Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista de la Facultad de Medicina Humana
Print version ISSN 1814-5469On-line version ISSN 2308-0531
Rev. Fac. Med. Hum. vol.21 no.2 Lima Apr-Jun 2021
http://dx.doi.org/10.25176/rfmh.v21i2.3608
Original article
Work conditions and personal protective equipment against Covid-19 in health personnel, Lima-Peru
1Miembro de European Association of Science Editors; Universidad Nacional Hermilio Valdizán, Lima-Perú.
2Facultad de Enfermería; Universidad Nacional del Callao-Perú.
3Facultad de Medicina Humana; Universidad Nacional Mayor de San Marcos-Perú.
4Facultad de Enfermería; Universidad Norbert Wiener, Lima-Perú.
Objective:
To determine the association between working conditions and access to personal protective equipment (PPE) in health personnel in the city of Lima-Perú.
Methods:
Descriptive, cross-sectional and analytical study. The sample was of 271 respondents virtually in the city of Lima, who met the selection criteria, captured between 07/09/2020 to 08/09/2020. The data collection instrument was validated by expert judgment with a score> 80% (content validity). An analysis was carried out with the generalized linear model of the Poisson family, log link function, robust models with fit. A statistically significant value of p <0.05 was considered.
Results:
The 55% of health personnel (HCP) worked more than 12 hours and only 53% received one PPE per day of work. 40% of the HCP almost never received a mask. In the multivariate analysis, the SP with ages <26 years (p=0.00) and from 26 to 55 years (p=0.00) received an incomplete PPE. The HCPs who did not have an employment relationship with the institution (p=0.02) received a mask on few occasions.
Conclusion:
Health personnel under the age of 56 rarely received PPE. When they work without an employment relationship, they sometimes receive a mask.
Key words: protective equipment; COVID-19; Health personnel; Organization at work and occupational health (Source: DeCS BIREME).
INTRODUCTION
SARS-CoV-2 (COVID-19) spread worldwide, being classified as a pandemic by the World Health Organization (WHO) in March 2020 and until that date no effective drugs or vaccines are available to combat it. Cases of COVID-19 continue to increase, especially in the American continent, which has increased the need for frontline health professionals in both public and private institutions, even working long hours.1,2Because of these frontline health workers have a high risk of infection, this contributes to a greater spread of the disease,3,4representing up to 20% of COVID-19 cases in a country.5The proper use of N95 or similar masks can reduce the possibility of contracting COVID-19 by 64% to 75%.6Peru is no stranger to this reality and is one of the main countries with more cases of COVID-19 according to reports from Johns Hopkins University.7
The Centers for Disease Control and Prevention (CDC) and WHO recommend non-pharmacological measures such as: hygiene, disinfection, early detection and use of personal protective equipment (PPE) such as non-sterile and sterile gloves, N95 / PPF2 mask, face protector, protective goggles, disposable aprons, disposable clothing, among others.8-10However, there was a worldwide shortage of PPE, especially masks, due to the high demand from health institutions and the population, in addition to the interruption of the supply chain of medical supplies.(9,11)due to this great need, health professionals reuse11and even refurbish an PPE of materials not recommended for safe protection,12putting their health at risk. The risk of infection increases when the worker works in the Intensive Care Unit (ICU) area, or COVID-19 wards, especially when the hospital does not have an efficient system of air replacements. As a result, the health professional may contract COVID-19 disease and need to be hospitalized, even use mechanical ventilation in the ICU or lose his life, figures that increased as the problem of access to PPE worsened.15
In hospitals, biosafety measures must be strict. These guidelines suggest a mandatory minimum ratio of personal protective equipment according to the level of risk, previously assessed by the occupational health and safety area, which suggests the type of PPE according to the occupational risk.8,16there is poor implementation of occupational safety and health policies, especially in the health systems of developing countries. And they have weak health systems.17,18
The organisms that watch over occupational health recommend that access to PPE should be ensured, improving working conditions integrated with the prevention measures established in the organizational plans against COVID-19.8,16,19
Therefore, the study aimed to determine the association between working conditions and access to PPE for health personnel in the city of Lima-Perú.
METHODS
Design and study area
The study design was: descriptive, cross-sectional and analytical. He was executed between July 9 and August 9, 2020. A survey was conducted of the health personnel of the city of Lima.
Population and sample
Virtually a survey was sent to 753 people ≥ 18 years of age, through social networks in order to reach all the different reference hospitals in the city of Lima, which were distributed in the districts of: Villa el Salvador, La Victoria, Ate, San Martin de Porras, Breña, el Agustino, Lince, Miraflores, Independencia, San Juan de Lurigancho and Callao. Of which 553 were answered by health personnel, 230 did not meet the selection criteria (surveys of people who did not want to participate in the study, those under 18 years of age, health personnel who did not work directly with patients diagnosed with COVID-19, foreigners, primary care, from other cities, inconsistent or partial answers), so that in the end only 271 surveys remained.
