. J Neurol. 2014;261(4):651-4. DOI: https://doi.org/10.1007/s00415-013-7032-x [ Links ]
4. Kumar N, Kumar P, Angurana SL, Khosla D, Mukherjee KK, Aggarwal R, et al. Evaluation of outcome and prognostic factors in patients of glioblastoma multiforme: A single-institution experience. J Neurosci Rural Pract. 2013;4(Suppl 1):S46-55. DOI: 10.4103/0976-3147.116455 [ Links ]
5. Sanai N, Alvarez-Buylla A, Berger MS. Neural stem cells and the origin of gliomas. N Engl J Med. 2005;353(8):811-22. DOI: 10.1056/NEJMra043666 [ Links ]
6. Nazzaro JM, Neuwelt EA. The role of surgery in the management of supratentorial intermediate and high-grade astrocytomas in adults. J Neurosurg. 1990;73(3):331-44. DOI: https://doi.org/10.3171/jns.1990.73.3.0331 [ Links ]
7. Quigley MR, Maroon JC. The relationship between survival and the extent of the resection in patients with supratentorial malignant gliomas. Neurosurgery. 991;29(3):385-8. DOI: https://doi.org/10.1227/00006123-199109000-00008 [ Links ]
8. Markert JM. The role of early resection vs biopsy in the management of low-grade gliomas. JAMA. 2012;308(18):1918-9. DOI: 10.1001/jama.2012.14523 [ Links ]
9. Puiggròs C, Lecha M, Rodríguez T, Pérez-Portabella C, Planas M. El índice de Karnofsky como predictor de mortalidad en pacientes con nutrición enteral domiciliaria. Nutrición Hospitalaria. 2009;24(2):156-60. Available at: http://scielo.isciii.es/scielo.php?pid=S0212-16112009000200008&script=sci_arttext&tlng=en [ Links ]
10. Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, Burger PC, Jouvet A, et al. The 2007 WHO Classification of Tumours of the Central Nervous System. Acta Neuropathol. 2007;114(2):97-109. DOI: https://dx.doi.org/10.1007%2Fs00401-007-0243-4 [ Links ]
11. Stewart LA. Chemotherapy in adult high-grade glioma: a systematic review and meta-analysis of individual patient data from 12 randomised trials. Lancet. 2002;359(9311):1011-8. DOI: https://doi.org/10.1016/S0140-6736(02)08091-1 [ Links ]
12. Walker MD, Green SB, Byar DP, Alexander E, Batzdorf U, Brooks WH, et al. Randomized comparisons of radiotherapy and nitrosoureas for the treatment of malignant glioma after surgery. N Engl J Med. 1980;303(23):1323-9. DOI: 10.1056/NEJM198012043032303 [ Links ]
13. Nitta T, Sato K. Prognostic implications of the extent of surgical resection in patients with intracranial malignant gliomas. Cancer. 1995;75(11):2727-31. DOI: https://doi.org/10.1002/1097-0142(19950601)75:11%3C2727::AID-CNCR2820751115%3E3.0.CO;2-H [ Links ]
14. Hess KR. Extent of resection as a prognostic variable in the treatment of gliomas. J Neurooncol. 1999;42(3):227-31. DOI: https://doi.org/10.1023/A:1006118018770 [ Links ]
15. van Rijn J, Heimans JJ, van den Berg J, van der Valk P, Slotman BJ. Survival of human glioma cells treated with various combinations of temozolomide and X-rays. Int J Radiat Oncol Biol Phys. 2000;47(3):779-84. DOI: https://doi.org/10.1016/S0360-3016(99)00539-8 [ Links ]
16. Bauman GS, Gaspar LE, Fisher BJ, Halperin EC, Macdonald DR, Cairncross JG. A prospective study of short-course radiotherapy in poor prognosis glioblastoma multiforme. Int J Radiat Oncol Biol Phys. 1994;29(4):835-9. DOI: https://doi.org/10.1016/0360-3016(94)90573-8 [ Links ]
