Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista de la Facultad de Medicina Humana
Print version ISSN 1814-5469On-line version ISSN 2308-0531
Rev. Fac. Med. Hum. vol.21 no.4 Lima Oct./Dec. 2021
http://dx.doi.org/10.25176/rfmh.v21i4.4033
Clinical case
Jaw region endometriosis: Case report
1Hospital General María Auxiliadora. Lima, Perú.
Introduction:
Endometriosis is a chronic gynecological disease, which refers to the presence of endometrial glands and stroma outside the uterine endometrium. This entity has a frequency of 10 to 15% in women of reproductive age, and its most common site of presentation is the ovary. At the extrapelvic level, the most common location is the gastrointestinal and genitourinary location. However, it can occur in any location.
Presentation:
The case of a 40-year-old female patient with a face tumor in the jaw region is described, presenting with a disease time of 2 years. Among the important antecedents, two months before the appearance of the tumor region, the patient underwent endodontic surgery of a lower molar tooth, contiguous to the jaw. Likewise, one month before the appearance of the tumor, the patient underwent an exploratory laparoscopy for electrofulguration of endometriotic foci in the uterine myometrium. The patient underwent a surgical resection of the tumor in the jaw region described; and after reviewing the histological and immunohistochemical slides at the institution, the diagnosis of endometriosis was established.
Conclusion:
Extrapelvic endometriosis is rare in our country, and its diagnosis requires experience and visual training in the recognition of normal endometrial tissue. The presentation of this case was considered important because it would be the first case reported in Peru and in the world, of an endometriosis located in the jaw region.
Keywords: extrapelvic endometriosis; (Source: MeSH Terms).
INTRODUCTION
Endometriosis is a chronic gynecological disease, defined as the presence of normal endometrial tissue, abnormally located in locations other than the uterine endometrium. It is a relatively common entity, whose frequency ranges from 10 to 15% of women at reproductive age, with a peak incidence between 30 and 45 years. Clinically it can manifest with dyspareunia, dysmenorrhea and infertility, although it can also be asymptomatic1,2,3,4.
In general terms, endometriosis can be divided into pelvic and extrapelvic3,5. Regarding pelvic location, the most common location is the ovary in 67%. Other locations that follow in frequency are the fallopian tube, Douglas pouch and pelvic peritoneum1,2.
Extrapelvic endometriosis has been described in many organs, the most frequent locations being the gastrointestinal tract and the genitourinary tract. However, it could be found in virtually any location5. In Peru and worldwide, there are case reports of extrapelvic endometriosis; however, there are no reports of endometriosis in the jaw region. Therefore, it was decided to publish the present clinical case.
CASE REPORT
A case is presented of a 40-year-old female patient with a background of severe episodes of dysmenorrhea due to endometriosis in the uterine myometrium. As surgical background, two months before the appearance of the tumor, the patient had undergone endodontic surgery of a lower right molar tooth, adjacent to the jaw region. One month before the appearance of the tumor, the patient underwent an exploratory laparoscopy for electrofulguration of endometriotic foci located in the uterine myometrium.
Approximately two years ago, the patient noticed in the right jaw region, a small tumor, approximately 0.5 cm on clinical palpation, indurated, which grew progressively until it measured approximately 3 cm. The patient presented intermittent pain in this tumor and the pain intensified mainly with acupressure. The patient also reported more intense symptoms during her menstrual period.
Due to the size and growth of the tumor, the head and neck surgeon decided to perform surgery for its surgical resection, raising as a diagnostic presumption a facial fibroma. Subsequently, the surgical specimen was sent to the anatomic pathology service.
The patient did not undergo any imaging study, since the head and neck surgeon chose to perform the surgery as soon as possible. No serum dosage of any tumor marker was performed either.
On macroscopic evaluation of the surgical specimen, a fragment of tissue with an irregular surface measuring 3x 2.5 x 2.5 x 1.8 cm, light brown in color and firm in consistency was observed. Multiple cuts revealed heterogeneous tissue of whitish brown color alternating with yellowish areas and other areas of dark brown color.
Microscopy showed fibroadipose tissue with presence of glandular structures covered by pseudostratified cylindrical epithelium, some of them dilated and with presence of hemosiderophages in the lumen, surrounded by cellular stroma. With the aforementioned histological findings, Endometriosis was proposed as a probable diagnosis.
Due to the atypical location and for diagnostic support, immunohistochemical studies for Estrogen and Progesterone Receptor (ER/PR) were requested, confirming the suspicion, both immunohistochemical markers were positive for stromal cells and cells of the glandular epithelium, concluding with certainty the diagnosis of Endometriosis.