The sample was not random, it had a snowball sampling, so the participants shared the link of the virtual survey to their health contacts (friends, family or coworkers), through social networks such as "Facebook, Telegram and WhatsApp".
To estimate the association between working conditions and access to personal protective equipment, the theoretical bases were reviewed and a virtual survey was constructed. The first version of the survey contained 24 questions, with dichotomous, polytomous, multiple choice or data-filling alternatives.
Variables and tools
The main variables of the study were: PPE access; receives mask, age, employment relationship, area of work, occupational group, working hours and years on the workplace.
The survey was validated by 13 experts (physicians, nurses, pharmaceutical chemist, nutritionist, medical technologist, health professional, Occupational Medicine and Health Management) with which it reached a score of over 80% in content validity. Subsequently, a pilot study of the virtual survey was conducted with 36 people to improve internal validity, with the results obtained 8 questions were removed and only 17 remained. The survey had the following parts: the first were sociodemographic data consisting of 4 questions on (age, gender, city of residence and occupation); The second part corresponded to working conditions which had 6 questions (type of contract, institution where you work, level of attention of the workplace, profession, area of the hospital where you work, hours of work per shift and years of work experience); The third part asked about personal protective equipment with 4 questions (types of PPE you received from your employer, if you received a complete/incomplete PPE, how many days you were given an PPE and how many days you were given an N95 mask) and the fourth part contained questions that were used to apply the selection or adjustment criteria of the statistical analysis (works directly with a patient diagnosed with COVID-19, at your workplace perform screening for COVID-19 and you were diagnosed with COVID-19).
Procedures
Due to the context of the current pandemic, a virtual survey was conducted using a Google Drive sheet. The questions validated by expert judgment were appropriate in the Google Drive form and subsequently a pilot study was conducted. The message sent by social networks "Facebook, Telegram and WhatsApp" contained a brief description of: the purpose of the study, that the survey would be anonymous and the indication if you wanted to participate in the study "click on link of the virtual survey". When entering the survey, a message would appear "whether or not I wanted to be part of the study," if they marked "no" the survey ended and if they marked "yes" they continued with the development of the questions. In order to obtain the largest number of respondents, the link was shared to one or more health workers from the districts of Lima Norte, Centro, Este, Sur and Callao. Also influential people contributed in sharing and recommending that the link is not a virus. The Google Drive program stored all the answers in real time in an Excel format, then worked with the database according to the selection criteria, for the second time the information was corroborated to rule out any error, then coded the variables according to the objectives of the study and finally exported the data to the statistical program SPSS version 24.
Ethical aspects
The ethical principles in research according to the Helsinki Norms were respected, participation was voluntary, anonymous and the data were treated confidentially.
Statistical analysis
A descriptive and analytical study was carried out according to the objectives of the study. For the descriptive analysis we used percentages and frequencies for polytomous variables. Tables and graphs were also created according to the type of variable. With the Kolmogórov-Smirnov test, we determined that the sample did not have a normal distribution (p=0.00).
In the first analysis, chi-square was used for categorical variables. Next, multivariate analysis was performed with generalized linear models with Poisson family, log link function and robust models. This was adjusted for gender and COVID-19 diagnosis. A statistically significant value of p<0.05 and a confidence interval of 95% was considered.
RESULTS
Of all health personnel, 271 met the selection criteria. The female population was more representative (71%) in the study. The mean age of the total participants was 42 (+10.10 years), with an age range from 21 to 70 years.
The age group with the largest population was 31 to 45 years, followed by 46 to 55 years. The majority of the male gender worked as physician; the majority of the female gender were nurses. (Table 1)
Table 1. Occupational group according to age group and gender in health personnel.
| Occupational group | N | % | Age group (years) | Gender | |||||
|---|---|---|---|---|---|---|---|---|---|
| < 31 | 31 a 45 | 46 a 55 | 56 a 64 | > 64 | M | F | |||
| Medical specialist | 29,2 | 2 | 40 | 26 | 8 | 3 | 43 | 36 | |
| Resident physician | 32 | 11,8 | 15 | 15 | 2 | 0 | 0 | 14 | 18 |
| General physician | 9 | 3,3 | 1 | 6 | 2 | 0 | 0 | 2 | 7 |
| Nurse practitioner | 60 | 22,1 | 1 | 25 | 21 | 13 | 0 | 2 | 58 |
| General nurse | 46 | 17,0 | 11 | 28 | 6 | 1 | 0 | 7 | 39 |
| Laboratory personnel | 11 | 4,1 | 4 | 3 | 4 | 0 | 0 | 4 | 7 |
| Other health professions | 18 | 6,6 | 1 | 7 | 4 | 6 | 0 | 4 | 14 |
Source: Number of respondents =n., M= male, F= Female. *ACS = Administrative Contract of Services.