17. McGirt MJ, Mukherjee D, Chaichana KL, Than KD, Weingart JD, Quinones-Hinojosa A. Association of surgically acquired motor and language deficits on overall survival after resection of glioblastoma multiforme. Neurosurgery. septiembre de 2009;65(3):463-9; discussion 469-470. DOI: https://doi.org/10.1227/01.NEU.0000349763.42238.E9 [ Links ]
18. Liang H-K, Wang C-W, Tseng H-M, Huang C-Y, Lan K-H, Chen Y-H, et al. Preoperative prognostic neurologic index for glioblastoma patients receiving tumor resection. Ann Surg Oncol. noviembre de 2014;21(12):3992-8. DOI: https://doi.org/10.1245/s10434-014-3793-4 [ Links ]
19. Zhu Y, Zhu X, Wang S, Shen F, Shen H, Liu W. A multivariate analysis of the prognostic factors of grade III gliomas. Chin Med J. 2008;121(12):1072-5. Available at: https://insights.ovid.com/pubmed?pmid=18706219 [ Links ]
20. Lacroix M, Abi-Said D, Fourney DR, Gokaslan ZL, Shi W, DeMonte F, et al. A multivariate analysis of 416 patients with glioblastoma multiforme: prognosis, extent of resection, and survival. J Neurosurg. 2001;95(2):190-8. DOI: https://doi.org/10.3171/jns.2001.95.2.0190 [ Links ]
21. Lovatón Espadín, Rolando Eladio. Sobrevida asociada a la resección quirúrgica de los gliomas de alto grado operados en el Departamento de Neurocirugía del Hospital Edgardo Rebagliati Martins en el periodo 2011-2012 [Bachelor Thesis]. [Lima]: Facultad de Medicina. Escuela de postgrado UNMSM; 2014. Available at: https://docplayer.es/15800822-Universidad-nacional-mayor-de-san-marcos.html [ Links ]
22. Ahmadloo N, Kani A-A, Mohammadianpanah M, Nasrolahi H, Omidvari S, Mosalaei A, et al. Treatment outcome and prognostic factors of adult glioblastoma multiforme. J Egypt Natl Canc Inst. marzo de 2013;25(1):21-30. DOI: https://doi.org/10.1016/j.jnci.2012.11.001 [ Links ]
23. Chaichana K, Parker S, Olivi A, Quiñones-Hinojosa A. A proposed classification system that projects outcomes based on preoperative variables for adult patients with glioblastoma multiforme. J Neurosurg. 2010;112(5):997-1004. DOI: https://doi.org/10.3171/2009.9.JNS09805 [ Links ]
24. Laws ER, Parney IF, Huang W, Anderson F, Morris AM, Asher A, et al. Survival following surgery and prognostic factors for recently diagnosed malignant glioma: data from the Glioma Outcomes Project. J Neurosurg. 2003;99(3):467-73. DOI: https://doi.org/10.3171/2009.9.JNS09805 [ Links ]
25. Lamborn KR, Chang SM, Prados MD. Prognostic factors for survival of patients with glioblastoma: recursive partitioning analysis. Neuro-oncology. 2004;6(3):227-35. DOI: https://doi.org/10.1215/S1152851703000620 [ Links ]
26. Nuño M, Birch K, Mukherjee D, Sarmiento JM, Black KL, Patil CG. Survival and prognostic factors of anaplastic gliomas. Neurosurgery. 2013;73(3):458-65; quiz 465. DOI: https://doi.org/10.1227/01.neu.0000431477.02408.5e [ Links ]
27. Akman F, Cooper RA, Sen M, Tanriver Y, Kentli S. Validation of the Medical Research Council and a newly developed prognostic index in patients with malignant glioma: how useful are prognostic indices in routine clinical practice? J Neurooncol. 2002;59(1):39-47. DOI: https://doi.org/10.1023/A:1016353614525 [ Links ]
Received: June 26, 2020; Accepted: July 12, 2020











 text in
text in