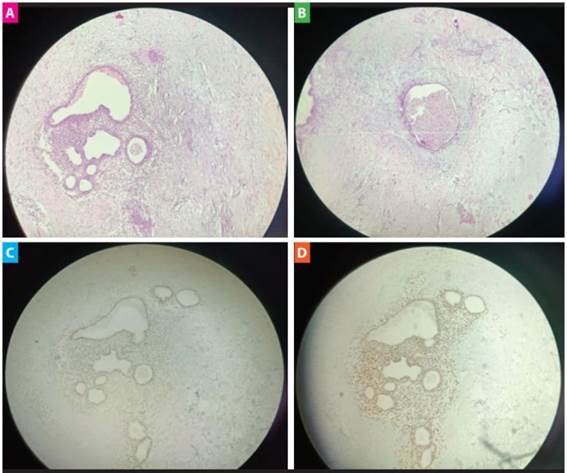
Figure 1: A) Glands with pseudostratified columnar epithelium, surrounded by cellular stroma [Hematoxylin-Eosin] (10x). B) Dilated glands with presence of hemosiderophages in their lumen [Hematoxylin-Eosin] (10x). C) Estrogen receptor (ER) positive in stromal cells and glandular epithelium (10x). D) Progesterone Receptor (PR) Positive in stromal cells and glandular epithelium (10x).
Subsequently, the patient was reevaluated one week after surgery, and reported great clinical improvement. Therefore, it was decided not to prescribe any additional treatment. She did not require any hormonal therapy either.
The patient was clinically stable with no symptoms at 6 months of reevaluation, currently she no longer presents episodes of dysmenorrhea, nor evidence of other tumors in the jaw region.
DISCUSSION
Endometriosis is an estrogen-dependent entity, and is considered to be the most common cause of chronic pelvic pain in women of childbearing age. Because of its estrogen-dependence, it is extremely rare after menopause3. The patient in the present case is 40 years old, which is in accordance with the most frequent age of presentation of this pathology.
Extrapelvic endometriosis is usually a rare condition and is generally associated with delays in diagnosis and significant morbidity5.
Within the extrapelvic locations we find the following, summarized in the table below6:
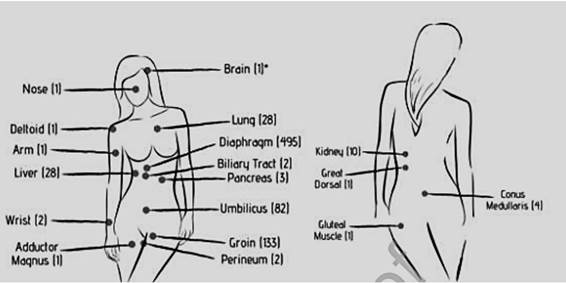
Figure 2: Reported extrapelvic sites of endometriosis (In parentheses, number of cases reported to date)
Endometriosis has a multifactorial etiology. Traditionally, there are three theories that attempt to explain the origin of endometriosis, which are summarized in the following table3,4:
Table 1. Theories about the etiology of endometriosis
| THEORY OF COELOMIC METAPLASIA (OR PERITONEAL METAPLASIA) | Proposed by Meyer in 1903. The development of the disease is the result of a continuous process of differentiation of mesothelial cells of the peritoneal or coelomic tissue, under the effect of inflammatory or hormonal factors, resulting in the formation of groups of cells that will gradually go to a remodeling into endometrial glands and stroma. This theory explains the development of endometriosis in women with Müllerian agenesis, and the development of endometriosis in distant organs. |
| DISPERSION THEORY AND ENDOMETRIAL "TRANSPLANTATION" | The dispersion of endometrial cells through lymphatic vessels was proposed by Halban in 1924. The most accepted theory to date is that of hematogenous spread of endometrial cells, described by Sampson in 1925, who mentioned that retrograde spread of live endometrial cells can occur in the peritoneal cavity and ovaries, during menstruation. In 1952, Javert demonstrated histologically the presence of endometrial tissue in the pelvic veins. This theory attempts to explain the extrapelvic locations of endometriosis. |
| INDUCTION THEORY | Combination of the two previous theories. According to this theory, unknown substances are released from the endometrium and cause transformation of undifferentiated mesenchymal cells to endometrial tissue cells. |
Source: Machairiotis N.; Stylianaki A.; Dryllis G. et al.