Multivariate analysis found that the health professional who belonged to the age group <26 years was more likely to receive an incomplete PPE (PR: 25.3; 95%CI: 23.9-26.7, p value=0.00), compared to workers aged 56 to 64; Similarly, the age group of 26 to 55 years received more frequently an incomplete PPE (PR: 24.8; 95%CI: 24.1-25.5, p value= 0.00), compared to workers aged 56 to 64; In both age groups the statistical model was adjusted for: type of contract, level of the workplace, area of work, profession, hours of work per shift, years of work experience, gender and the reference on the COVID-19 diagnosis. The health professional who did not have a contract (temporary without employment) received a mask less frequently (RP: 0.75; 95%CI: 0.14-0.9, p value= 0.02), compared to those who had permanent employment; This crossover was adjusted for age group, workplace level, area of work, profession, working hours per shift, years of work experience, gender, and COVID-19 diagnostic reference. The provision of incomplete PPE or not receiving a mask per work shift had no association with workplace level, occupation, hours of work per shift, and years on the workplace. (Table 2)
Table 2. Multivariate analysis of the factors associated with receiving incomplete PPE and not receiving a mask in the health professional.
| n | % | Receives a PPE incomplete | RP | 95% IC | P | Receives mask | RP | 95% CI | P | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| YES | NO | NO | YES | ||||||||||||||
| Age | |||||||||||||||||
| <26 years | 5 | 1.8 | 2 | 3 | 25.3 | 23.9 -26.7 | O,OO | 4 | 1 | not significant | |||||||
| 26 to 55 years | 235 | 86.7 | 156 | 79 | 24.8 | 24.1 -25.5 | O,OO | 142 | 93 | not significant | |||||||
| 56 to 64 years | 28 | 10.3 | 18 | 10 | Reference | 19 | 9 | Reference | |||||||||
| >64 years | 3 | 1.1 | 3 | 0 | NA | 2 | 1 | NA | |||||||||
| Employment relationship | |||||||||||||||||
| Permanent (appointed) | 87 | 32.1 | 60 | 27 | not significant | 56 | 31 | not significant | |||||||||
| Temporary direct link* | 51 | 18.8 | 34 | 17 | not significant | 34 | 17 | not significant | |||||||||
| Temporary indirect link** | 21 | 7.7 | 14 | 7 | not significant | 8 | 13 | 0.75 | 0.14 - 0.9 | 0.02 | |||||||
| Temporary no link | 112 | 41.3 | 71 | 41 | Reference | 69 | 43 | Reference | |||||||||
| Area of work | |||||||||||||||||
| Physician’s office o topic | 17 | 6.3 | 17 | 0 | NA | 8 | 9 | Reference | |||||||||
| Diagnostic imaging | 13 | 4.8 | 12 | 1 | not significant | 5 | 8 | not significant | |||||||||
| Emergency | 68 | 25.1 | 45 | 23 | not significant | 45 | 23 | not significant | |||||||||
| Hospitalization | 70 | 25.8 | 46 | 24 | Reference | 38 | 32 | not significant | |||||||||
| Clinical Laboratory | 9 | 3.3 | 5 | 4 | not significant | 6 | 3 | not significant | |||||||||
| Clinical Pathology | 6 | 2.2 | 6 | 0 | NA | 2 | 4 | not significant | |||||||||
| ICU | 32 | 11.8 | 16 | 16 | not significant | 25 | 7 | not significant | |||||||||
| Low exposure to COVID-19& | 56 | 20.7 | 32 | 24 | NA | 38 | 18 | not significant | |||||||||
| Occupational group | |||||||||||||||||
| Medical specialist | 79 | 29.2 | 52 | 27 | not significant | 53 | 26 | not significant | |||||||||
| Resident physician | 9 | 3.3 | 7 | 2 | not significant | 6 | 3 | not significant | |||||||||