In general terms, the most widely accepted theory for the pathogenesis of endometriosis is the theory of ectopic endometrial implantation through retrograde menstruation. Likewise, extrapelvic endometriosis, as in the case of the patient in the present clinical picture, can be explained by migration of endometrial cells through lymphatic and blood vessels3,4.
In this particular case, two important antecedents were found: an electrofulguration surgery of endometriotic foci, and an odontological surgical procedure in a dental piece, close to the area of appearance of the tumor. The odontological procedure stands out mainly because this procedure could have contributed considerably, according to the dispersion theory, to the migration of endometrial cells by hematogenous route to the jaw region.
There are also certain factors that are still under investigation today, and which also seem to be involved in the origin of endometriosis, which are presented below:
Genetics: Daughters or sisters of patients with endometriosis have been observed to have an increased risk of developing the disease. An approximately 10-fold increase in the incidence of the disease has been described in women with an affected first-degree relative. Likewise, studies have found an association of endometriosis with chromosome 10q26 and with the region 7p15.23.
Immunological: There is a possibility that the immune system may not be able to defend itself against a situation of retrograde menstruation. Therefore, it is believed that there may be a causal association between endometriosis and autoimmune diseases, allergic reactions and certain toxins3.
Environmental: It is presumed that environmental factors can cause endometriosis, specifically some plastics and cooking with certain types of plastic containers or microwaves and the effect of dioxin, which can be found as an environmental contaminant in forest fires, and also in animal foods with high fat content. In addition, pesticides and hormones in some foods can also cause hormonal imbalance, and consequently increase the risk of endometriosis3.
Congenital defects: In the case of patients with an atretic hymen, the first menses may remain trapped inside the patient's uterus, increasing the possibility of retrograde menstruation and, therefore, the risk of endometriosis3.
In relation to the histopathological diagnosis of both pelvic and extrapelvic endometriosis, there are the following criteria, and at least 2 of them must be met to establish a definitive diagnosis2.
Table 2. Histopathological criteria for Endometriosis
| HISTOPATHOLOGICAL CRITERIA |
|---|
| ENDOMETRIAL TYPE GLANDS: Müllerian, or endometrial type epithelium; consisting of simple cylindrical or pseudostratified epithelium. Atrophic epithelium may also be seen. May show degenerative atypia (enlarged "fuzzy" nuclei) or metaplasia. |
| ENDOMETRIAL TYPE STROMA: Often contains a fine capillary network. May undergo smooth muscle metaplasia, fibrosis (long-standing), and decidual change. May be myxoid (especially during pregnancy). Stroma may be only one identifiable component, in which case it may be termed stromal endometriosis. |
| EVIDENCE OF CHRONIC BLEEDING Foamy or hemosiderin-laden macrophages (hemosiderophages). |
Source: Han L, García R, Busca A, y Parra-Herran C.
Endometriosis can be diagnosed with well-defined histopathological criteria, as presented inTabla 2 2. In this case report, all these criteria were evidenced, so the final diagnosis of endometriosis was made, in this case, of jaw location.
The immunohistochemical study can be of help in doubtful cases, since the glandular structures express cytokeratin 7 (CK7), estrogen and progesterone receptors (ER/PR), the same immunomarkers that are expressed in normal endometrium7.
Also, in the case of suspected stromal endometriosis, or in the situation where we wish to verify that the stroma we are looking at microscopically corresponds to endometrial stroma, we can use immunohistochemistry for CD10, as well as estrogen receptor (ER), both of which can be useful for marking stromal cells. However, it is important to keep in mind that CD10 is a rather nonspecific marker and that other stromal cells in the female genital tract may also be ER positive1.
Clinically, both pelvic and extrapelvic endometriosis can be confused with any proliferative tumor, benign or malignant. The key to suspecting the diagnosis of endometriosis is to inquire about the patient's clinical history, looking for related symptoms such as dysmenorrhea, dyspareunia and infertility5. In the patient's case, we found dysmenorrhea to be an important symptom.
Taking into account the nature of endometriotic disease and the associated chronic pain, treatment is often a challenge. Endometriosis, being multifactorial and having no defined cause, has a basically empirical treatment8.
Regarding medical treatment, contraceptive pills can be used, since they cause a reduction in the amount of bleeding and thus allow for the reduction of pain during the menstrual period3.
In addition, gonadotropin-releasing hormone (GnRH) agonists may also be used because they block the production of ovarian stimulating hormones, which reduces estrogen levels, and consequently causes endometrial tissue to shrink. GnRH agonists can force endometriosis into remission during the time of treatment and sometimes for months or years afterwards3.
However, medical alternatives that include hormonal suppression have proven to be of limited effectiveness. For this reason, the ideal drug does not yet exist8.
For this reason, medical treatment is usually associated with conservative or non-conservative surgical treatment, depending on the patient's desire to preserve or not her reproductive capacity.
Conservative surgical treatment can include electrofulguration, laser evaporation and thermal coagulation, and can be performed laparoscopically or laparotomy (open surgery)3. Regardless of the surgical technique used, it is important that all endometriotic lesions are adequately removed and all adhesions are carefully cleaned in order to significantly reduce pelvic pain and the risk of infertility in women who wish to preserve their reproductive capacity3.
Non-conservative surgical treatment includes the performance of a total hysterectomy, specifically for those women who already have their parity satisfied8.
Surgical treatment is recommended only when pain cannot be managed medically and quality of life is affected. Surgical treatment is not free of complications, so a series of conditions are required to ensure that the surgery fulfills its main purpose: pain relief8.
In relation to treatment, it is relevant to mention that the patient did not receive hormonal treatment with contraceptives or GnRh analogs at any time, since after the surgery for electrofulguration of endometriotic foci, the episodes of dysmenorrhea decreased considerably.
Likewise, after surgical resection of the tumor in the jaw region, the patient presented significant clinical improvement; therefore, it was decided not to prescribe any complementary treatment.
CONCLUSIONS
Extrapelvic endometriosis is infrequent in our country, and the thought of such diagnosis requires experience and visual training in the recognition of normal endometrial tissue.
This case report is intended to motivate all anatomopathologists to consider the diagnosis of endometriosis whenever we are faced with a patient of reproductive age with a tumor in any location of the body.
Likewise, it is always recommended to make an adequate clinical-pathological correlation in order to establish a properly supported diagnosis, so that a treatment directed to the patient can be offered afterwards.
REFERENCES
1. McCluggage, GT. Endometriosis-related pathology: a discussion of selected uncommon benign, premalignant and malignant lesions. Histopathology 2020, 76, 76-92. DOI: 10.1111/his.13970 [ Links ]
2. Han L, García R, Busca A, Parra-Herran C. Endometriosis. PathologyOutlines.com website.https://www.pathologyoutlines.com/topic/ovarynontumorendometriosis.html. Accessed April 15th, 2021. [ Links ]
3. Machairiotis, N., Stylianaki, A., Dryllis, G. et al. Extrapelvic endometriosis: a rare entity or an under diagnosed condition? Diagn Pathol 2013, 8: 194. https://doi.org/10.1186/1746-1596-8-194 [ Links ]
4. Villena Galarza, MV. Silvers Godoy JP. Silvers Espinosa, JE. Endometrioma subcutáneo en la pared abdominal. A propósito de un caso. Rev Metro Ciencia 2017; 25(1): 20-23. Disponible en: https://docs.bvsalud.org/biblioref/2019/03/986604/metro-junio-out-2017-1-18-21.pdf [ Links ]
5. Mignemi G, Facchini C, Raimondo D, Montanari G, Ferrini G, Seracchioli R. A case report of nasal endometriosis in a patient affected by Behcet's disease. J Minim Invasive Gynecol 2012. Jul-Aug; 19(4):514-6. doi: 10.1016/j.jmig.2012.03.005. PMID: 22748956. [ Links ]
6. Andrés, MP, Arcoverde, FV, Souza, CC, Fernandes, LFC, Abrão, MS y Kho, RM. Endometriosis extrapélvica: una revisión sistemática. Revista de Ginecología Mínimamente Invasiva, 2019. doi: 10.1016 / j. jmig.2019.10.004 [ Links ]
7. Maira González, N., Vidal Santana, F., Castro Sánchez, A., & Pérez Quintela, B. V. Endometriosis cutánea: a propósito de un caso. Progresos de Obstetricia y Ginecología 2013, 56(3), 156-158. doi: 10.1016/j.pog.2012.07.007 [ Links ]
8. Negrón Rodríguez José. Manejo del dolor pélvico crónico en pacientes con endometriosis. Rev. peru. ginecol. obstet. [Internet]. 2016 Ene [citado 2021 Jul 18] ; 62( 1 ): 69-76. Disponible en: http://www.scielo.org.pe/scielo.php?script=sci_arttext&pid=S2304-51322016000100007&lng=es. [ Links ]
Received: July 07, 2021; Accepted: August 09, 2021











 text in
text in 