| General physician | 32 | 11.8 | 29 | 3 | not significant | 16 | 16 | not significant | |||||||||
| Practitioner nurse | 60 | 22.1 | 35 | 25 | not significant | 35 | 25 | not significant | |||||||||
| General nurse | 46 | 17.0 | 25 | 21 | not significant | 31 | 15 | not significant | |||||||||
| Laboratory personnel | 11 | 4.1 | 7 | 4 | Reference | 5 | 6 | Reference | |||||||||
| Nursing Technician | 16 | 5.9 | 13 | 3 | not significant | 11 | 5 | not significant | |||||||||
| Other health professions | 18 | 6.6 | 11 | 7 | not significant | 10 | 8 | not significant | |||||||||
| Hours worked per shift | |||||||||||||||||
| 6 hours | 52 | 19.2 | 29 | 23 | not significant | 39 | 13 | not significant | |||||||||
| 8 hours | 18 | 6.6 | 9 | 9 | not significant | 12 | 6 | not significant | |||||||||
| 12 hours | 149 | 55.0 | 87 | 62 | not significant | 100 | 49 | not significant | |||||||||
| 24 hours | 52 | 19.2 | 42 | 10 | Reference | 28 | 24 | Reference | |||||||||
| Years on the workplace | |||||||||||||||||
| <1 year | 11 | 41 | 5 | 6 | not significant | 10 | 1 | not significant | |||||||||
| 2 to 5 years | 63 | 23,2 | 40 | 23 | not significant | 36 | 27 | not significant | |||||||||
| 6 to 10 years | 50 | 18,5 | 39 | 11 | not significant | 33 | 17 | not significant | |||||||||
| 11 to 29 years | 127 | 46,9 | 80 | 47 | not significant | 75 | 52 | not significant | |||||||||
| >30 years | 20 | 7,4 | 15 | 5 | Reference | 13 | 7 | Reference | |||||||||
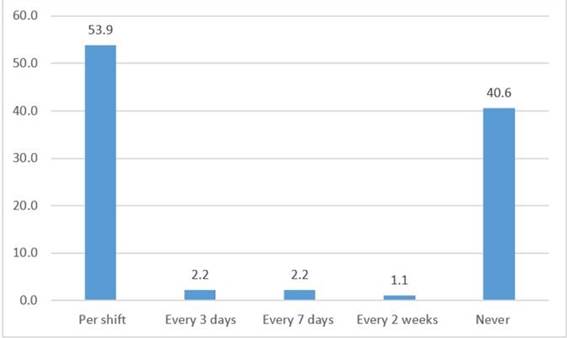
53.9% of the study population reported that they receive their PPE for each work shift, 40.6% reported that they never received PPE for the care of patients with COVID-19. (Figure 1)
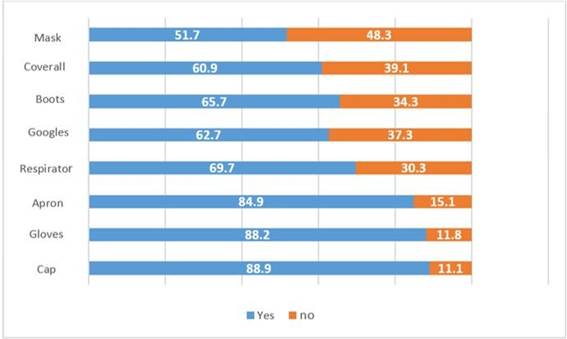
The study population reports that the PPE they receive most from their employer are: cap (88.9%), gloves (88.2%) and apron (84.9%). (Figure 2)
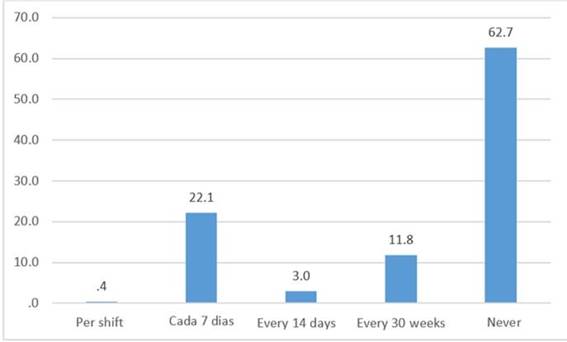
62.7% of health personnel reported that they were never given an N95 mask and only 0.5% received one N95 mask per shift. (Figure 3)
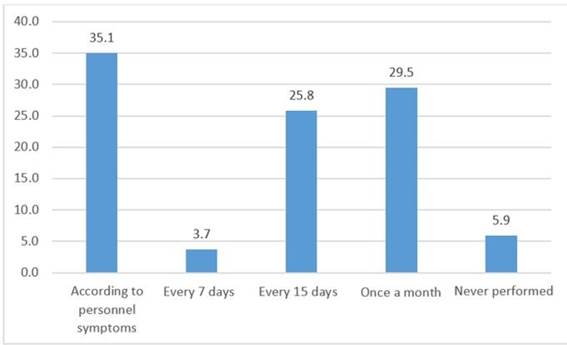
Health personnel reported that they usually take at least one rapid test if: they present symptoms of COVID-19 (35.1%), monthly control (29.5%), every 15 days (25.8%) and some never take them (5.9%). (Figure 4)
DISCUSION
In our study, 55% of the health personnel reported having received personal protective equipment (PPE) for each work shift. Lack of PPE provision may be due to pandemic shortages and high demand at different levels of health care globally.9,12Another explanation is the interruption in the supply chain of medical supplies, insufficient production to meet market demand for PPE in Peru.
It has been reported that when the PPE is reduced, health personnel purchase their own personal protective equipment, reuse or adapt with other materials not certified for such work, thereby increasing the risk of contracting the SARS-CoV-2 virus.(12)This scenario would explain why frontline health personnel can represent from 10% to 20% of all infected cases by this disease in a country.5
Our results coincide with a study in Latin America, where health professionals had limited access to PPE such as: face protector, mask, disposable gown, and among others.2This despite the WHO recommended personal protection equipment as a priority to work in COVID-19 patient care.
Health personnel also carry out activities outside the hospital, such as: home visits, evaluation to determine epidemiological maps, etc.; Transit through these places does not guarantee compliance with the administrative and security controls that are implemented in hospitals, especially in a pandemic.20For the above reasons, health personnel are a vulnerable population in this pandemic; providing personal protective equipment is an obligation of the employer, whether state or private, thereby reducing the risk of contracting the disease, with the consequent reduction of staff insecurity to provide care to a suspected or confirmed COVID-19 patient.21
Our study reports that incomplete personal protective equipment was given to health personnel under 56 years of age; this finding may explain why priority was given to the delivery of complete PPE to health personnel at greater risk of vulnerability when contracting COVID-19, also health personnel ≥ 56 years (11%) were working in different institutions. One study found that among hospitalized health professionals who died of COVID-19, mortality doubled between the ages of 50 and 59, quadrupled between the ages of 60 and 69, and was 12 times higher after age 70 compared with younger patients.3
The risk of contracting COVID-19 has been exacerbated by inadequate provision of personal protective equipment.22This information is consistent with another epidemic of severe acute respiratory syndrome (SARS), where inadequate PPE use was associated with increased risk of the disease.23
In the study, half of the health personnel worked more than 12 hours per shift caring for patients diagnosed with COVID-19. The extension of working hours may be due to cover shifts of staff in quarantine due to COVID-19, staff shortages due to high demand and comorbidity leave. All this added to a lack of a ventilation system with air exchange, which can increase the risk of contracting COVID-19, since it is known that the virus is transmitted by air.4,14Studies have clearly shown that the severity of COVID-19 is directly proportional to the viral load in the airways.14This explains why there are a large number of physicians infected and killed by COVID-19 in Peru, in the different services, such as the intensive care unit, hospitalization and others.15Here the importance of caring for health personnel and providing them with the necessary PPE.24
In addition, there are studies showing that long working hours affect health, suggesting an increased risk of cardiovascular disease and cancer.24,25In addition, excessively long working hours (> 12 hours) also deteriorate the mental health status of workers, generating symptoms of anxiety, depression, and sleep disorders.26A study in China showed that, during the COVID-19 outbreak, sleep disturbance was highly prevalent in health professionals.27
50.9% of respondents reported that they were almost never given an N95 respirator per shift. These results can be explained by the growing need to have a greater number of N95 respirators, the high demand for respirators at different levels of the health sector, the increase in the purchase by the population triggered the shortage of this medical input,9,12to this was added the increase in prices of up to ten times its usual value by suppliers, leading to a restricted and high cost good. Our results coincide with the study carried out on health professionals in Latin America, where only 56% of the health professionals who attended patients diagnosed with COVID-19, had access to N95 respirators, the hospital filled this gap by assigning surgical masks to its workers.2Surgical masks are not recommended as respiratory protection for jobs with high exposure to COVID-19.28It is evident that the FFP2 respirator, followed by the N95 respirator meet the requirements for filtration of small airborne particles, another advantage of these respirators is the tight fit to the user's face being more effective than surgical masks in reducing exposure to COVID-19.13,28,29In a study conducted on N95 respirators, their use showed efficient blocking against SARS-CoV-2 virus particles.30Therefore in health professionals, respirators such as FPP2 or N95 are very necessary to use them for adequate protection against this disease, without leaving aside frequent hand washing.31
The results of the study show that neither the profession nor the area where health personnel work has a difference in access to PPE. This could be explained due to the shortage of personal protective equipment in the global context caused by the pandemic.9,10At least the purchase of N95 respirators should be prioritized for health personnel working in areas of higher risk of exposure to COVID-19,(3,14)since the main route of transmission of this disease is the air and the N95 respirator has been shown to reduce the rate of infection by COVID-19.6A study described the levels of risk in health professionals who worked with COVID-19 patients, the areas of high exposure to this disease were: hospitalization and internal medicine, even reaching a higher average of this disease when compared to other areas or hospital services, especially nurses, followed by physicians.32
Our results show that about half of the health professionals (41%) did not have an employment contract and this group was assigned sometimes N95 respirator. This would be explained by the abrupt demand for jobs to cover the growing need to care for COVID-19 patients, labor informality increased in the health sector. This problem of informal employment leads to inequalities and inequity. Currently, the Peruvian state does not have the necessary logistics system to monitor compliance with labor laws, and many companies take advantage of this situation.33
Our study agrees with the results of research conducted on health professionals that included Hispanics, Asians and ethnic minorities, they did not have adequate PPE despite working in the area of COVID-19 patient care; They even report that 23% of the health personnel reported that they reused the PPE.34In addition, they had much lower wages compared to workers with a formal contract.35
As described above, the incipient development of occupational health areas in hospitals is still an Achilles’ heel in Peru and other Latin American countries.15,18In the context of the pandemic in Peru, the Ministry of Health published a regulation (Ministerial Resolution N° 448 - MINSA), focused on guidelines for the surveillance, prevention and control of workers' health in the context of COVID-19, It describes a worker's risk factors against COVID-19, based on age and comorbidities. As well as using PPE according to the level of risk of exposure to COVID-19 at the workplace. Health personnel are classified as medium and high risk of exposure to COVID-19.16The ILO, WHO and CDC also recommend that health professionals should use an appropriate PPE, since the risk of exposure to SARS-CoV-2 is frequent during routine tasks performed.8,10,36With published evidence in the world and standards in Peru, the occupational health areas of hospitals have the duty to implement occupational health policies to reduce the morbidity and mortality of this pandemic among health professionals. Prevention and promotion of health in the workplace improves productivity, reduces absenteeism due to illness, strengthens safety and improves job satisfaction.
Regarding the limitations of this research, we found only one multicenter study in Latin America on the use of personal protective equipment, but it does not specify information about Peru. In this study, most of the health personnel who responded to the survey were women from different health areas; however, in the multivariate analysis, the statistical adjustment was made.
The sample size does not represent the population of the city of Lima (Peru) even though there were respondents from different districts of the city, so it cannot be extrapolated to the entire population of Lima.
The information generated by the virtual survey to carry out the research is considered as a self-report, which could suffer from a bias.
It is recommended for future research to carry out studies on the effectiveness of the use of PPE in reducing the number of people infected by COVID-19 in health workers according to hospital level.
CONCLUSION
Young health personnel and those under 56 years of age infrequently received full personal protective equipment. Health personnel without a work contract less frequently received an N95 mask. Finally, only half of the health personnel reported receiving personal protective equipment for each work shift.
REFERENCES
1. Cheng VCC, Wong S-C, Chen JHK, Yip CCY, Chuang VWM, Tsang OTY, et al. Escalating infection control response to the rapidly evolving epidemiology of the coronavirus disease 2019 (COVID-19) due to SARS-CoV-2 in Hong Kong. Infect Control Hosp Epidemiol. 2020;41(5):493-8. Disponible en: https://pubmed.ncbi.nlm.nih.gov/32131908/ [ Links ]
2. Delgado D, Wyss Quintana F, Perez G, Sosa Liprandi A, Ponte-Negretti C, Mendoza I, et al. Personal Safety during the COVID-19 Pandemic: Realities and Perspectives of Healthcare Workers in Latin America. Int J Environ Res Public Health. 18 de 2020;17(8). Disponible en: https://pubmed.ncbi.nlm.nih.gov/32325718/ [ Links ]
3. Jankowski J, Davies A, English P, Friedman E, McKeown H, Rao M, et al. Risk Stratification tool for Healthcare workers during the CoViD-19 Pandemic; using published data on demographics, co-morbid disease and clinical domain in order to assign biological risk. medRxiv (Internet). 15 de junio de 2020 (citado 17 de septiembre de 2020);2020.05.05.20091967. Disponible en: https://www.medrxiv.org/content/10.1101/2020.05.05.20091967v3 [ Links ]
4. Morawska L, Cao J. Airborne transmission of SARS-CoV-2: The world should face the reality. Environment International (Internet). 1 de junio de 2020 (citado 17 de septiembre de 2020);139:105730. Disponible en: http://www.sciencedirect.com/science/article/pii/S016041202031254X [ Links ]
5. Lazzerini M, Putoto G. COVID-19 in Italy: momentous decisions and many uncertainties. The Lancet Global Health (Internet). 1 de mayo de 2020 (citado 16 de septiembre de 2020);8(5):e641-2. Disponible en: https://www.thelancet.com/journals/langlo/article/PIIS2214-109X(20)30110-8/abstract [ Links ]
6. Chu DK, Akl EA, Duda S, Solo K, Yaacoub S, Schünemann HJ, et al. Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis. The Lancet (Internet). 27 de junio de 2020 (citado 4 de febrero de 2021);395(10242):1973-87. Disponible en: https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)31142-9/abstract [ Links ]
7. Universidad Johns Hopkins. Coronavirus COVID-19 Global Cases by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University (JHU) (Internet). 2021 (citado 4 de febrero de 2021). Disponible en: https://gisanddata.maps.arcgis.com/apps/opsdashboard/index.html#/bda7594740fd40299423467b48e9ecf6 [ Links ]
8. World Health Organization. Coronavirus disease (COVID-19) outbreak: rights,roles and responsibilities of health workers, including key considerations for occupational safety and health (Internet). 2020 (citado 17 de septiembre de 2020). Disponible en: https://www.who.int/publications-detail-redirect/coronavirus-disease-(covid-19)-outbreak-rights-roles-and-responsibilities-of-health-workers-including-key-considerations-for-occupational-safety-and-health [ Links ]
9. Livingston E, Desai A, Berkwits M. Sourcing Personal Protective Equipment During the COVID-19 Pandemic. JAMA (Internet). 19 de mayo de 2020 (citado 16 de septiembre de 2020);323(19):1912-4. Disponible en: https://jamanetwork.com/journals/jama/fullarticle/2764031 [ Links ]
10. United States Department of Labour. Safety and Health Topics | COVID-19 | Occupational Safety and Health Administration (Internet). 2020 (citado 17 de septiembre de 2020). Disponible en: https://www.osha.gov/SLTC/covid-19/index.html [ Links ]
11. Schwartz A, Stiegel M, Greeson N, Vogel A, Thomann W, Brown M, et al. Decontamination and Reuse of N95 Respirators with Hydrogen Peroxide Vapor to Address Worldwide Personal Protective Equipment Shortages During the SARS-CoV-2 (COVID-19) Pandemic. Appl Biosaf (Internet). 1 de junio de 2020 (citado 16 de septiembre de 2020);25(2):67-70. Disponible en: https://doi.org/10.1177/1535676020919932 [ Links ]
12. Maguiña Vargas C, Maguiña Vargas C. Reflexiones sobre el COVID-19, el Colegio Médico del Perú y la Salud Pública. Acta Médica Peruana (Internet). enero de 2020 (citado 16 de septiembre de 2020);37(1):8-10. Disponible en: http://www.scielo.org.pe/scielo.php?script=sci_abstract&pid=S1728-59172020000100008&lng=es&nrm=iso&tlng=es [ Links ]
13. Klompas M, Baker MA, Rhee C. Airborne Transmission of SARS-CoV-2: Theoretical Considerations and Available Evidence. JAMA (Internet). 4 de agosto de 2020 (citado 17 de septiembre de 2020);324(5):441-2. Disponible en: https://jamanetwork.com/journals/jama/fullarticle/2768396 [ Links ]
14. Aggarwal S, Aggarwal S, Aggarwal A, Jain K, Minhas S. Alta carga viral y mala ventilación: causa de alta mortalidad por COVID-19. Asia Pac J Public Health (Internet). 25 de julio de 2020 (citado 17 de septiembre de 2020);1010539520944725. Disponible en: https://doi.org/10.1177/1010539520944725 [ Links ]
15. Galán-Rodas E, Tarazona-Fernández A, Palacios-Celi M, Galán-Rodas E, Tarazona-Fernández A, Palacios-Celi M. Riesgo y muerte de los médicos a 100 días del estado de emergencia por el COVID-19 en Perú. Acta Médica Peruana (Internet). abril de 2020 (citado 17 de septiembre de 2020);37(2):119-21. Disponible en: http://www.scielo.org.pe/scielo.php?script=sci_abstract&pid=S1728-59172020000200119&lng=es&nrm=iso&tlng=es [ Links ]
16. Ministerio de Salud. Resolución Ministerial N° 448-2020-MINSA: Lineamientos para la Vigilancia, Prevención y Control de la salud de los trabajadores. (Internet). 2020 (citado 17 de septiembre de 2020). Disponible en: https://www.gob.pe/institucion/minsa/normas-legales/744524-448-2020-minsa [ Links ]
17. The Lancet. Redefining vulnerability in the era of COVID-19. Lancet (Internet). 2020 (citado 17 de septiembre de 2020);395(10230):1089. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7270489/ [ Links ]
18. Carrasco-Cortez V. Los trabajadores de salud, los actores olvidados de las reformas. Acta Médica Peruana (Internet). enero de 2014 (citado 17 de septiembre de 2020);31(1):50-6. Disponible en: http://www.scielo.org.pe/scielo.php?script=sci_abstract&pid=S1728-59172014000100009&lng=es&nrm=iso&tlng=es [ Links ]
19. Lancet T. COVID-19: protecting health-care workers. The Lancet (Internet). 21 de marzo de 2020 (citado 18 de septiembre de 2020);395(10228):922. Disponible en: https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)30644-9/abstract [ Links ]
20. Baron S, McPhaul K, Phillips S, Gershon R, Lipscomb J. Protecting Home Health Care Workers: A Challenge to Pandemic Influenza Preparedness Planning. Am J Public Health (Internet). octubre de 2009 (citado 16 de septiembre de 2020);99(Suppl 2):S301-7. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4504355/ [ Links ]
21. Robyn R. M. Gershon MHS, Lori A. Magda MA, Allison N. Canton BA, Halley E. M. Riley BA, Faith Wiggins BA, Wayne Young MBA, et al. Pandemic-related ability and willingness in home healthcare workers. American Journal of Disaster Medicine (Internet). 1 de enero de 2010 (citado 16 de septiembre de 2020);5(1):15-26. Disponible en: https://www.wmpllc.org/ojs/index.php/ajdm/article/view/1966 [ Links ]
22. Sterling MR, Tseng E, Poon A, Cho J, Avgar AC, Kern LM, et al. Experiences of Home Health Care Workers in New York City During the Coronavirus Disease 2019 Pandemic: A Qualitative Analysis. JAMA Intern Med (Internet). 4 de agosto de 2020 (citado 16 de septiembre de 2020); Disponible en: https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2769096 [ Links ]
23. Seto WH, Tsang D, Yung RWH, Ching TY, Ng TK, Ho M, et al. Effectiveness of precautions against droplets and contact in prevention of nosocomial transmission of severe acute respiratory syndrome (SARS). Lancet. 3 de mayo de 2003;361(9368):1519-20. [ Links ]
24. De La Cruz-Vargas JA, De La Cruz-Vargas JA. Protegiendo al personal de la salud en la pandemia Covid-19. Revista de la Facultad de Medicina Humana (Internet). abril de 2020 (citado 14 de septiembre de 2020);20(2):173-4. Disponible en: http://www.scielo.org.pe/scielo.php?script=sci_abstract&pid=S2308-05312020000200173&lng=es&nrm=iso&tlng=es [ Links ]
25. Rivera AS, Akanbi M, O'Dwyer LC, McHugh M. Shift work and long work hours and their association with chronic health conditions: A systematic review of systematic reviews with meta-analyses. PLOS ONE (Internet). 2 de abril de 2020 (citado 16 de septiembre de 2020);15(4):e0231037. Disponible en: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0231037 [ Links ]
26. Vanttola P, Puttonen S, Karhula K, Oksanen T, Härmä M. Prevalence of shift work disorder among hospital personnel: A cross-sectional study using objective working hour data. Journal of Sleep Research (Internet). 2020 (citado 16 de septiembre de 2020);29(3):e12906. Disponible en: https://onlinelibrary.wiley.com/doi/abs/10.1111/jsr.12906 [ Links ]
27. Wang S, Xie L, Xu Y, Yu S, Yao B, Xiang D. Sleep disturbances among medical workers during the outbreak of COVID-2019. Occup Med (Lond) (Internet). 2020 (citado 16 de septiembre de 2020);364-9. Disponible en: https://dx.doi.org/10.1093/occmed/kqaa074 [ Links ]
28. Dugdale CM, Walensky RP. Filtration Efficiency, Effectiveness, and Availability of N95 Face Masks for COVID-19 Prevention. JAMA Intern Med (Internet). 11 de agosto de 2020 (citado 17 de septiembre de 2020); Disponible en: https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2769441 [ Links ]
29. Verbeek JH, Rajamaki B, Ijaz S, Sauni R, Toomey E, Blackwood B, et al. Personal protective equipment for preventing highly infectious diseases due to exposure to contaminated body fluids in healthcare staff. Cochrane Database Syst Rev. 15 de 2020;4:CD011621. [ Links ]
30. Kim M-C, Bae S, Kim JY, Park SY, Lim JS, Sung M, et al. Effectiveness of surgical, KF94, and N95 respirator masks in blocking SARS-CoV-2: a controlled comparison in 7 patients. Infect Dis (Lond). 26 de agosto de 2020;1-5. [ Links ]
31. Sommerstein R, Fux CA, Vuichard-Gysin D, Abbas M, Marschall J, Balmelli C, et al. Risk of SARS-CoV-2 transmission by aerosols, the rational use of masks, and protection of healthcare workers from COVID-19. Antimicrob Resist Infect Control. 06 de 2020;9(1):100. [ Links ]
32. Maltezou HC, Dedoukou X, Tseroni M, Tsonou E, Raftopoulos V, Papadima K, et al. SARS-CoV-2 infection in healthcare personnel with high-risk occupational exposure: evaluation of seven-day exclusion from work policy. Clin Infect Dis (Internet). 29 de junio de 2020 (citado 24 de septiembre de 2020); Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7337654/ [ Links ]
33. Fernández-Maldonado Mujica E. Perú: de la Ley General del Trabajo al Régimen Laboral "Pulpín". Cuadernos del Cendes (Internet). mayo de 2015 (citado 17 de septiembre de 2020);32(89):141-72. Disponible en: http://ve.scielo.org/scielo.php?script=sci_abstract&pid=S1012-25082015000200007&lng=es&nrm=iso&tlng=es [ Links ]
34. Nguyen LH, Drew DA, Graham MS, Joshi AD, Guo C-G, Ma W, et al. Risk of COVID-19 among front-line health-care workers and the general community: a prospective cohort study. The Lancet Public Health (Internet). 1 de septiembre de 2020 (citado 16 de septiembre de 2020);5(9):e475-83. Disponible en: https://www.thelancet.com/journals/lanpub/article/PIIS2468-2667(20)30164-X/abstract [ Links ]
35. Kew H, As V. Economic Vulnerability Among US Female Health Care Workers: Potential Impact of a $15-per-Hour Minimum Wage. Am J Public Health (Internet). 20 de diciembre de 2018 (citado 17 de septiembre de 2020);109(2):198-205. Disponible en: https://europepmc.org/article/med/30571300 [ Links ]
36. Organización Internacional del Trabajo (OIT). Las normas de la OIT y el COVID-19 (coronavirus) (Internet). 2020 (citado 21 de septiembre de 2020). Disponible en: http://www.ilo.org/global/standards/WCMS_739939/lang--es/index.htm [ Links ]
Received: January 13, 2021; Accepted: February 15, 2021











 text in
text in